The document provides guidance on performing various cardiac MRI sequences and views, including how to obtain basic views like the 2 chamber, 4 chamber, and short axis views. It also discusses considerations for special sequences like velocity encoded phase contrast imaging to quantify flow and gadolinium enhanced MRA. Advanced cardiac MRI tools are also outlined, such as myocardial perfusion imaging, tagging for wall motion analysis, and viability assessment with delayed enhancement.
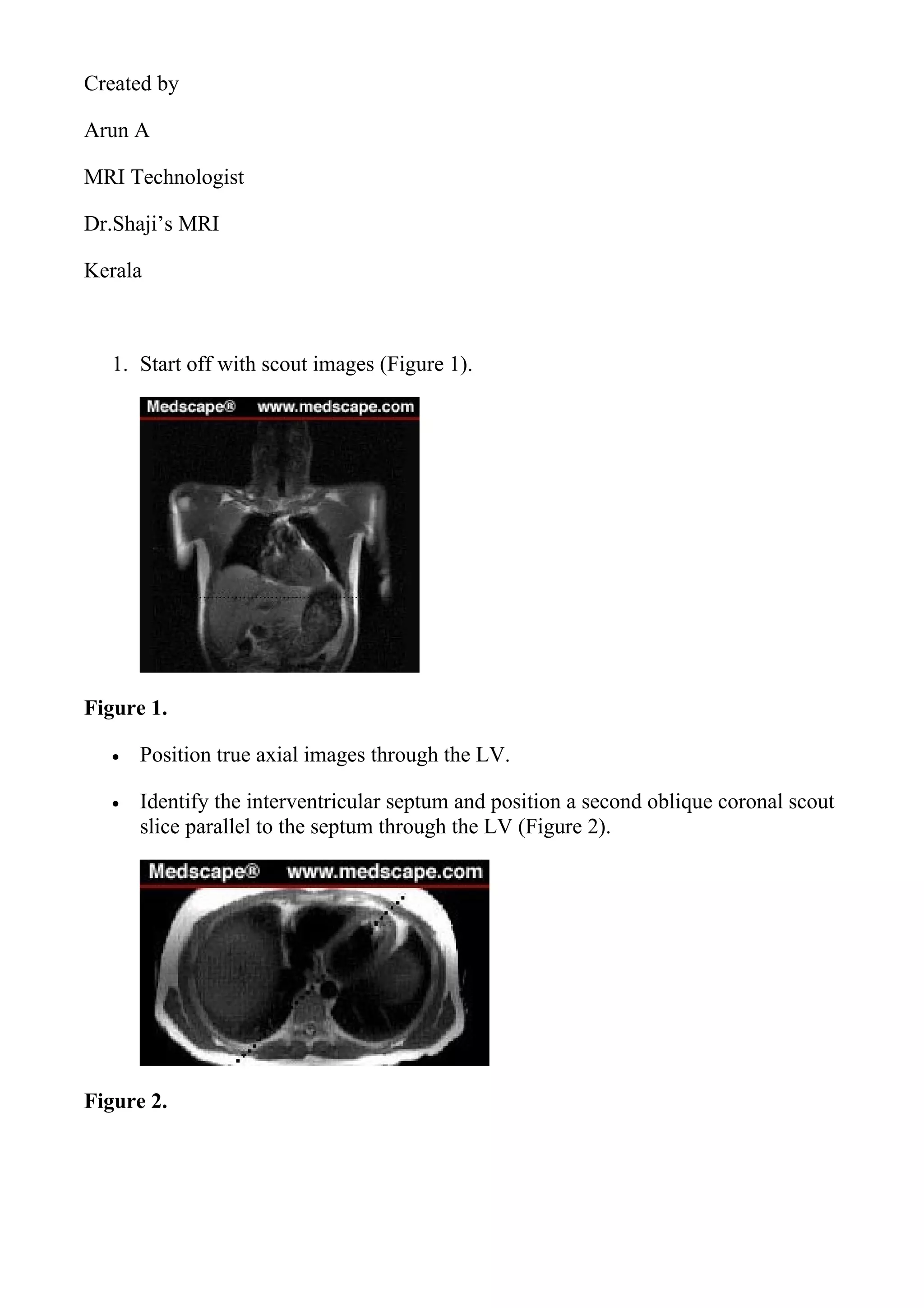
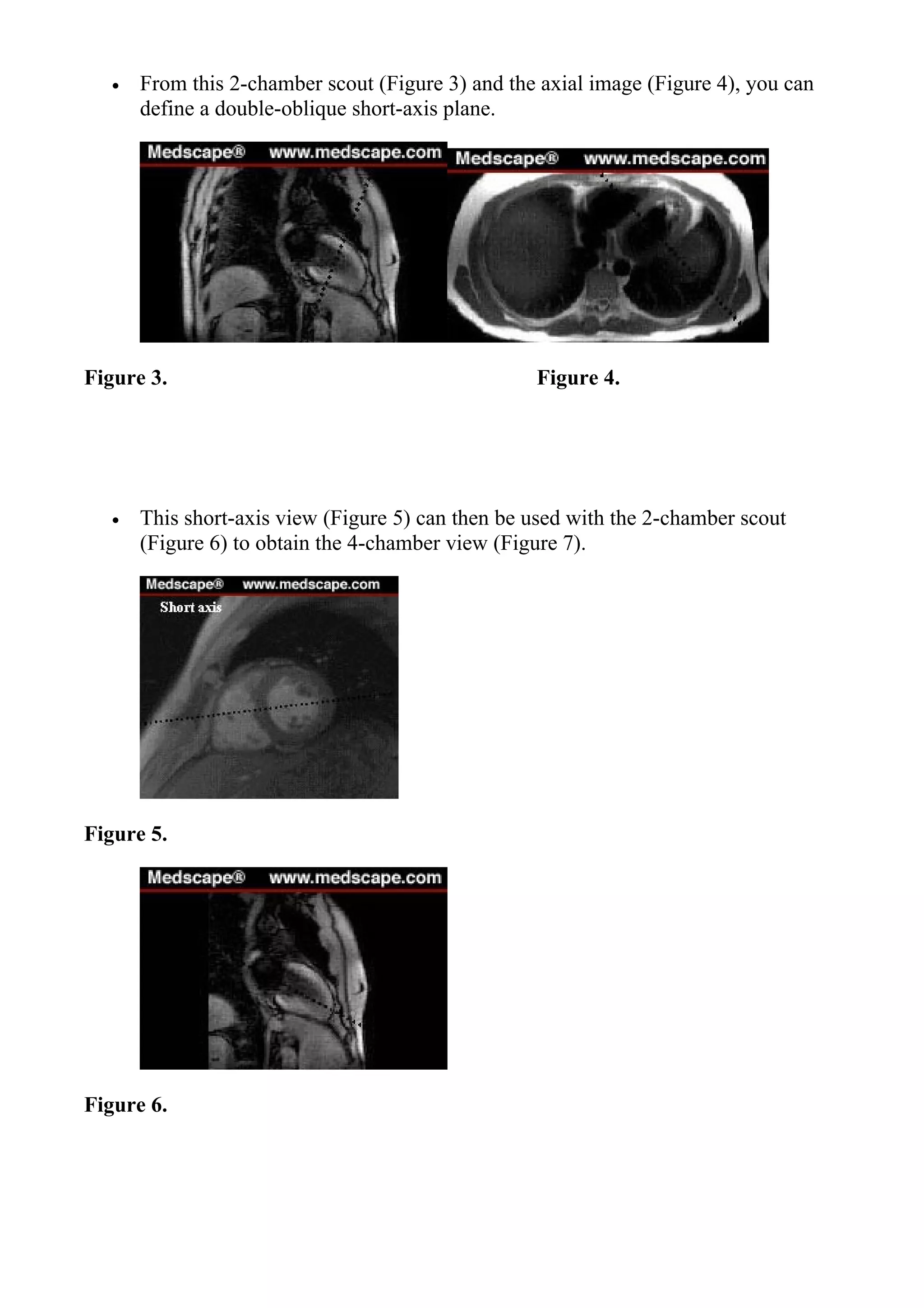

![Figure 10
Cardiac MRI: The Basic Sequences
Black Blood Imaging
• ECG-gated spin echo (SE) or fast-spin echo (FSE) (turbo spin echo [TSE])
• ECG-gated db-HASTE (double IR-half-Fourier single-shot turbo-spin echo)
-Uses: To identify extraluminal aortic pathology, intramural hematoma, or dissection
-Cardiac gating: TR = R-R interval for SE or FSE; gating not absolutely needed for HASTE
-Can be performed breath-hold (fast imaging) or multiple averages non-breath-hold (NBH)
-To get more slices, one may need to concatenate slices
-HASTE can be used in arrhythmias
Bright Blood Imaging
• Cine gradient echo imaging (GRE)
• FASTCARD
• True fast imaging with steady-state precession (FISP)
-Uses: To determine flow, motion, aortic valvular disease
-Cardiac gating: Choose temporal resolution based on TR and R-R interval
# temporal phases 0.85 x (R-R/TR)
-Can be performed breath-hold (segmented k-space) or 3-4 averages NBH
-Real-time true FISP can be used in arrhythmias
-Retrospectively gated sequences can be used with peripheral pulse gating if necessary
Velocity-Encoded CINE (Phase Contrast)
• Velocity encoded CINE imaging (Vinnie)
• FASTCARD PC
-Uses: To quantify flow at stenoses to estimate pressure gradient or collateral blood flow](https://image.slidesharecdn.com/startoffwithscoutimages-100608225627-phpapp01/75/Cardiac-MRI-4-2048.jpg)

