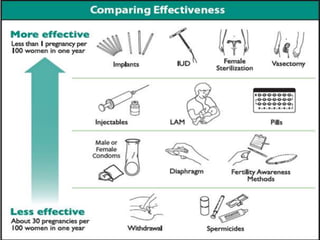
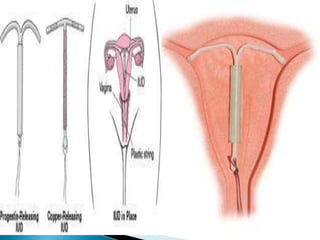
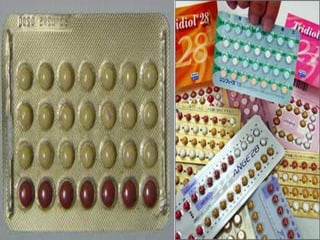
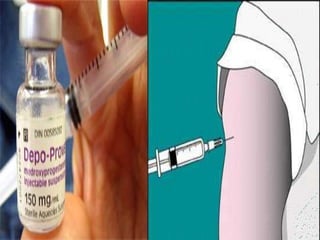
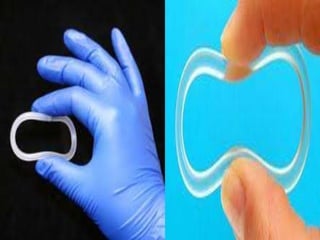
This document discusses various methods of family planning. It describes natural family planning methods like withdrawal and calendar-based methods. It then discusses barrier methods like condoms, diaphragms, and spermicides. Intrauterine devices that contain copper or hormones are explained next. The document also covers hormonal contraceptives like oral contraceptive pills containing estrogen and progestin, and progestin-only pills, implants, and injectables. Advantages and disadvantages are provided for many of the methods.