Anatomy and physiology of thyroid gland
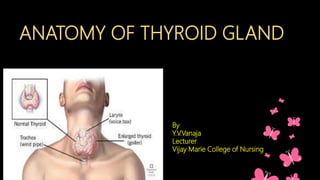
- 1. Anatomy of Thyroid Gland It is an endocrine gland situated in the lower part of the front and sides of the neck ANATOMY OF THYROID GLAND By Y.V.Vanaja Lecturer Vijay Marie College of Nursing
- 2. It is an endocrine gland, situated in the lower part of the front and sides of the neck, located just inferior to the larynx. Butterfly shaped thyroid gland Extends : from oblique line of thyroid cartilage to the 5th and 6th tracheal ring. lie against C5,C6,C7 & T1 It composed of right and left lobes on either side of the trachea, that is connected by an isthmus anterior to the trachea.. about 50% thyroid glands have a small 3rd lobe – pyramidal lobe. It extends superiorly from the isthmus the normal mass of the thyroid is 30g THYROID GLAND
- 4. The lobes are conical in shape having: • An apex • A base • Three surfaces: Lateral, medial, posterolateral Two borders: Anterior and posterior Apex: • directed upwards and slightly laterally. Base: on level with the 4th or 5th trachealring. RELATIONS OF THE LOBES
- 6. Blood supply: • Superior and inferior thyroid arteries. • Superior, middle and inferior thyroid veins. Lymphatic drainage: • Upper & lower deep cervical lymph node • Pretracheal and paratracheal lymph node Nerve supply: • Middle cervical ganglion • Superior and inferior cervical ganglia
- 9. Nerve supply
- 10. Microscopic spherical sacs called thyroid follicles make up most of the thyroid gland The wall of each follicle consists primarily of cells called follicular cells most of which extend to the lumen of the follicle A basement membrane surrounds each follicle When the follicular cells are inactive , their shape is low cuboidal to squamous, but under the influence of TSH they become active in the secretion and range from low cuboidal to low columnar shape The follicular cells produce 2 hormones triiodothyronine (T3) and tetraiodothyronine (T4) T3 and T4 are together called thyroid hormones. A few cells called para follicular cells or C cells lies between follicles they produce the hormone calcitonin. HISTOLOGY
- 12. PHYSIOLOGY OF THYROID GLAND
- 13. The thyroid gland is the only endocrine gland that stores its secretory product in large quantities – normally about a 100 - day supply. Synthesis and secretion of T3 and T4 occurs as follows 1) Iodide trapping 2) Synthesis of thyroglobulin 3) Oxidation of iodide 4) Iodination of tyrosine 5) Coupling of T1 and T2 6) Pinocytosis and digestion of colloid 7) Secretion of thyroid Hormones 8) Transport in the Blood
- 14. 1) Iodide trapping; Thyroid follicular cells trap iodide ions by actively transporting them from the blood into the cytosol 2) Synthesis of Thyroglobulin; while follicular cells are trapping iodide they are also synthesizing thyroglobulin (TGB) • Produced in the – rough endoplasmic reticulum • Modified in – Golgi complex • Packed into secretory vesicles - undergo exocytosis, releases TBG into the lumen of the follicle 3) Oxidation of Iodide: • Some of the aminoacids in TGB are tyrosines that will become iodinated • As the iodide ions are being oxidized, they pass through the membrane into the lumen of the follicle
- 15. 4) Iodination of tyrosine; • As iodine molecules I2 form they react with tyrosines that are part of thyroglobulin molecules. • Binding of one iodine yields Monoiodothyrosine (T1) and a second iodination produces diiodotyrosine (T2) • TGB with attached iodine atoms , a sticky material that accumulates and is stored in the lumen of the thyroid follicle, is termed colloid . 5)Coupling of T1 and T2 ; • Two T2 molecules join to form T4 or T1 and one T2 join to form T3 6) Pinocytosis & digestion of colloid ; • Droplets of colloid reenter follicular cells by pinocytosis and merge with lysosomes • Digestive enzymes in the lysosomes break down TGB, Cleaving off molecules of T3 and T4 7) Secretion of Thyroid hormones; Because T3 and T4 are lipid soluble, they diffuse through the plasma membrane into interstitial fluid and then into the blood
- 16. • T4 normally is secreted in greater quantity than T3, but T3 is several times more potent. • Moreover after T4 enters a body cell, most of it is converted to T3 by removal of one iodine. 8) Transport in the blood ; more than 99% of both the T3 and the T4 combine with transport proteins in the blood , mainly Thyroxine- binding globulin(TGB)
- 17. Steps in the synthesis of thyroid hormones
- 19. Because most body cells have receptors for thyroid hormones, T3 and T4 exert their effects throughout the body 1. Thyroid hormones increase BMR, the rate of oxygen consumption under standard or basal conditions, by stimulating the use of cellular O2 to produce ATP • When the BMR increases, cellular metabolism of CHO, lipids and proteins increases 2. A second major effect of thyroid hormones is to stimulate synthesis of additional sodium- potassium pumps, which use large amount of ATP to continually eject the sodium ions from the cytosol into the extracellular fluid and potassium ions from the extracellular fluid into the cytosol. • As the cells produce and use more ATP, more heat is given off, and body temperature rises. • This phenomenon is called the calorigenic effect. • Thyroid Hormone – maintains normal body temperature Actions of Thyroid Hormones
- 20. 3. In the regulation of metabolism, thyroid hormones stimulate protein synthesis and increase the use of glucose and fatty acids for ATP production. • They also increase lipolysis and enhance cholesterol excretion, thus reducing blood cholesterol level. 4. the thyroid hormones enhance some actions of the catecholamines because they up-regulate beta receptors. • For this reason symptoms of hyperthyroidism include increased HR, more forceful heartbeats, & increased BP • 5. Together with the growth hormone and insulin, thyroid hormone accelerate body growth of the nervous & skeletal systems. • Deficiency of the thyroid hormone during fetal development, infancy, or childhood causes severe MR and stunted bone growth
- 21. Thyrotropin releasing hormone from the hypothalamus and TSH from the anterior pituitary stimulate synthesis and release of thyroid hormones Low blood levels of T3 and T4 or low metabolic rate stimulates the hypothalamus to secrete TRH TRH enters the hypophyseal portal veins and flows to the anterior pituitary , where it stimulate thyrotrophs to secrete TSH TSH stimulates virtually all aspects of thyroid follicular cell activity, and growth of the follicular cells Thyroid follicular cells release T3 and T4 into the blood until the metabolic rate returns to normal An elevated level of T3 inhibits release of TRH and TSH Regulation of secretions and actions of thyroid Hormones
- 23. Conditions thyroid hormones hat increase ATP demand- a cold environment, Hypoglycemia, high altitude, and pregnancy also increase the secretion of thyroid hormones Calcitonin: The hormone produced by parafollicular cells of the thyroid gland is calcitonin CT decrease the level of calcium in the blood by inhibiting the action of osteoclasts. The secretion of CT is controlled by negative feedback system When the blood level is high, calcitonin lowers the amount of blood calcium and phosphates by inhibiting the bone resorption by osteoclast and accelerating uptake of calcium and phosphates into bone extracellular matrix
Editor's Notes
- HISTOLOGY
- FORMATION, STORAGE AND RELEASE OF THYROID HORMONES