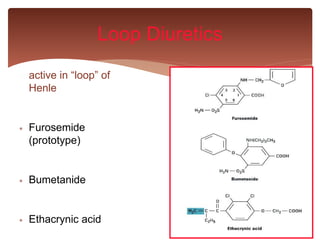
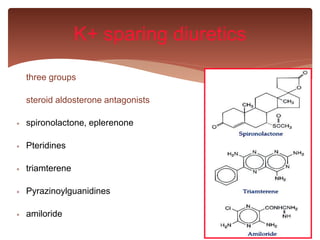
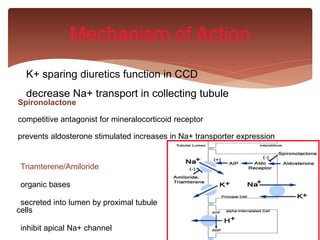
This document discusses different classes of diuretic drugs, including their sites of action in the nephron, mechanisms of action, therapeutic uses, and side effects. It covers osmotic diuretics, carbonic anhydrase inhibitors, thiazide diuretics, loop diuretics, and potassium-sparing diuretics. The main points are that diuretics work by inhibiting transport in different parts of the nephron like the proximal tubule, loop of Henle, or distal convoluted tubule. They are used to treat conditions like edema, hypertension, and heart failure. Common side effects among the classes include electrolyte imbalances and metabolic alterations.




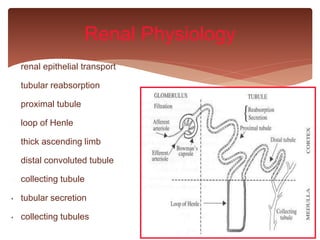




![ inhibits carbonic anhydrase in renal
proximal tubule cells
carbonic anhydrase catalyzes
formation of HCO3- and H+ from H2O
and CO2
inhibition of carbonic anhydrase
decreases [H+] in tubule lumen
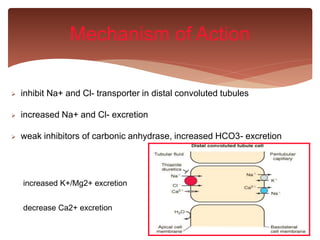
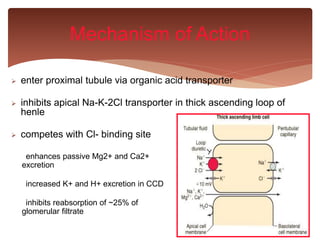
Mechanism of Action
less H+ for for Na+/H+ exchange
increased lumen Na+, increased H2O
retention](https://image.slidesharecdn.com/diuretics-160908094819/85/Diuretics-15-320.jpg)
![ used to treat chronic open-angle glaucoma
aqueous humor has high [HCO3-]
acute mountain sickness
prevention and treatment
metabolic alkalosis
sometimes epilepsy
mostly used in combination with other diuretics in resistant
patients
Therapeutic Uses](https://image.slidesharecdn.com/diuretics-160908094819/85/Diuretics-16-320.jpg)









![ hyperkalemia: monitor plasma [K+]
spironolactone: gynecomastia
triamterene: megaloblastic anemia in cirrhosis patients
amiloride: increase in blood urea nitrogen, glucose
intolerance in diabetes mellitus
Side Effects](https://image.slidesharecdn.com/diuretics-160908094819/85/Diuretics-32-320.jpg)
