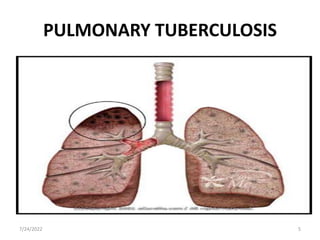
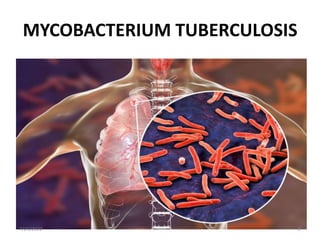
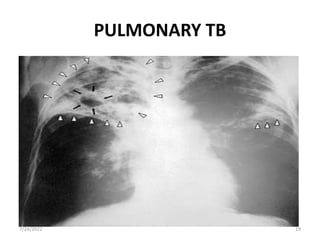
This document provides an overview of pulmonary tuberculosis, including its definition, classification, types, incidence, risk factors, pathophysiology, signs and symptoms, diagnosis, treatment, nursing management, and complications. It classifies TB based on anatomical site, previous treatment history, and drug resistance. Key points include that TB is caused by the bacterium Mycobacterium tuberculosis and spreads through airborne droplets. Diagnosis involves chest x-rays, sputum smears and cultures, tuberculin skin tests, and interferon-gamma blood tests.





























































![Contd....
–Risk for impaired gas exchange related to
destruction of alveolar-capillary membrane,
thick, viscous secretions or Bronchial edema.
–Infection, risk for [spread/reactivation] related
to inadequate primary defense, decreased
cilliary action/stasis of secretions or extension
of infection, lowered resistance or
malnutrition.
75
7/24/2022](https://image.slidesharecdn.com/1-220724172006-e6be70a7/85/PULMONARY-TUBERCULOSIS-75-320.jpg)