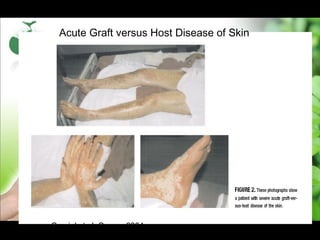
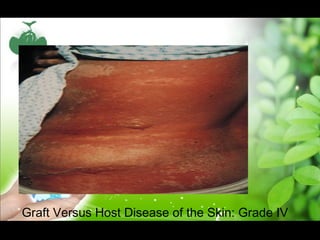
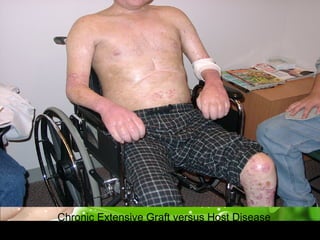
There are three main types of bone marrow transplants - autologous using the patient's own cells, and allogeneic using cells from a sibling or unrelated donor. Cells can come from bone marrow, peripheral blood stem cells, or umbilical cord blood. The transplant process involves a conditioning phase to eliminate disease and immune cells, stem cell infusion, a neutropenic phase with no immune system, engraftment as the immune system recovers, and a long-term post-engraftment period. Complications can include graft-versus-host disease where donor cells attack host tissues, infections during the neutropenic phase, and other organ toxicities.