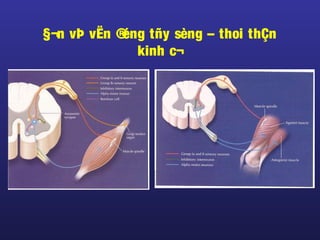
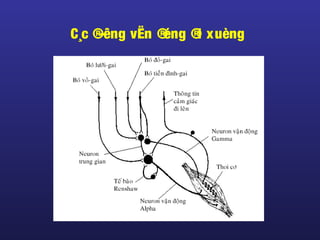
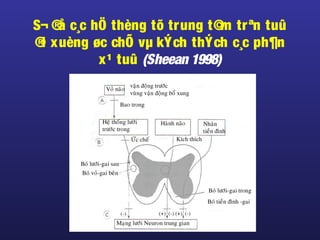
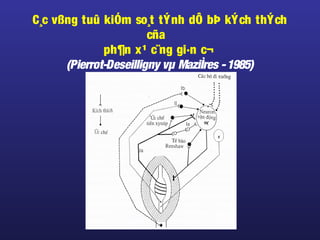
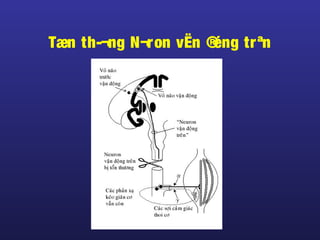
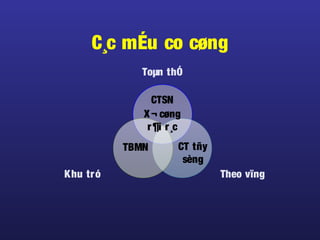
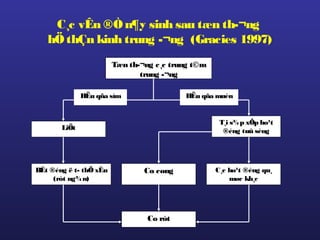
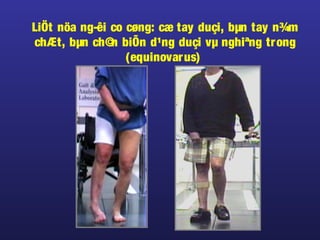
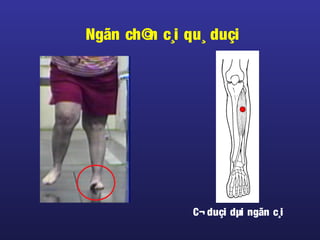
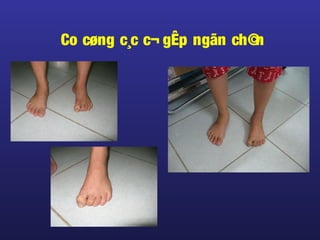
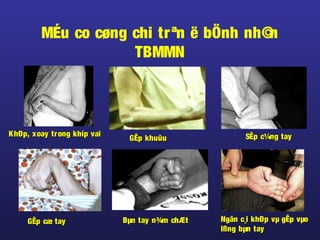
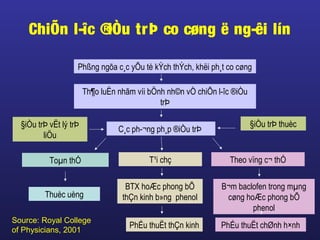
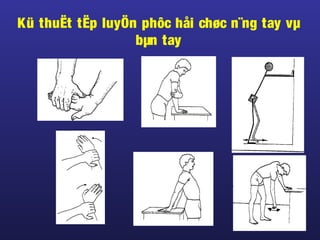
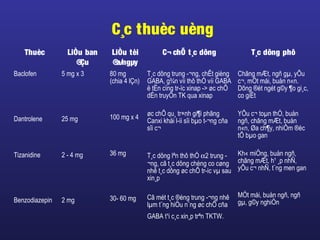
Tài liệu này trình bày về điều trị co cứng, định nghĩa và các phương pháp điều trị tổng quan. Nó liệt kê các triệu chứng, nguyên nhân và các cách tiếp cận để giảm thiểu tình trạng co cứng thông qua liệu pháp và thuốc. Cuối cùng, bài viết cũng thảo luận về những yếu tố ảnh hưởng đến chức năng vận động và cách quản lý co cứng trong điều trị.