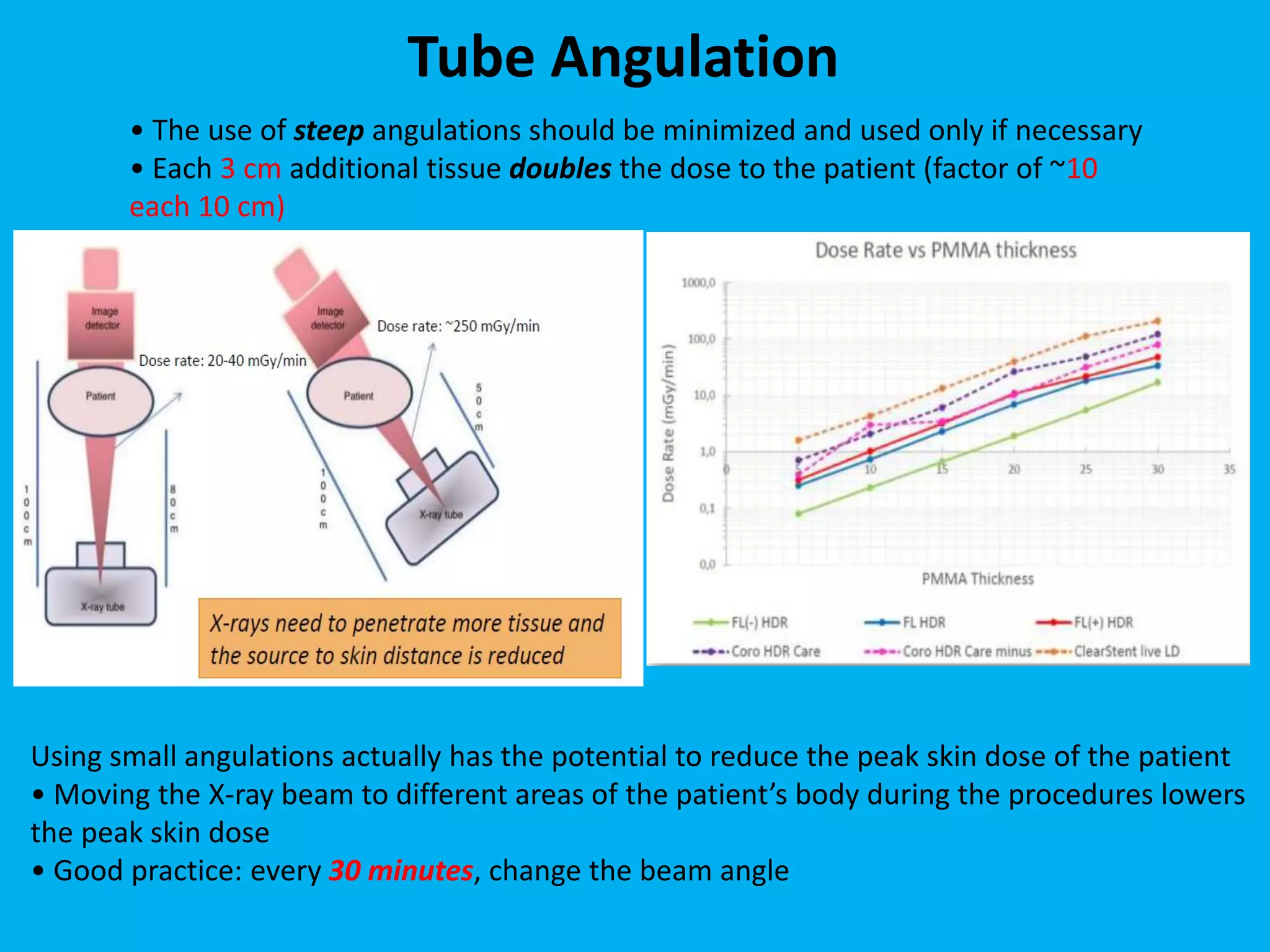
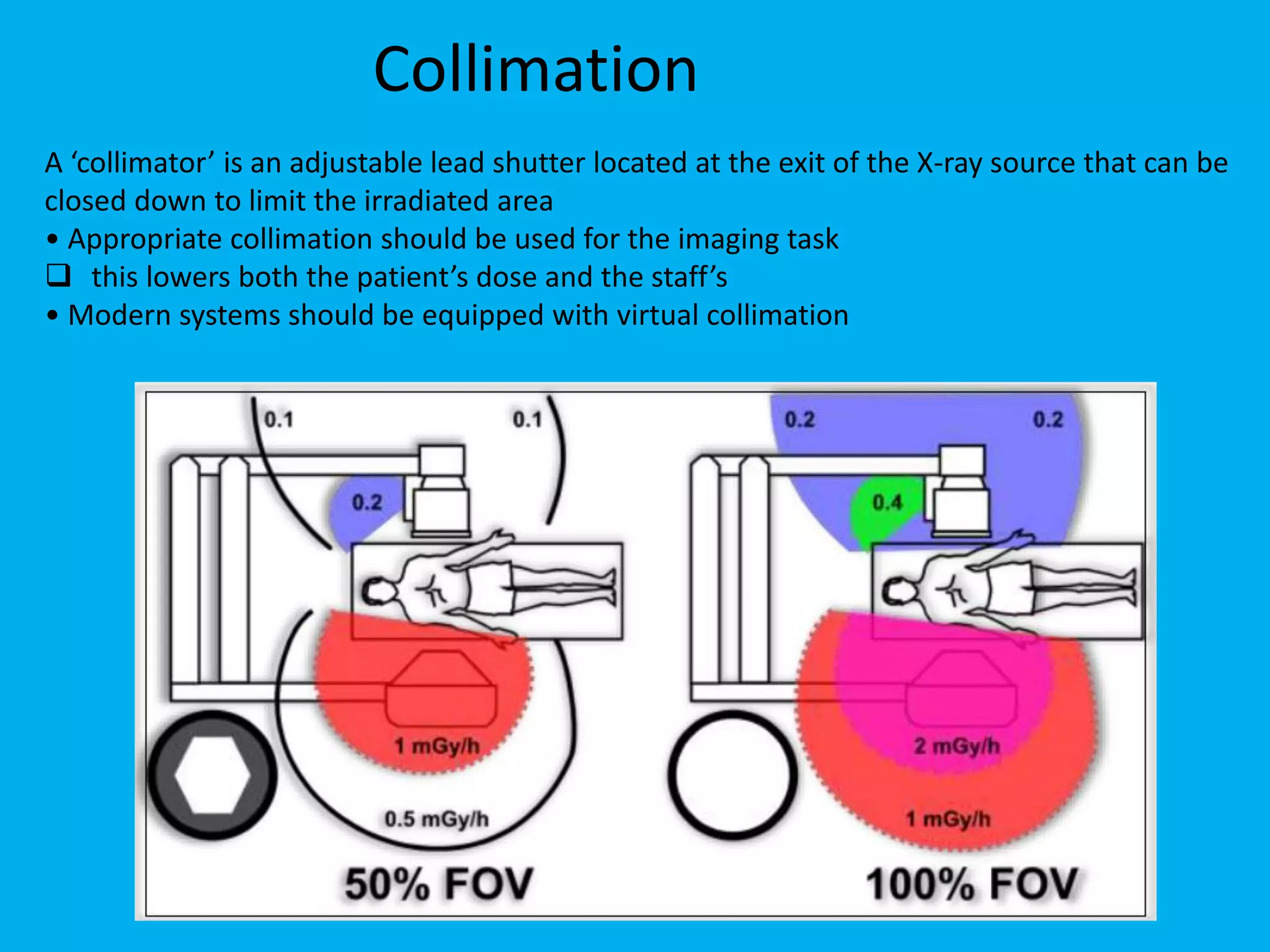
This document discusses patient dose management in angiography procedures. It defines key radiation terms like exposure, absorbed dose, equivalent dose and effective dose. It explains radiation units like Gray, Sievert and Dose Area Product. Factors influencing patient dose like equipment settings, patient positioning, tube angulation, magnification and collimation are described. Methods to minimize dose like reducing beam-on time, increasing source-to-patient distance and using automatic exposure control are provided. The use of diagnostic reference levels to promote radiation dose optimization is also summarized.