2021 WHO Classification of brain tumours.pptx
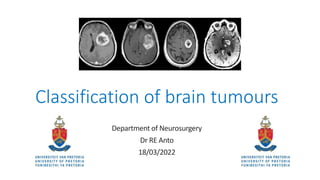
- 1. Classification of brain tumours Department of Neurosurgery Dr RE Anto 18/03/2022
- 2. Contents • Introduction • Epidemiology • Risk factors • Etiology • Hereditary sx • Clinical presentation • Classification systems • Benign vs Malignant • Tumour locations • WHO Classification System • Main changes • References
- 3. Introduction • Brain tumour is an abnormal mass of tissue intracranially, in which cells grow and multiply uncontrollably, seemingly unchecked by the mechanisms that control normal cells. • Multiple classification systems • Primary vs. Secondary • Type of cell origin • Location • Grading (Benign or Malignant)
- 4. Epidemiology • Primary brain tumours are relatively rare: 2% of all cancers in adults • NOTE: In paeds: 15-20 % of paediatric cancers • Great variance in degree of incidence between 1st world and developing countries • May be due to differences in resources like imaging modalities and better registration and data capture systems • Incidence rises with age • Males: Female (1.5:1) – except meningiomas (female > male)
- 5. Davis FG, McCarthy BJ. Current epidemiological trends and surveillance issues in brain tumours. Expert Rev Anticancer Ther2001;1:395–401.
- 6. Risk factors • Develop as a consequence of accumulated genetic alterations that permit cells to evade normal regulatory mechanisms and destruction by the immune system • Seizures may herald development of cerebral tumours by years! • Risk for any cerebral tumour after first admission for epilepsy is increased 20-fold • Highlights the need for continued surveillance of patients with new- onset seizures
- 7. Etiology • Some epidemiological studies suggest increased incidence of astrocytomas • Petrochemicals eg vinyl chloride • Electromagnetic radiation • High dose ionizing radiation • 10 times risk of meningiomas • 2.5 times risk for gliomas • Primary CNS lymphoma • Viruses eg EBV • Immunocompromised (transplant patient, AIDS)
- 8. Hereditary syndromes • < 5% of all primary CNS tumours • Neurofibromatosis I and II (MPNST, Optic n glioma, Meningiomas, Vestibular schwannoma) • Von-Hippel Lindau sx (Haemangioblastoma) • Tuberous sclerosis (SEGA, Cortical tubers) • Li-Fraumeni sx (Malignant gliomas, PNET, Medulloblastoma) • MEN I (Multiple endocrine neoplasia) ( Pituitary adenomas, Malignant schwannoma) • Turcot sx (GBM, Medulloblastoma) • Werner’s sx (Meningioma)
- 9. Clinical Presentation • Generalized or focal signs. • Epilepsy: focal or generalized tonic clonic seizures • Frontal lobe: • Anosmia • Dementia • Urinary incontinence • Conjugate deviation of eyes • Aphasia
- 10. Clinical Presentation • Temporal lobe: • Temporal lobe epilepsy • Auditory hallucinations • Memory difficulties • Parietal lobe: • Hemisensory changes • Sensory apraxia • Occipital lobe: • Visual field changes • Chiasmatic lesions: • Visual field changes
- 11. Clinical Presentation • Posterior fossa lesions: • CN Palsies • Long tract signs • Obstructive HCP • Sellar lesions • Hormone dysfunction • Acromegaly • Hyperprolactinemia • Hypopituitarism • Hypocortisolemia • Visual disturbances
- 12. Classification systems • Primary: • Arise from the brain tissue or surrounding meninges itself • Glial • Non-glial (in structures in the brain including nerves, vessels, glands) • Secondary: • Arises from other tumours in the body and migrate to the brain • 5-10 times more common than primary CNS tumours (most common tumours in adults)
- 15. Benign vs Malignant • This distinction is less significant than for other systems • Benign • Slow-growing tumours • Low cellularity • Few mitosis • No necrosis • No vascular proliferation • However, location of these tumours can have lethal consequences despite its histological classification • Eg: FM meningioma causing compression of the medulla and causing cardiorespiratoy arrest
- 16. Malignant • Not malignant “metastasize” out of CNS (rare) • Morphological Features: • 1. Nuclear atypia • 2. Mitosis • 3. Endothelial Proliferation • 4. Necrosis Daumas-Duport C, Scheithauer B, O'Fallon J, Kelly P (1988). Grading of astrocytomas. A simple and reproducible method. Cancer 62: 2152-2165.
- 18. WHO Classification • 1979: 1st edition – Histological typing of CNS tumours • 1993: 2nd edition – Reflected advances in immunohistochemistry • 2000: 3rd edition – Started introduction pathology and genetics • 2007: 4th edition – used up until 2015 (Youmans 6th edition) • 2016: Revised 4th edition – substantial revision of 4th edition
- 20. WHO Classifications (2007/2016) • Formulating concept of how CNS tumours diagnoses are structured in the molecular era • Restructured diffuse gliomas, medulloblastomas and incorporated genetically identified entities. • Embryonal tumours (removal of PNET) • Ependymoma genetic variants introduced
- 21. WHO Classifications (2007/2016) • Addition of newly recognized entities, variants and patterns: • IDH-wildtype and IDH-mutant glioblastoma (entities) • Diffuse midline glioma, H3 K27M–mutant (entity) • Embryonal tumour with multilayered rosettes, C19MC-altered (entity) • Ependymoma, RELA fusion–positive (entity) • Diffuse leptomeningeal glioneuronal tumor (entity) • Anaplastic PXA (entity) • Epithelioid glioblastoma (variant) • Glioblastoma with primitive neuronal component (pattern) • Multinodular and vacuolated pattern of ganglion cell tumor (pattern)
- 22. WHO Classifications (2007/2016) • Deletion of former entities, variants and terms: • Gliomatosis cerebri • Protoplasmic and fibrillary astrocytoma variants • Cellular ependymoma variant • “Primitive neuroectodermal tumor” • Addition of brain invasion as a criteria for atypical meningioma • Restructuring of solitary fibrous tumour and hemangiopericytoma (SFT/HPC) as one entity and adapting a grading system to accommodate this change • Expansion and clarification of entities included in nerve sheath tumors, with addition of hybrid nerve sheath tumors and separation of melanotic schwannoma from other schwannomas • Expansion of entities included in hematopoietic/lymphoid tumors of the CNS (lymphomas and histiocytic tumors
- 24. 2021 WHO Classification • 5th edition of WHO Classification of Tumours of the Central Nervous System (CNS) • Sixth version of the international standard for the classification of brain and spinal cord tumours • Build on the 2016 updated fourth edition and the work of the Consortium to Inform Molecular and Practical Approaches to CNS Tumour Taxonomy (cIMPACT-NOW)
- 25. cIMPACT-NOW • Consortium to Inform Molecular and Practical Approaches to CNS Tumour Taxonomy – Not Officially WHO • Seven updates from 2016-2020
- 26. Gliomas, glioneuronal tumors, and neuronal tumours • Adult-type diffuse gliomas • Astrocytoma, IDH-mutant • Oligodendroglioma, IDH-mutant, and 1p/19q-codeleted • Glioblastoma, IDH-wildtype • Pediatric-type diffuse low-grade gliomas • Diffuse astrocytoma, MYB- or MYBL1-altered • Angiocentric glioma • Polymorphous low-grade neuroepithelial tumor of the young • Diffuse low-grade glioma, MAPK pathway-altered • Pediatric-type diffuse high-grade gliomas • Diffuse midline glioma, H3 K27-altered • Diffuse hemispheric glioma, H3 G34-mutant • Diffuse pediatric-type high-grade glioma, H3-wildtype and IDH-wildtype • Infant-type hemispheric glioma
- 27. Gliomas, glioneuronal tumors, and neuronal tumours • Circumscribed astrocytic gliomas • Pilocytic astrocytoma • High-grade astrocytoma with piloid features • Pleomorphic xanthoastrocytoma • Subependymal giant cell astrocytoma • Chordoid glioma • Astroblastoma, MN1-altered
- 28. Glioneuronal and neuronal tumours • Ganglioglioma • Desmoplastic infantile ganglioglioma (DIG) / desmoplastic infantile astrocytoma • Dysembryoplastic neuroepithelial tumor • Diffuse glioneuronal tumor with oligodendroglioma-like features and nuclear clusters (provisional inclusion) • Papillary glioneuronal tumor • Rosette-forming glioneuronal tumor • Myxoid glioneuronal tumor • Diffuse leptomeningeal glioneuronal tumor • Gangliocytoma • Multinodular and vacuolating neuronal tumor • Dysplastic cerebellar gangliocytoma (lhermitte-duclos disease) • Central neurocytoma • Extraventricular neurocytoma • Cerebellar liponeurocytoma
- 29. Ependymal tumours • Supratentorial ependymoma • Supratentorial ependymoma, ZFTA fusion-positive • Supratentorial ependymoma, YAP1 fusion-positive • Posterior fossa ependymoma • Posterior fossa ependymoma, Group PFA • Posterior fossa ependymoma, Group PFB • Spinal ependymoma • Spinal ependymoma, MYCN-amplified • Myxopapillary ependymoma • Subependymoma
- 30. Choroid Plexus tumours • Choroid plexus papilloma • Atypical choroid plexus papilloma • Choroid plexus carcinoma
- 31. Embryonal tumours - Medulloblastoma • Medulloblastomas, molecularly defined • Medulloblastoma, WNT-activated • Medulloblastoma, SHH-activated and TP53-wildtype • Medulloblastoma, SHH-activated and TP53-mutant • Medulloblastoma, NON-WNT/NON-SHH • Medulloblastomas, histologically defined
- 32. Other CNS Embryonal tumours • Atypical teratoid/rhabdoid tumor • Cribriform neuroepithelial tumor (provisional inclusion) • Embryonal tumor with multilayered rosettes (ETMR) • CNS neuroblastoma, FOXR2-activated • CNS tumor with BCOR internal tandem duplication • CNS embryonal tumor
- 33. Pineal tumours • Pineocytoma • Pineal parenchymal tumor of intermediate differentiation • Pineoblastoma • Papillary tumor of the pineal region • Desmoplastic myxoid tumor of the pineal region, smarcb1- mutant
- 34. Cranial and Paraspinal nerve tumours • Schwannoma • Neurofibroma • Perineurioma • Hybrid nerve sheath tumor • Malignant melanotic nerve sheath tumor • Malignant peripheral nerve sheath tumor • Paraganglioma
- 35. Meningioma • Meningothelial • Fibrous • Transitional • Psammomatous • Angiomatous • Microcystic • Secretory • Lymphoplasmacyte-rich • Metaplastic • Chordoid • Clear Cell • Atypical • Papillary • Rhabdoid • Anaplastic
- 36. Mesenchymal, non-meningothelial tumours – Soft tissue tumours • Fibroblastic and myofibroblastic tumors • Solitary fibrous tumor • Vascular tumors • Hemangiomas and vascular malformations • Hemangioblastoma • Skeletal muscle tumors • Rhabdomyosarcoma • Uncertain differentiation • Intracranial mesenchymal tumor, FET-CREB fusion-positive (provisional inclusion) • CIC-rearranged sarcoma • Primary intracranial sarcoma, dicer1-mutant • Ewing sarcoma
- 37. Chondro-osseous tumours • Chondrogenic tumors • Mesenchymal chondrosarcoma • Chondrosarcoma • Notochordal tumors • Chordoma (including poorly differentiated chordoma)
- 38. Melanocytic tumours • Diffuse meningeal melanocytic neoplasms • Meningeal melanocytosis • Meningeal melanomatosis • Circumscribed meningeal melanocytic neoplasms • Meningeal melanocytoma • Meningeal melanoma
- 39. Hematolymphoid tumours - Lymphomas • CNS lymphomas • Primary diffuse large b-cell lymphoma of the CNS • Immunodeficiency-associated CNS lymphoma • Lymphomatoid granulomatosis • Intravascular large b-cell lymphoma • Miscellaneous rare lymphomas in the CNS • MALT lymphoma of the dura • Other low-grade b-cell lymphomas of the CNS • Anaplastic large cell lymphoma (ALK+/ALK−) • T-cell and NK/t-cell lymphomas
- 40. Germ cell tumors • Mature teratoma • Immature teratoma • Teratoma with somatic-type malignancy • Germinoma • Embryonal carcinoma • Yolk sac tumor • Choriocarcinoma • Mixed germ cell tumor
- 41. Tumors of the sellar region • Adamantinomatous craniopharyngioma • Papillary craniopharyngioma • Pituicytoma, granular cell tumor of the sellar region, and spindle cell oncocytoma • Pituitary adenoma (pitNET) • Pituitary blastoma
- 42. Metastases to the CNS • Metastases to the brain and spinal cord parenchyma • Metastases to the meninges
- 43. Main changes in 5th edition • Builds on prior version by placing greater emphasis on molecular markers in terms of classification and grading • Heterogenous classification • Layered report structure • Integrated diagnosis • Histopathological classification • CNS WHO Grade • Molecular information
- 44. Grading • Within tumour types • Unlike other WHO classification systems that graded each tumor based on its own features (i.e. the most low-grade version of a particular tumor was given grade 1) • This approach has been abandoned, in favour of grading tumours within “type” • Example: • No Grade 1 Diffuse Astrocytoma, IDH Mutant (only 2,3 or 4) • Glioblastoma, IDH-wildtype – can only be Grade 4 • Arabic numerals • Previously – I,II,III,IV (Roman numerals) • Replaced by Arabic Numerals – 1,2,3,4 • Example: Meningioma, CNS WHO Grade 1
- 45. Grading • Anaplastic modifier • The term anaplastic, used extensively in the prior classifications has been dropped in favour of grading only. • Thus what was previously known as an "anaplastic astrocytoma" is now referred to as an "astrocytoma, IDH-mutant, CNS WHO grade 3 • Molecular grading • For the first time, molecular features have been explicitly added to the grading schema • May supersede histological features. • Example: an IDH-wildtype astrocytoma with low-grade histologic features can be considered Grade 4 (Glioblastoma) in the presence of EGFR amplification, TERT promoter mutation or the combined gain of chromosome 7 and loss of chromosome 10
- 46. Other changes • NOS (Not Otherwise Specified) • Diagnostic information (histological or molecular) needed to assign a specific WHO diagnosis is not available • Example: not enough tissue available or no resources available • NEC (Not Elsewhere Classified) • Results do not readily allow for a WHO diagnosis • Clinical, histological, or molecular mismatch
- 47. References • Louis D, Perry A, Wesseling P et al. The 2021 WHO Classification of Tumors of the Central Nervous System: A Summary. Neuro-Oncology. 2021;23(8):1231-51. doi:10.1093/neuonc/noab106 • Louis D, Perry A, Reifenberger G et al. The 2016 World Health Organization Classification of Tumors of the Central Nervous System: A Summary. Acta Neuropathol. 2016;131(6):803-20. doi:10.1007/s00401-016-1545-1 – Pubmed • International Agency for Research on Cancer, Otmar D. Wiestler. WHO Classification of Tumours of the Central Nervous System. (2016) ISBN: 9789283244929 • GreenBerg 9th edition • Davis FG, McCarthy BJ. Current epidemiological trends and surveillance issues in brain tumours. Expert Rev Anticancer Ther2001;1:395–401.
- 48. Thank you