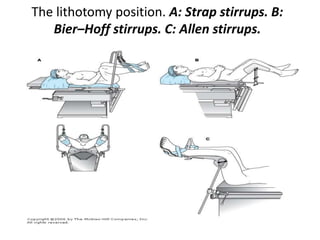
This document provides information about anesthesia for genitourinary surgeries and procedures. It discusses considerations for cystoscopy, transurethral resection of the prostate (TURP), lithotripsy, and the lithotomy position. Regional or general anesthesia is typically used depending on the procedure and patient factors. Complications of TURP can include hemorrhage, TURP syndrome from fluid absorption, bladder perforation, hypothermia, septicemia, and disseminated intravascular coagulation. Careful monitoring is important to detect issues like fluid overload and hyponatremia.




















![c
• The hypotonicity of these fluids also results in
acute hyponatremia and hypoosmolality, which
can lead to serious neurological manifestations .
• Symptoms of hyponatremia usually do not
develop until the serum sodium concentration
decreases below 120 mEq/L.
• Marked hypotonicity in plasma ([Na+] < 100
mEq/L) may also result in acute intravascular
hemolysis.](https://image.slidesharecdn.com/anesthesiaforgenitourinarysurgery-230614183351-1e056e98/85/Anesthesia-for-Genitourinary-Surgery-pptx-22-320.jpg)































![Suggested Reading
• Battillo JA, Hendler MA: Effects of patient
positioning during anesthesia.
• In: Anesthesia for Urological Surgery.
• Lebowitz RW (editor). Int Anesthesiol Clin
1993;31:67. [PMID: 8440533]
• Dobson PM, Caldicott LD, Gerrish SP, et al:
Changes in hemodynamic variables during
transurethral resection of the prostate:
Comparison of general and spinal anaesthesia.
• Br J Anaesth 1994;72:267. [PMID: 8130043](https://image.slidesharecdn.com/anesthesiaforgenitourinarysurgery-230614183351-1e056e98/85/Anesthesia-for-Genitourinary-Surgery-pptx-56-320.jpg)
