Heart Failure.pptx
- 1. Heart Failure Prepared by Nursing Instructor Mrs. Safoora Qureshi CON, PIMS
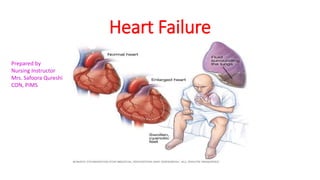
- 2. Heart Failure • Heart Failure is an state in which heart cannot provide sufficient cardiac output to satisfy metabolic need of the body • HF formerly called Congested Heart Failure • An abnormal clinical condition involving impaired cardiac pumping, results in characteristic pathologic changes of vasoconstriction and fluid retention • HF is not a disease, may associated with CAD, HTN, MI • HF is the heart’s inability to pump an adequate supply of blood to the body. • A clinical and pathophysiologic syndrome that results from ventricular dysfunction, volume, or pressure overload, alone or in combination
- 4. Reduce Cardiac Out put carotid baroreceptor stimulation Renal Perfusion/GFR Activation of CNS HR & Inotropy Myocardial toxicity Activation of RAAS Vasoconstriction After load Negative remodeling Worsens the LV Symptoms of HF shortness of breaths, arrythmias, edema, chest congestion etc increased angiotensin -II From increased Aldosterone water retention Hemodynamic alteration Preload Myocardial injury Pathophysiology of Heart Failure ANP & BNP Heart CHF
- 5. Pathology of Ventricular Failure • Systolic Failure (r-EF); The hallmark of systolic dysfunction is a decrease in the left ventricular ejection fraction. • The normal EF is greater than 55% of ventricular volume. • Systolic failure is caused by • impaired contractile function(MI) • increased afterload (hypertension), • mechanical abnormalities (VHD) • Diastolic Failure (p-EF): • is an impaired ability of the ventricles to relax and fill during diastole, result in decreased in stroke volume and CO. • High filling pressure due to stiff or noncompliance ventricles, result in venous engorgement in both pulmonary and systemic circulation.
- 6. Types Of HF: Left-sided Heart Failure: • is the most common type of heart failure. • Left-sided heart failure occurs when the left ventricle doesn’t pumps efficiently, result in reduce CO • This prevents the body from getting enough oxygen-rich blood. • The blood backs up into the lungs, which causes shortness of breath, pulmonary congestion and edema Right-Sided Heart Failure: • Heart failure can also affect the right side of the heart. Left-sided heart failure is the most common cause of this. • Other causes include certain lung problems and issues in other organs. z
- 7. Causes: Chronic • Coronary Artery Disease • Hypertension • Rhematic Heart Disease • Congenital Heart Disease • Cardiomyopathy, congenital or acquired • Valvular disease • Severe forms of anemia • Bacterial endocarditis Acute • Acute MI • Dysrhythmias • Pulmonary Embolism • Thyrotoxicosis • Hypertension Crisis • Rupture of Papillary muscles (Mitral Valve) • Ventricular Septal Defect • Myocarditis
- 8. Clinical manifestation of (CHF) • Chest Pain • Fatigue • Dyspnea / paroxysmal nocturnal dyspnea • Tachycardia • Edema / peripheral, hepatomegaly, ascites, and pulmonary • Nocturia • Skin changes /dusky, cool, damp, hair loss • Behavioral Changes/ restlessness, confusion, impaired attention and memory • Weight Changes
- 9. CHD/CCF
- 10. Complication: • Pleural effusion • Dysrhythmias • Left ventricular thrombus • Hepatomegaly • Renal failure
- 11. Diagnosis: • History • Physical Examination • X-rays • ECG • Lab: Cardiac Enzyme BNP • Serum chemistries such as; • LFT, RFT, TFT, CBC • Echocardiogram • Stress testing • Cardiac Catheterization
- 12. Collaborative Care • Treatment of underline cause • Oxygen therapy 2 --- 6 l/min by nasal catheter • Rest-activity period • Drug therapy • Daily weight • Sodium restricted diet • Circulatory/ventricular assist device • (IABP) • Cardiac resynchronization therapy with • cardioverter-defibrillator • Cardiac transplant
- 13. ICD IABP
- 14. Drug therapy in (CHF) • Diuretics • Morphine sulphate • Vasodilators: • ACE inhibitors • Nitroglycerin • BNP (synthetic) • Beta-Blockers • Positive inotropes; • Digoxin • Dopamine, Dobutamine • Angiotensin II inhibitor • Antidysrhythmic
- 15. Nursing Management Oxygen therapy: • Administers oxygen as per need by nasal catheter • Monitor the effectiveness of the therapy to identify hypoxia and establish a range of oxygen saturation Position: • Semi-Fowler position to alleviate dyspnea and pain Respiratory Monitoring: • RR, rhythm, depth, and resp.efforts, to evaluate respiratory status • Auscultate breath sounds to assess congestion • Monitor dyspnea to observe the improvement of respiratory status • Note the events that improve or worsen the distress to detect the events, influence ADLs
- 16. Monitor Cardiac status: • Continue cardiac monitoring to detect arrythmias Anxiety reduction: • Use a reassuring approach to gain client confidence in care provider • Promote a sense of security by explaining all therapeutic procedures • Identify source of anxiety/fear and plan anxiety relieving techniques • Create a atmosphere to facilitate trust • Instruct the client in use of relaxation techniques (imagery) • Promote sleep by providing a calm and quiet environment
- 17. Energy Management: • Encourage alternate rest and activity period to reduce cardiac workload • Provide calming diversionary activities to promote relaxation to reduce oxygen consumption • Monitor patient’s oxygen demand during self-care/nursing care activities to determine the level of activity that can be performed Fluid /Electrolyte management: • Daily weight to monitor fluid retention/diuresis and weight reduction • CVP line monitoring • Monitor serum electrolyte balance to assess response to treatment
- 18. Hypervolemia management; • Monitor • respiratory status/distress/SOB to detect pulmonary edema • hemodynamic status including CVP, MAP to evaluate effective ness of therapy • renal function and intake output to monitor fluid balance • effectiveness of diuretics to assess response to treatment Dietary Management: • (DASH ) diet is widely used for patients with HF • Fluid restriction incase of renal insufficiency • Sodium restricted diet