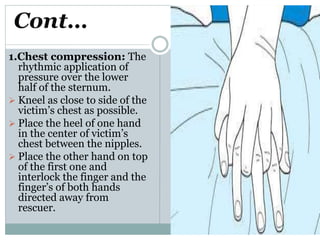
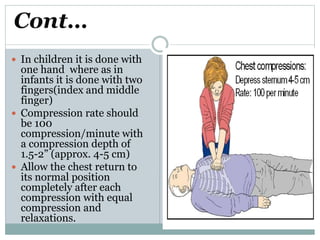
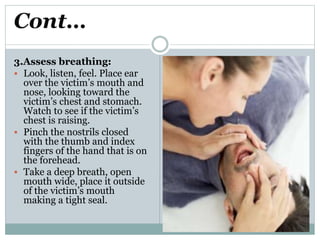
CPR involves chest compressions and assisted ventilation to restore circulation and prevent brain damage from lack of oxygen in someone experiencing cardiopulmonary arrest. It consists of basic life support provided by any first responder and advanced life support involving intubation, defibrillation, and drugs. The procedure for CPR involves checking responsiveness, feeling for a pulse, clearing the airway, giving chest compressions at a rate of 100 per minute to a depth of 1.5-2 inches, and rescue breaths at 10-12 breaths per minute until spontaneous circulation returns.