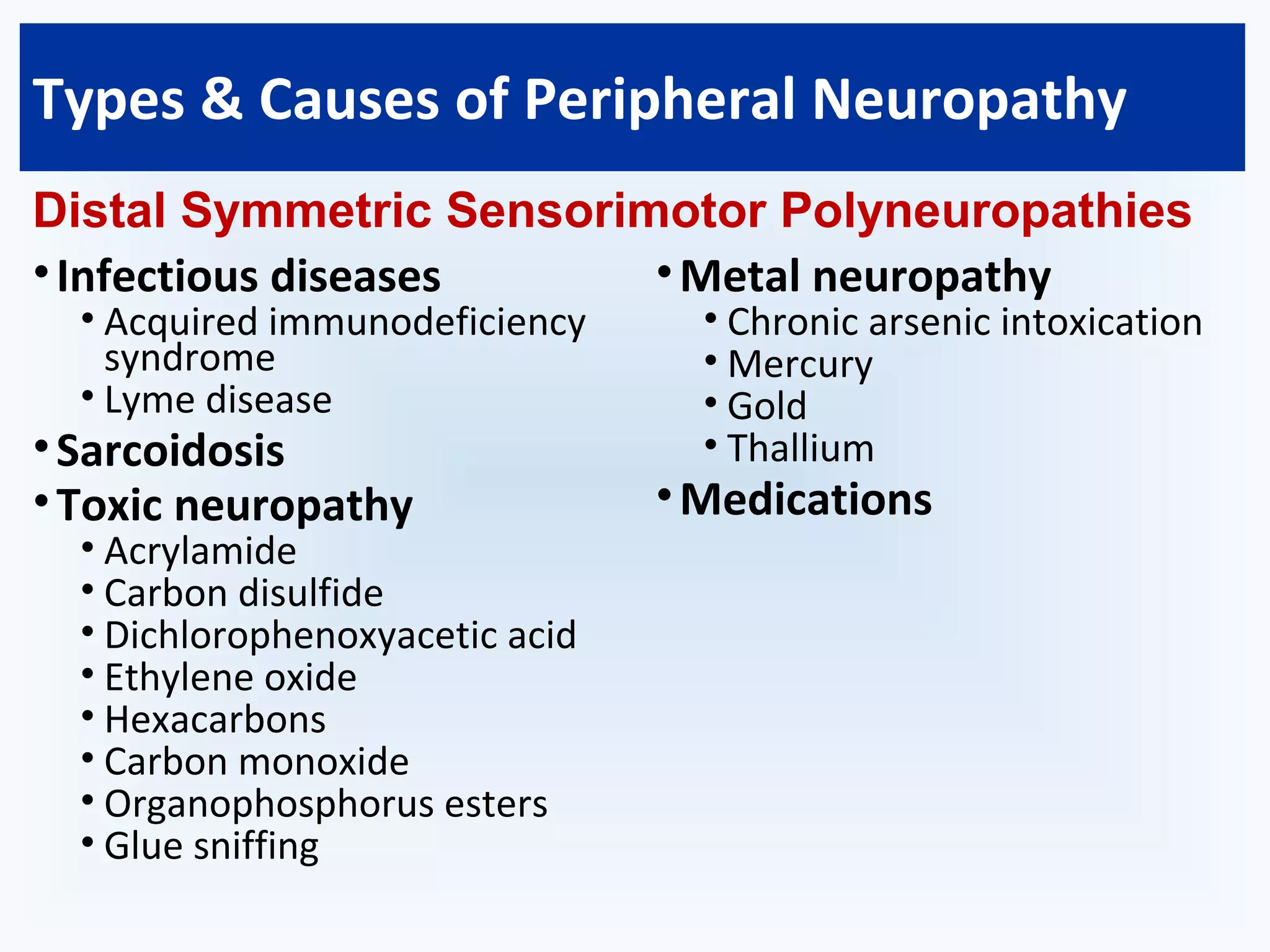
Peripheral neuritis, or peripheral neuropathy, is damage to nerves in the peripheral nervous system caused by diseases of the nerves or systemic illness. The peripheral nervous system consists of cranial and spinal nerves and contains motor, sensory, and autonomic nerves. Peripheral neuropathy can be classified based on the number, type, or process affecting nerves and may be caused by diseases like diabetes, infections, toxins, and medications. Physical exams can reveal motor and sensory signs while electrodiagnostic tests help evaluate the type and pattern of nerve involvement. Treatment involves managing underlying causes, relieving symptoms, and mechanical aids or surgery for specific nerve damage.