This document discusses tonsillitis, tonsillectomy, and adenoidectomy. It provides details on:
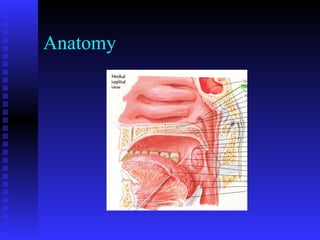
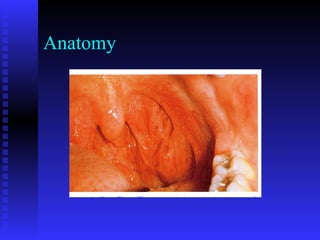
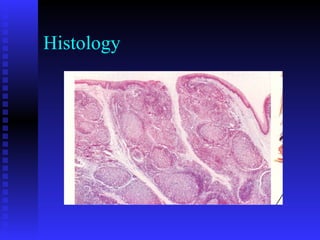
- The history and anatomy of these procedures
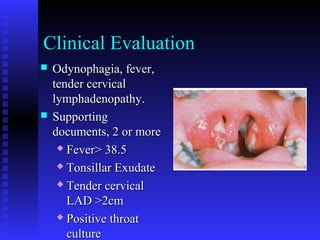
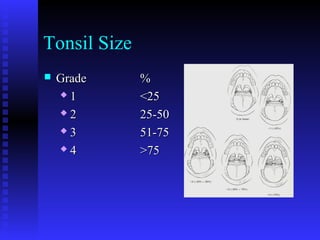
- Clinical evaluation and differential diagnosis of tonsillitis
- Surgical indications and techniques for tonsillectomy and adenoidectomy
- Preoperative evaluation and management of bleeding disorders
- Adjuvant therapies like antibiotics, steroids, and local anesthetics to improve postoperative outcomes