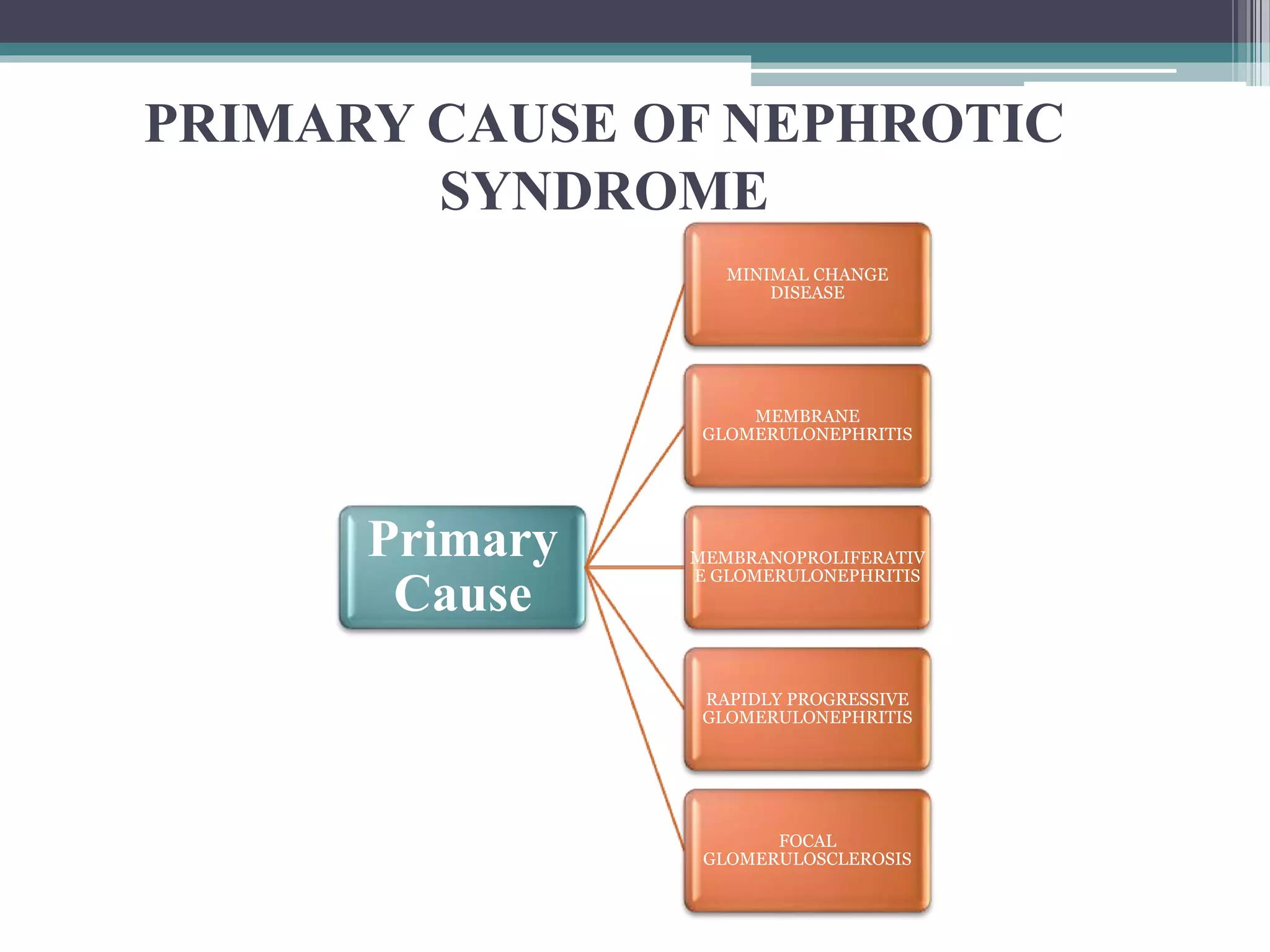
Nephrotic syndrome is a kidney disorder characterized by protein in the urine, low blood albumin levels, high blood lipids, and swelling. It is caused by damage to the glomerular capillary membrane in the kidney. Clinically, it presents with edema, proteinuria, hyperlipidemia, and hypoalbuminemia. Treatment involves fluid restriction, diuretics, corticosteroids, and ACE inhibitors to control symptoms and manage complications like infection, atherosclerosis, and renal failure. Prognosis depends on the underlying cause, with minimal change disease having a good prognosis if it responds to steroids.










![PATHOPHYSIOLOGY
LOSS OF PLASMA PROTEIN [ ALBUMIN]
DUE TO CAUSES- DAMAGE GLOMERRULAR CAPILLARY MEMBRANE
STIMULATES SYNTHESIS OF
LIPOPROTEIN
HYPERLIPIDEMIA
HYPOALBUMINEMIA
GENERALIZED OEDEMA
ACTIVATION OF RENIN ANGIOTENSIN SYSTEM
SODIUM RETENTION
EDEMA
DECREASE OSMOTIC PRESSURE
FLUID MOVES FROM IVS TO ECS](https://image.slidesharecdn.com/nephroticsyndrome-190707163748/75/Nephrotic-syndrome-By-Sachin-Dwivedi-13-2048.jpg)












