This document outlines a presentation on the genus Clostridium. It begins with an introduction to Clostridium, noting that they are gram-positive, obligate anaerobic rods that can form endospores. It then covers the taxonomy and classification of Clostridium. The document discusses several important pathogenic Clostridium species - C. botulinum, C. perfringens, C. tetani, C. difficile. For each species, it covers transmission, clinical presentation, treatment and prevention. The final section discusses various diagnostic methods for Clostridium such as culture methods, gram staining, and molecular detection techniques.







![06.12.2013
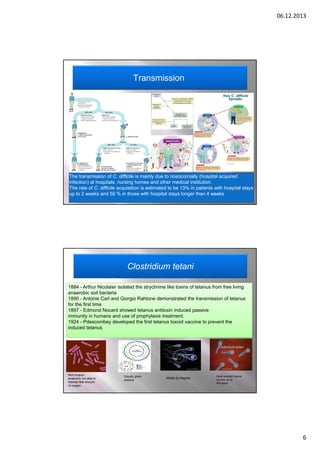
C. tetani infection/intoxication
Spores of
C. tetani
in wound
Germination and toxin
production under
anaerobic conditions
Transport of toxins via
lymphatic- bloodstream
through motor neurons
to spinal cord
Wound
contaminated
with soil
Symptoms
[Madigan et al. 2009]
17
Mechanism of action
Inhibitory interneurons
Excitation signals
from the
central nervous
system
Release of acetylcholine
inhibited by glycine
Muscle relaxation
Tetanus
toxin
Uncontrolled release
of acetylcholine
Spastic paralysis
18
Modified according to [Madigan et al. 2009]
9](https://image.slidesharecdn.com/clostridiamoleculardiagnosticsfinal-140221140026-phpapp02/85/Clostridia-9-320.jpg)
![06.12.2013
Mechanism of action
Inhibitory neurotransmitter glycine usually stops the
release of acetylcholine from the motor neurons
muscle relaxation
AB toxin (= Tetanospasmin, 50 kDa light chain + 100 kDa
heavy chain) inhibits release of glycine from inhibitory
interneurons
No glycine constant release of acetylcholine
spastic paralysis / uncontrolled contraction of the muscle
[Madigan et al. 2009]
19
Treatment:
Immediate treatment with human tetanus immune
globulin (TIG)
Medication to control muscle spasm
Aggressive wound care
Antibiotics: Metronidazole, Clindamycin, Erythromycin, Penicilin
Prevention:
Being fully immunized is the best tool to prevent tetanus
Immediate and proper wound care can also help
prevent infection
10](https://image.slidesharecdn.com/clostridiamoleculardiagnosticsfinal-140221140026-phpapp02/85/Clostridia-10-320.jpg)


![06.12.2013
Clostridium botulinum
Transmission:
Botulism is caused by exposure to botulinum toxin,
humans can become infected in a number of ways:
Inhalation of toxin
Consumption of toxin (foodborne)
Consumption of C. botulinum spores
(infant; adult intestinal toxemia)
Contamination of a tissue with C. botulinum
spores (wound)
Incubation Period:
12-80 hours (range 2 hours to 8 days)
Botulism
Foodborne botulism
C. botulinum in food
Toxin produced
Toxin ingested
Toxin in bloodstream
Attacks neurons
(flaccid paralysis)
Infant botulism
C. botulinum spores
ingested
Wound botulism
C. botulinum spores
in wound
C. botulinum grows
in intestinal tract
C. botulinum grows
in wound
Toxin produced
Toxin produced
Modified according to [Salyers et al. 1994]
13](https://image.slidesharecdn.com/clostridiamoleculardiagnosticsfinal-140221140026-phpapp02/85/Clostridia-13-320.jpg)
![06.12.2013
Botulinum toxin
7 related AB toxins (A‐G) most potent biological toxins known [Madigan et al. 2009]
Relevant toxins for human diseases: A, B, E [Lindstöm et al. 2006]
Light chain
(50 kD)
A
Heavy chain
(100 kD)
B
AB toxin (150 kD)
[Zhang et al. 2012]
Mechanism of C. botulinum intoxication
Absorption of toxin by mucosal surfaces in the
gastrointestinal system, the eye or non intact skin.
Botulinum toxin blocks acetylcholine release at the
neuromuscular junction of skeletal muscle neurons
and peripheral muscarinic cholinergic autonomic
synapses
It binds irreversibly to presynaptic receptors to
inhibit the release of acetylcholine and cause
neuromuscular weakness and autonomic
dysfunction
14](https://image.slidesharecdn.com/clostridiamoleculardiagnosticsfinal-140221140026-phpapp02/85/Clostridia-14-320.jpg)


![06.12.2013
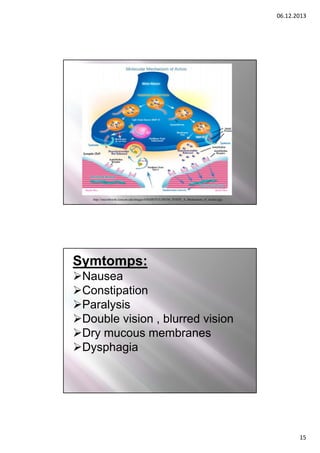
Mechanism of infections
Mechanism of action
Toxin A: Enterotoxin that disturbs the transport of
electrolytes loss of fluid, diarrhea
Toxin B: Cytotoxin that damages cells of the colon
36
[Jones et al. 2012]
18](https://image.slidesharecdn.com/clostridiamoleculardiagnosticsfinal-140221140026-phpapp02/85/Clostridia-18-320.jpg)












![06.12.2013
References
• Clinical Microbiology Reviews – Laboratory
Diagnostics of Botulism [Lindström,Korkeala]
• Manual of Clinical Microbiology
[Patrick R. Murray, Ellen Jo Barron et al.]
• Medizinische Mikrobiologie
[Herbert Hof, Rüdiger Dörries]
• Dario et al, Multiplex PCR for Detection of
Botulinum Neurotoxin – Producing Clostridia in
clinical, food, and environment samples;
(20):6457-6461; Appl. Environmental
Microbiology, 2009
References
•
•
•
•
•
•
Lindström M, Korkeala H: Laboratory Diagnostics of Botulism.
Clin. Microbiol. Rev. 2006, 19(2):298
Madigan MT, Martinko JM, Dunlap P V, Clark DP: Biology of
Microorganisms. 12th edition, Pearson Education Inc.,
San Francisco 2009
Salyers AA, Whitt DD: Bacterial Pathogenesis: A molecular
approach. ASM Press, Washington, D.C. 1994
Zhang Y, Lou J, Jenko KL, Marks JD, Varnum SM:
Simultaneous and sensitive detection of six serotypes of botulinum
neurotoxin using enzyme‐linked immunosorbent assay‐based
protein antibody microarrays. Analytical Biochemistry 430 (2012) 185–192
“Development of real‐time PCR tests for detecting
botulinum neurotoxins A,B,E,F producing Clostridium botulinum,
[…].” [P.Fach et al.], Journal of AppliedMicrobiology
Taq‐Man‐Picture [http://en.wikipedia.org/wiki/File:Taqman.png]
34](https://image.slidesharecdn.com/clostridiamoleculardiagnosticsfinal-140221140026-phpapp02/85/Clostridia-34-320.jpg)
