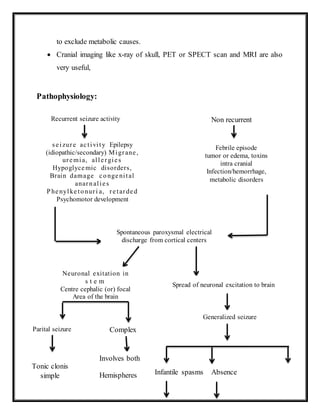
This document discusses neurological disorders, specifically focusing on convulsions disorders/seizure disorders/epilepsy. It defines epilepsy as recurrent episodes of cerebral origin involving disturbances of movement, sensation, behavior and consciousness. Various causes of epilepsy are described, including perinatal conditions, infections, metabolic conditions, poisoning, and genetic/hereditary syndromes. The document then classifies epilepsy and outlines the clinical features, diagnostic evaluation, and management including drug therapy, diet therapy, and surgery. Meningitis is also discussed, describing the causes, risk factors, pathophysiology, types (bacterial, viral, tuberculosis), clinical features, diagnostic evaluation, and treatment of various forms of meningitis.

![Systemic Disorders:
Vasculitis (CNS or systemic)
SLE
Hypertensive encephalopathy
Renal failure
Hepatic encephalopathy
Other:
Trauma
Tumor
Febrile
Idiopathic
Familial
Classification of Epilepsy:
Clinically epilepsy can be broadly classified in two groups i.e. generalized or
partial
1.Generalized Seizures:
2. Tonic — &No seizures (Grand ma])
3. Absence seizures:- i) Typical (petit ma]) ii) Atypical
4. Atopic seizures (Dropattacks) Myoclonic seizures
2. Partial Seizures:
a) Simple partial seizures: (with elementary symptoms and or impaired
consciousness)
I. With motor signs (Jacksonians or Focal motor).
II. With somato-sensory or special sensory i.c visual or auditory](https://image.slidesharecdn.com/neurologicaldisorders-160922072638/85/Neurological-disorders-2-320.jpg)
![III. With autonomic manifestations (Abdominal epilepsy)
b) Complex partial seizures: manifested with impaired consciousness and with
Automatism it include psychomotor or temporal lobe seizures.
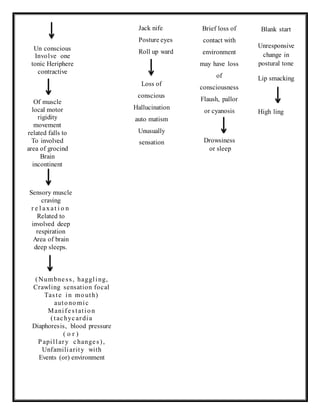
Clinical Features:
Generalized tonic-clonic seizures (grand ma! type)
The classical form has five phases, i.e an aura, tonic spasm, cionio phase and
postectal phase.
Aura-dizziness tonic spasm phase-body becomes stiff, face, may become
pale and distorted, eyes fixed in one position, back may be arched.
Head turned to backward in one side,
Arms are equally flexed and hands are clenched.
Due to spasm of respiratory muscles, there is ineffective breathing and cyanosis.
The clonic phase- the child may pass stool and urine involuntarily in the
postectal patient become confused or exhassted or perform automatic actions
Headache
3. Absence Seizures (Petitmal):
The child may loss contact with the environment for a few seconds.
Day dreaming
The child may discontinues the activity suddenly (e.g. reading, writing)and
may resume the same activity when the seizures occur.
A typical absence seizure may present as redding of the eyes, nodding of the
head, slight hand movements and smacking of lips.
4. Status Epilepticus:
Cerebral damage may occur due to prolonged cerebra] hypoxia or](https://image.slidesharecdn.com/neurologicaldisorders-160922072638/85/Neurological-disorders-3-320.jpg)
![hypoglycemia
In postectal state the child may have cardio respiratory arrest or aspiration
of vomitus.
5. Partial Seizures:
Motor, sensory, psych], or autonomic abnormalities, but consciousness
is preserved
6. Myoclonic Seizures (Infantile spasms):
Cerebral abnormalities
Mental retardation
The child presents with sudden forceful myoclonic contractions
involving the muscles of trunk, neck and extremities
7. Neonatal Seizures:
Eye blinking
Flutering and buccolingual movements
Diagnostic Evaluation:
Careful history taking
Physical and neurological examination
Laboratory tests.
EEG:- It may confirm type of abnormality and may detect facility, extent of
affection
C.T scan of head
Blood studies:-Blood glucose, calcium and lead and amino acid in serum,](https://image.slidesharecdn.com/neurologicaldisorders-160922072638/85/Neurological-disorders-4-320.jpg)