This document provides an overview of the temporomandibular joint (TMJ), including its:
- Types (synovial, bicondylar, ginglymoarthroidal)
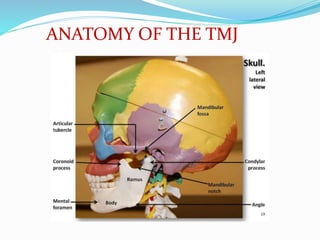
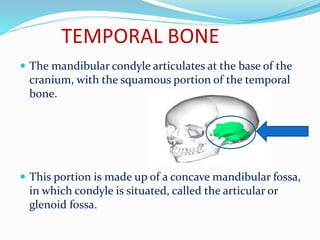
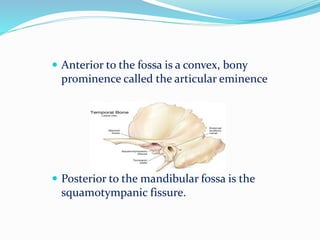
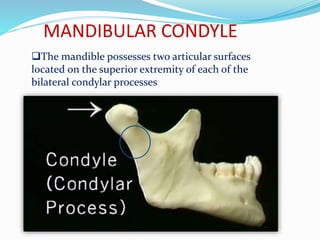
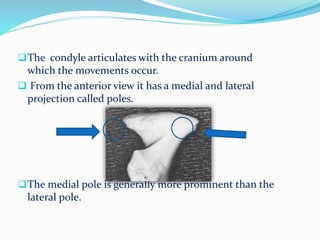
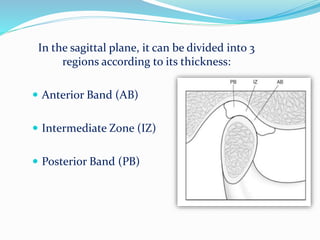
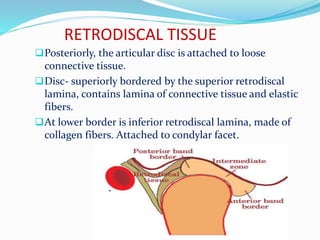
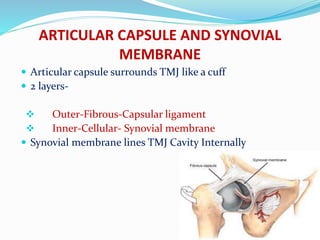
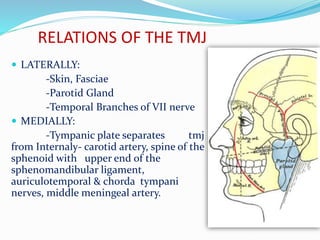
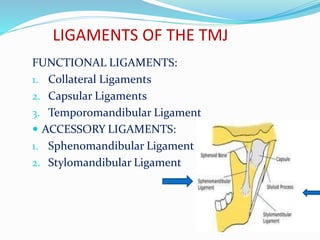
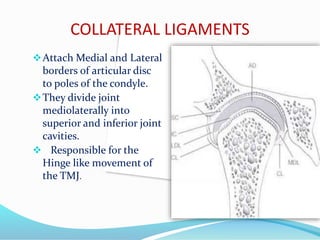
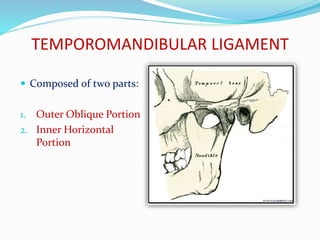
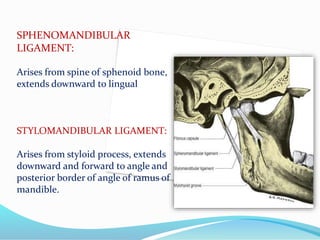
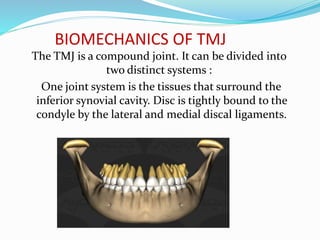
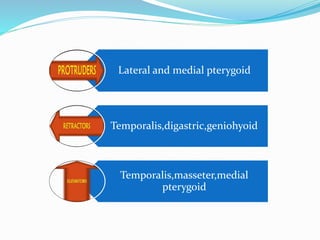
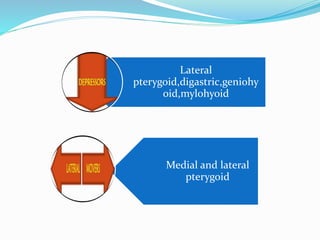
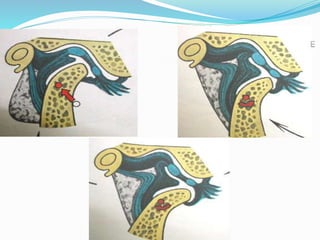
- Anatomy (bones, articular disc, ligaments, muscles)
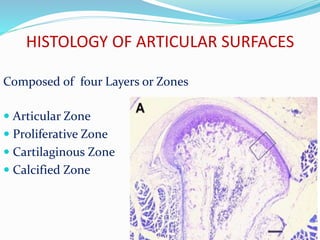
- Histology of the articular surfaces
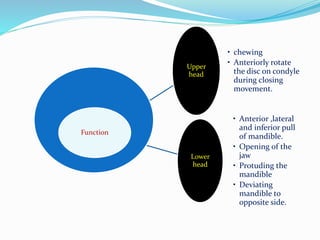
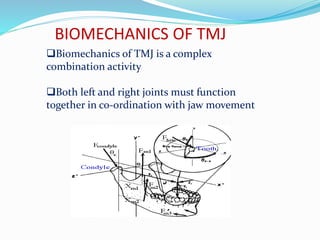
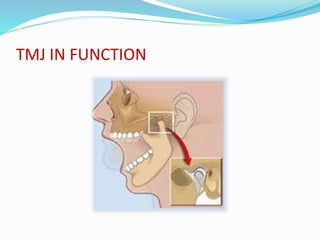
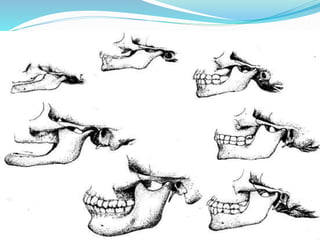
- Biomechanics and functions like opening and closing the mouth
- Age-related changes like flattening of bones and thinning of tissues