Drugs acting on the GI system include:
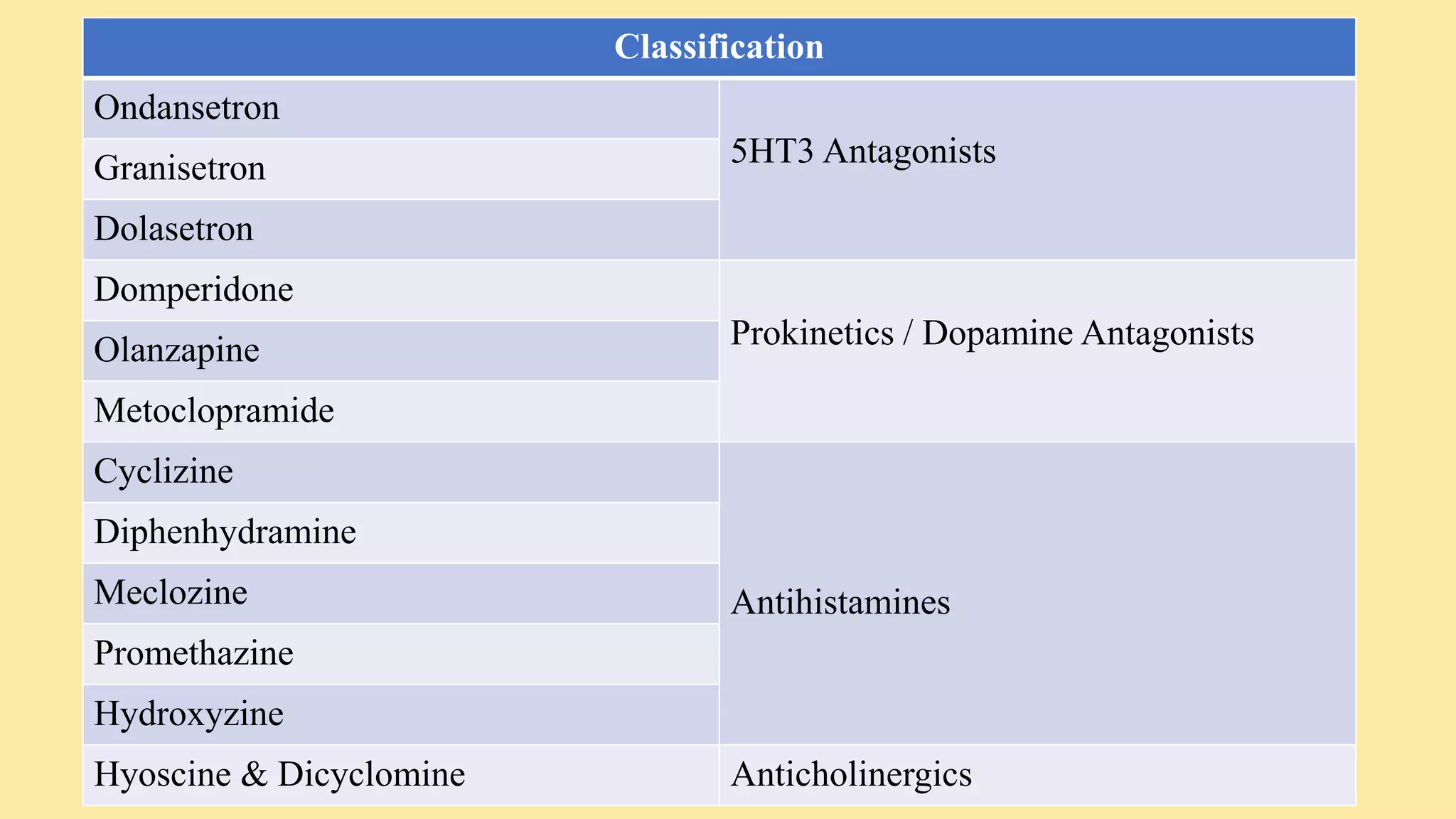
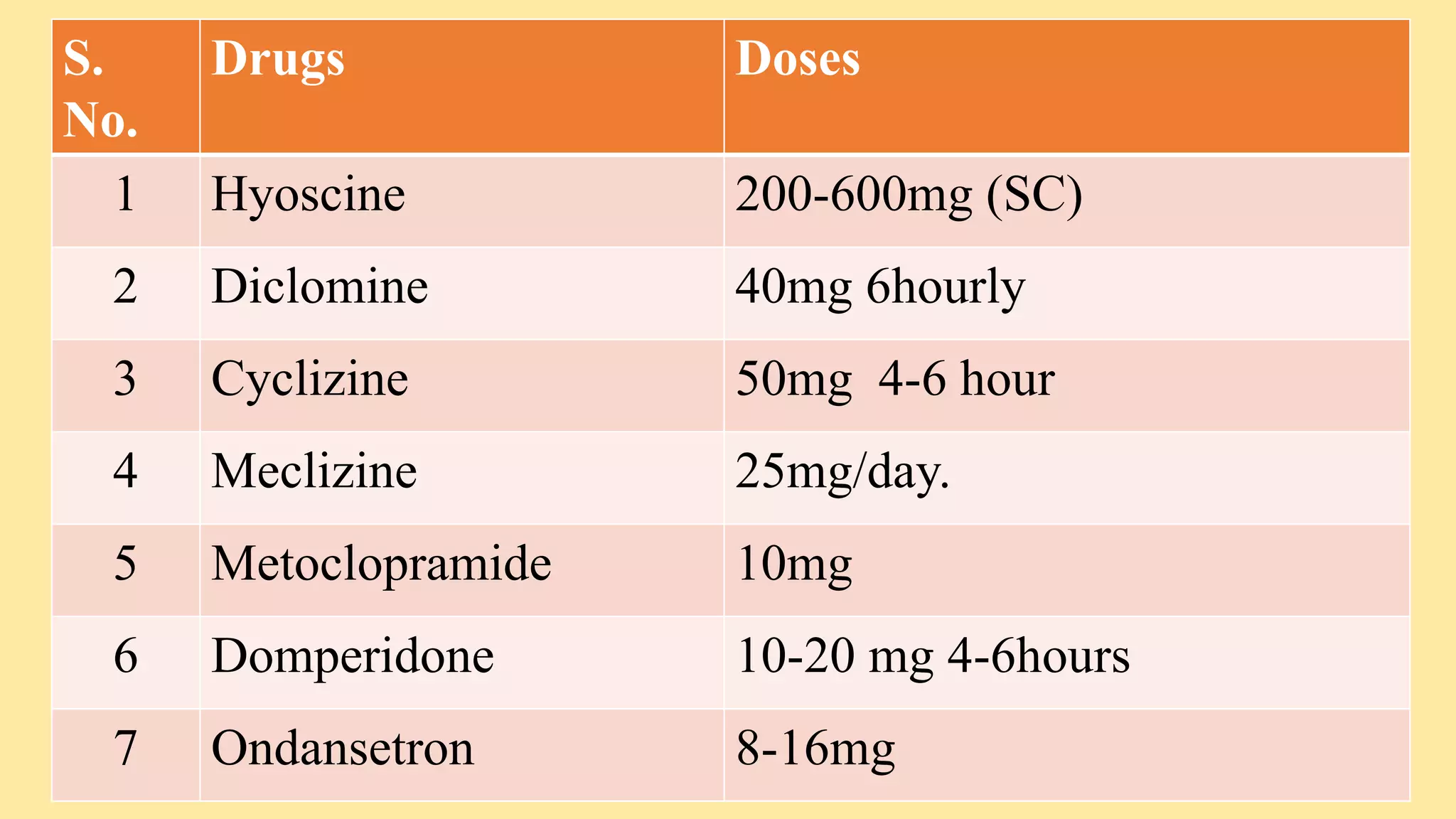
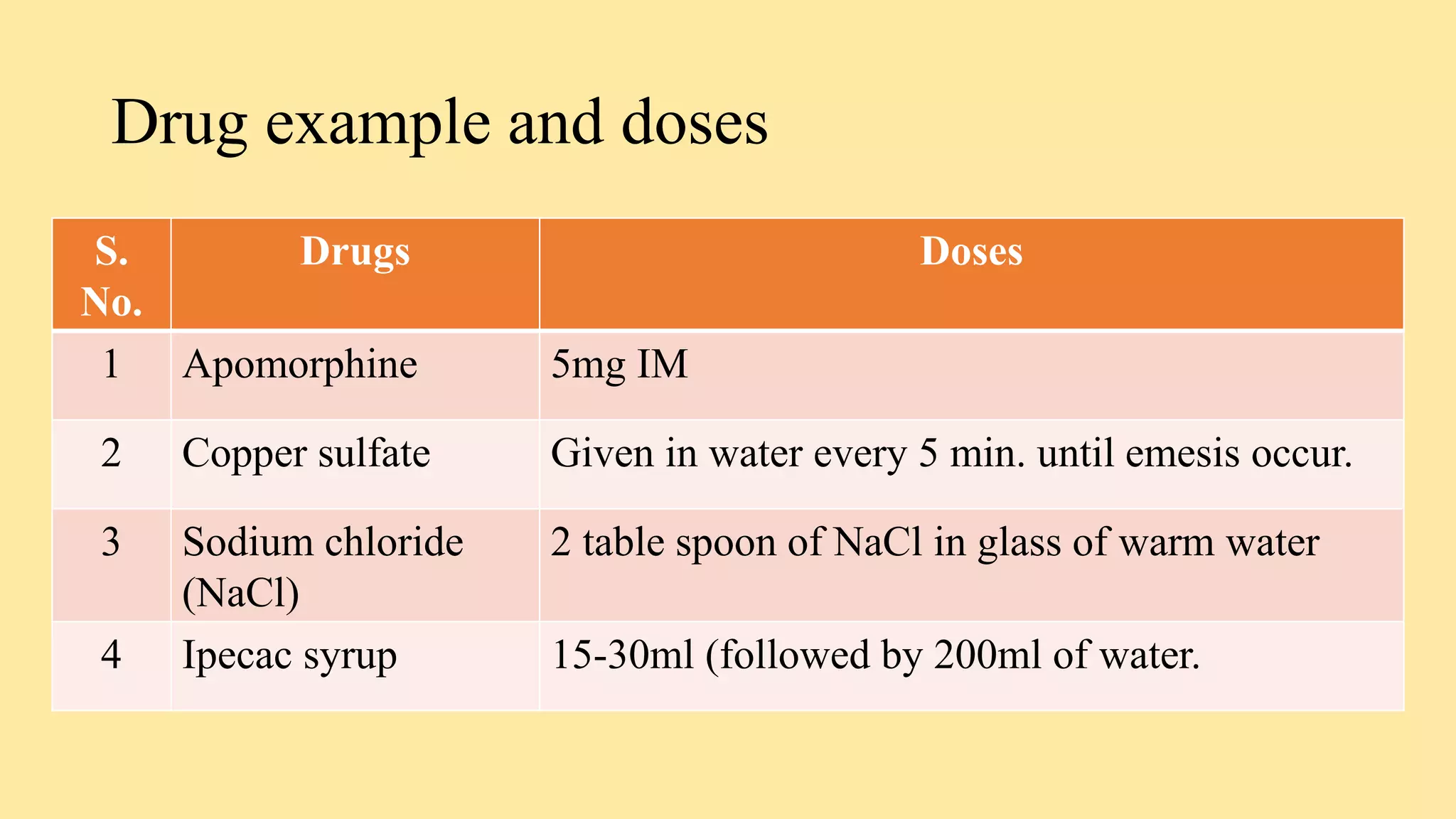
- Antiemetics which prevent nausea and vomiting like ondansetron and metoclopramide.
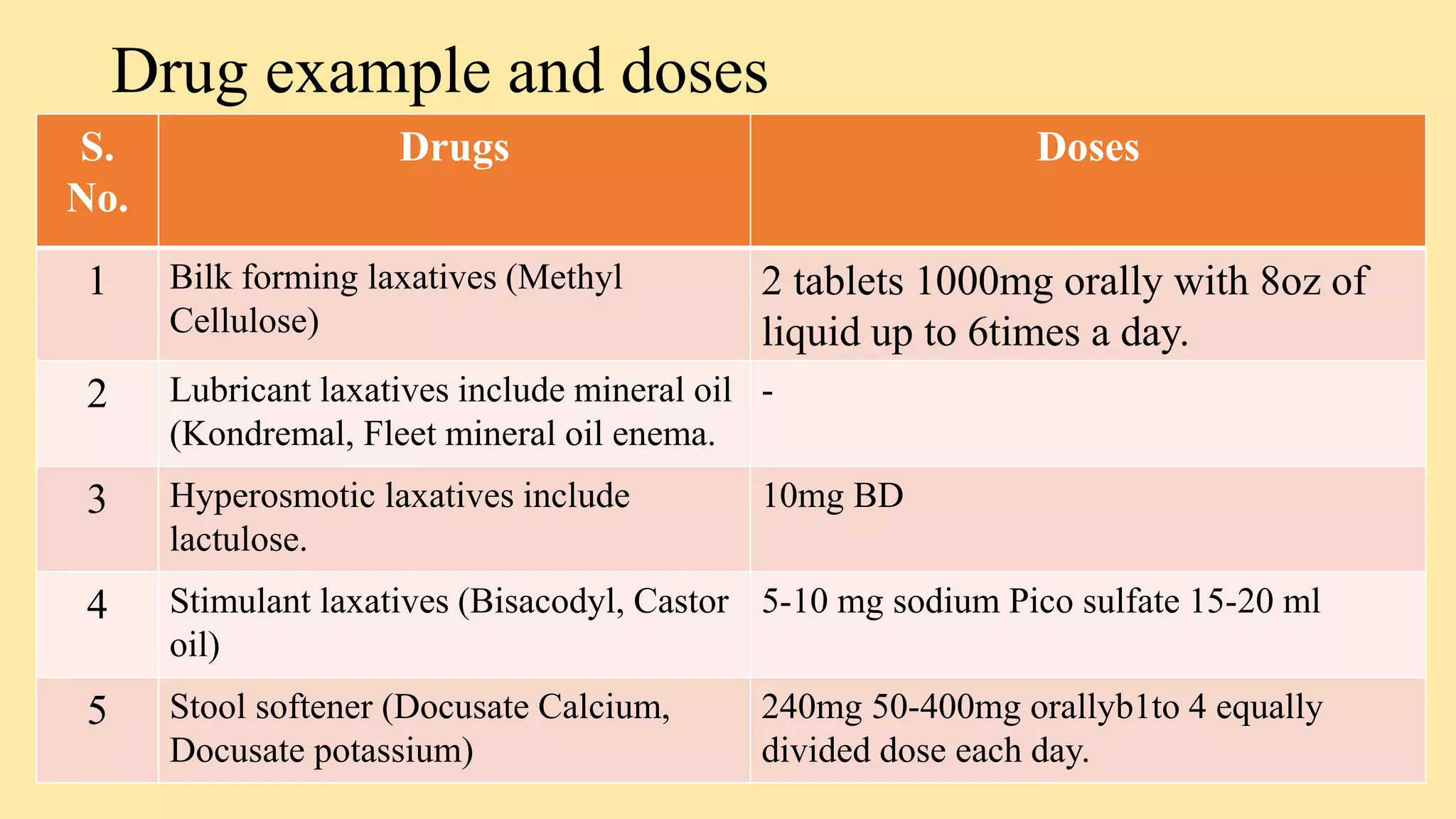
- Laxatives and purgatives like lactulose, bisacodyl, and docusate which are used to treat constipation.
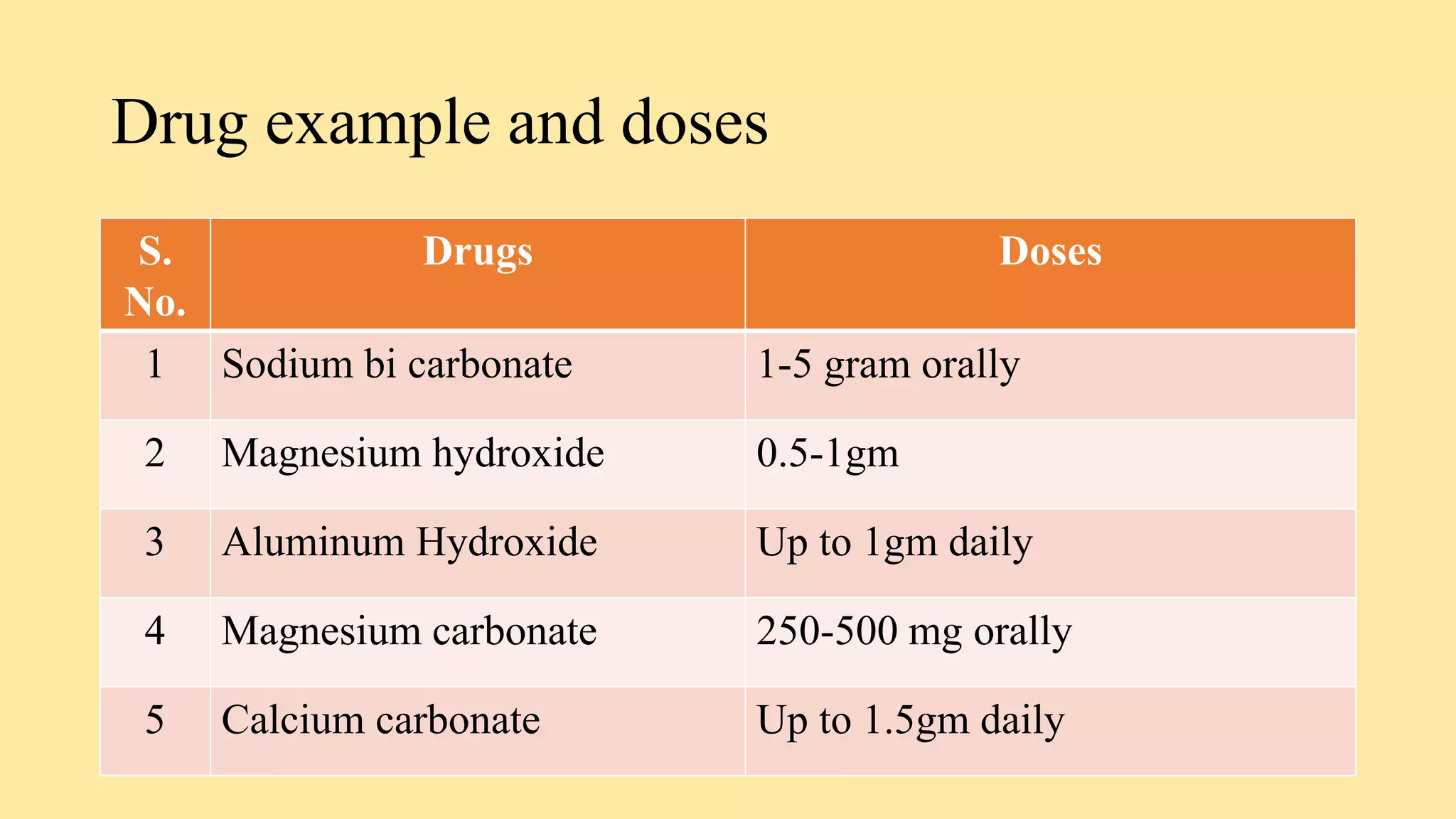
- Antacids such as aluminum hydroxide, magnesium hydroxide, and calcium carbonate which neutralize stomach acid.
- Cholinergic drugs which increase GI motility and secretions. Anticholinergic drugs block acetylcholine and decrease motility and secretions.