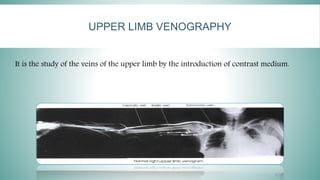
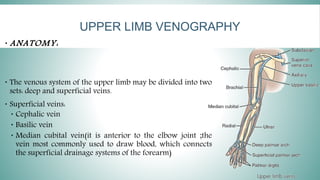
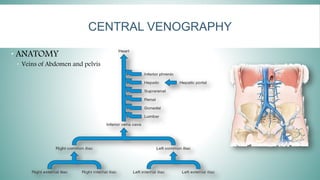
Angiography is a specialized radiologic imaging technique for visualizing blood vessels after injecting contrast media. The procedure involves a team of health professionals and requires specifically designed angiographic rooms and advanced imaging equipment. Various types of venography, such as peripheral and central venography, are performed to diagnose conditions like deep venous thrombosis, with specific patient preparation and contraindications outlined.