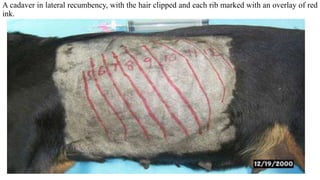
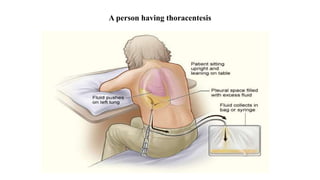
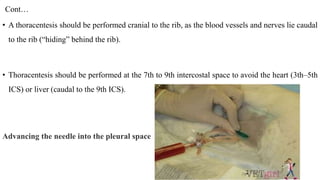
Thoracentesis is a procedure to remove fluid or air from the pleural space for diagnostic or therapeutic purposes. It requires inserting a needle between the ribs to drain fluid. The document outlines the materials, steps, and potential complications of performing thoracentesis on dogs, cats, and horses. Diagnostic thoracentesis is indicated for animals showing respiratory distress and reduced breath sounds to identify the cause of pleural effusion. Analysis of drained pleural fluid can help determine the underlying disease process.