ENDOCARDITIS.pptx
- 1. ENDOCARDITIS Prepared by Nursing Instructor Mrs. Safoora Qureshi CON, PIMS
- 2. Endocardium • Inner/deepest layer of the heart • Consist of flattened epithelial cells • Lines the heart chambers and valves • Prevent friction • Promote smooth flow of the blood
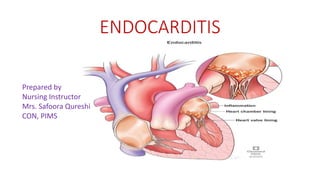
- 3. Endocarditis • Is the inflammation of endocardium, the inner most layer of the heart • Infective endocarditis (IE) is an infection of the inner surface of the heart, usually the valves • IE is a potentially fatal inflammation of heart valves’ lining and sometimes heart chambers’ lining. • IE is typically a bacterial infection and less commonly a fungal infection
- 4. Etiology Bacteria: • Staphylococcus aureus is the most virulent organism causing IE • Streptococcus viridian, • Enterocolli • Gram-positive and Gram- negative bacilli Fungus: • Candida albicans Viruses: • Coxsackie B virus
- 5. Risk Factors • Older age. • Artificial heart valves. • Germs are more likely to attach to an artificial (prosthetic) valves • Damaged heart valves. • such as rheumatic fever or infection • Congenital heart defects. • such as an irregular heart or abnormal heart valves • Implanted heart device. • such as a pacemaker, causing an infection of the heart's lining. • A history of endocarditis • Poor dental health • Long-term catheter use (indwelling caths or PD cath)
- 6. Classification Sub-Acute Endocarditis: Develops gradually over a period of weeks to several months • Most frequently seen in patients with • Damage heart. • Preexisting valvular disease Acute Infective Endocarditis: • Develops suddenly and may become life threatening with days • Primarily affect people with • Normal heart. • Healthy valves and • Present as a rapidly progressive illness
- 7. Pathophysiology Predisposing factors contribute to development of IE 1. A damage endocardial surface • Provide an environment conducive to bacterial growth such as valvular disease, RHD, CHD 2. Portal of entry: • Endocardial defects, a dental procedure or oral lesion may offered bacteria access to bloodstream Mechanism Vegetation: • Primary lesion of IE, consist of fibrin, leukocytes, platelets, and microbes that adhere to the valve surface or endocardium. Embolization • The loss of portions of these friable vegetations into the circulation results in embolization Systemic embolization: • left heart vegetation, progressing to various organ and to the extremities causing limb infarction • Right-side heart lesions embolize to the lungs Local infection: • cause damage to the valves or their supporting structure, result in dysrhythmias, valvular incompetency, HF
- 8. Damage to endothelial surface from anatomic or traumatic changes Primary focus of infection from causative agents Vegetation: consist of fibrin, leukocytes, microbes on valve surface & endocardium Local valve damage Management antibiotics not Bacteria, virus, fungus Right-side heart embolization Lung Infiltration of supportive structure Left-side heart embolization Brain liver spleen kidney limb Recovery Sepsis, HF, Heart block Pulmonary embolism Infective Endocarditis Pathophysiology
- 10. Clinical manifestation • Non- specific or Systemic illness: • Low grade fever, chill • Weakness, malaise, fatigue • Arthralgia, myalgia, back pain • Abdominal discomfort • Weight loss, • Headache • Feet legs swollen • Clubbing of fingers
- 11. Vascular Manifestation • Murmurs • Slinter hemorrhage ------ black longitudinal streaks in nail beds • Petechiae • Osler’s nodes------painful, tender, red or blue , pea-size nodes • Janeway's lesion --- pain less erythematous, flat, small red spots on palm and sole • Ruth’s spots -------- retinal hemorrhage reveals on fundoscopy Late Manifestations: secondary to IE • Splenomegaly • Flanks pain, abdominal rigidity, pulmonary edema • Hemiplegia, change in consciousness, gangrene
- 12. Osler’s nodes Janeway's lesion Slinter streaks Ruth’s spots
- 14. Diagnosis History and Physical Assessment: • Blood test • blood culture test: • Transthoracic Echocardiogram • Transesophageal echocardiogram/Ultrasound • Electrocardiogram / (ECG or EKG) • Chest X-ray • to find lug problems such as lung collapse and pulmonary edema
- 15. Treatment • Antibiotics • Infective Endocarditis will be treated with intravenous antibiotic therapy. Antibiotic therapy typically takes up to six weeks. • Steroids: as a immunosuppressant • To treat inflammation • To reduce autoimmune response and prevent permanent heart damage • NSAIDs: • To relieve pain
- 16. Collaborative Care Drug therapy Antibiotics • IV antibiotic therapy takes up to six weeks. Steroids: • To treat inflammation • To reduce autoimmune response • To prevent permanent heart damage NSAIDs: • To relieve pain Nursing Management • Strict bed rest • Restrict visitors • Keep in prop upped position • Monitor • vital signs, oxygen saturation • intake output • Meet nutritional requirement • Psychological support
- 17. Surgery • Indications • Prolonged infective endocarditis • damaged heart valves caused by endocarditis • Purpose; • To remove dead tissue, scar tissue, fluid buildup, or debris from infected tissue. • To repair or remove damaged heart valve • To replace it with either man-made material or animal tissue.
- 19. Prevention Healthy Life Style: • Be smoke-free. • Be more active. • Aim for a healthy weight. • Eat a healthy balanced diet – there are some specific diets you can follow that have been proven to reduce the risk of heart disease. • Drink less alcohol. • Manage stress