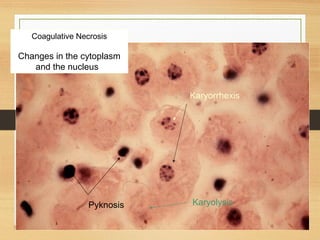
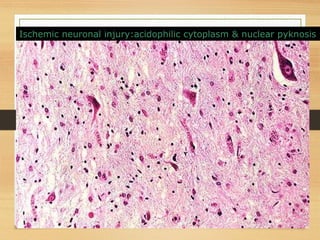
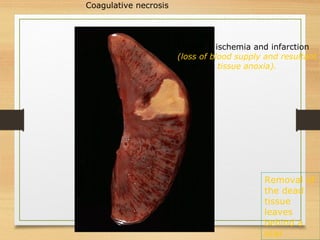
The document discusses necrosis and apoptosis, defining both processes and outlining their differences. It details the six types of necrosis, including coagulative, liquefactive, caseous, fat, gangrenous, and fibrinoid, with examples and characteristics of each. The document also describes morphological changes associated with necrosis and the implications of cell death on tissues and organs.