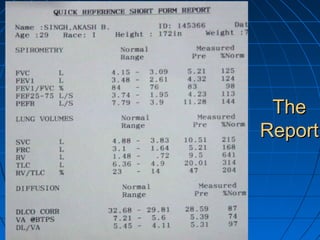
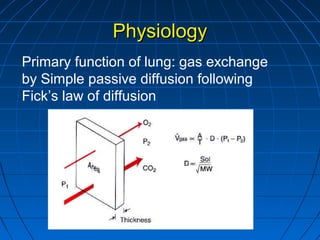
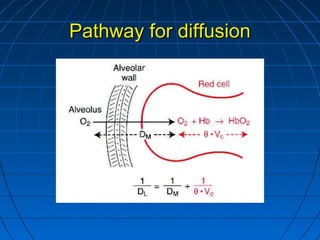
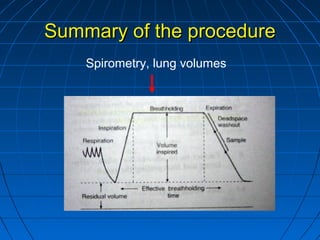
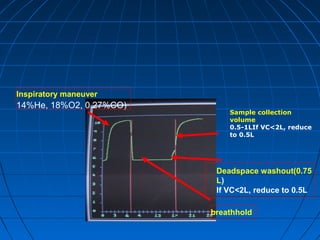
The document discusses diffusion capacity of the lungs, including the physiology of gas diffusion through the lungs, terminology used, methods of measuring diffusion capacity, and factors that affect diffusion capacity. It provides details on the single-breath method for measuring diffusion capacity, including procedures, acceptability criteria, calculations, and potential sources of error. Diseases that may increase or decrease diffusion capacity are also summarized.