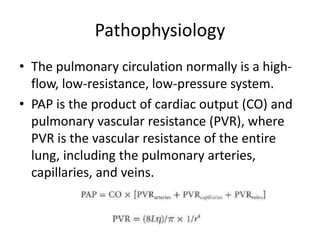
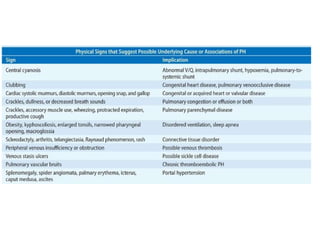
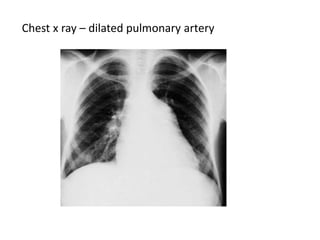
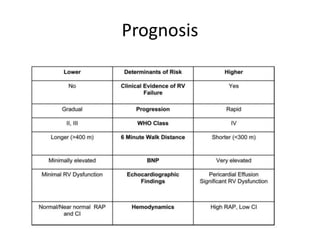
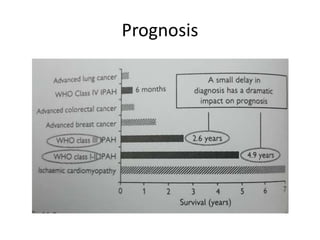
- Pulmonary artery hypertension (PAH) is defined as a mean pulmonary artery pressure of ≥25 mmHg at rest. It is characterized by pre-capillary pulmonary hypertension with a pulmonary wedge pressure <15 mmHg and a pulmonary vascular resistance >3 Wood units.
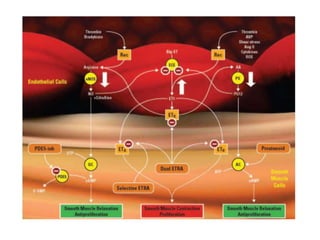
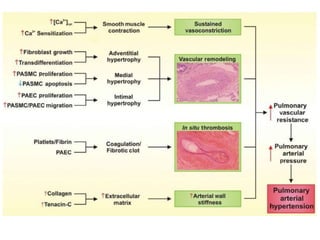
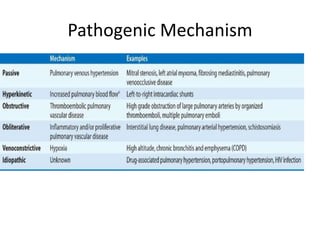
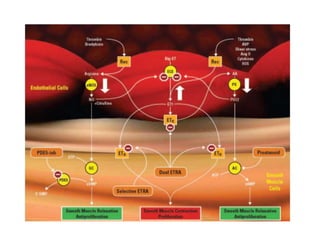
- The pathophysiology involves sustained vasoconstriction, vascular remodeling, in situ thrombosis, and increased arterial stiffness. Genetic factors like BMPR2 mutations also contribute to PAH development.
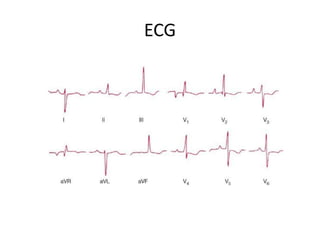
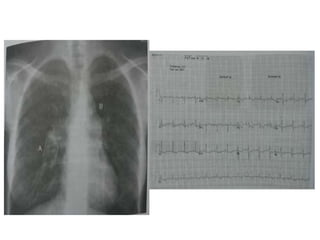
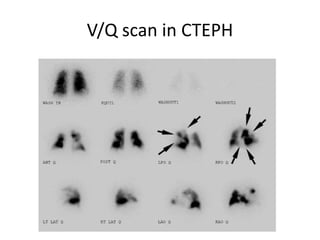
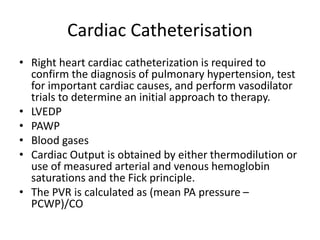
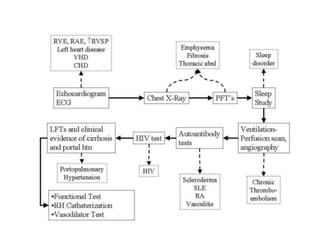
- Clinical features range from mild breathlessness to signs of right heart failure. Diagnostic tests include echocardiography, CT scans, V/Q scans, right heart catheterization and lab tests.
- Treatment involves oxygen therapy, diure