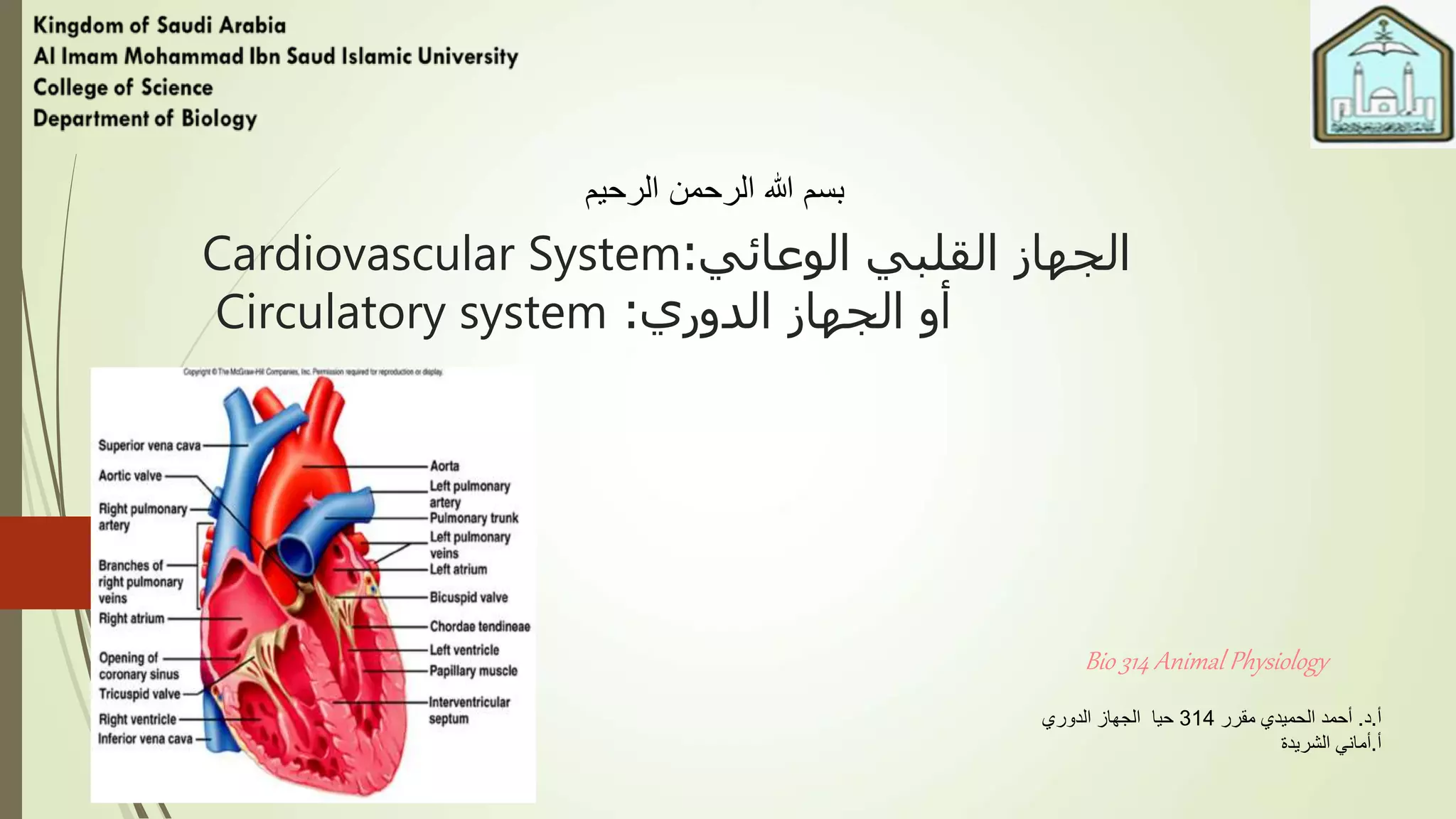
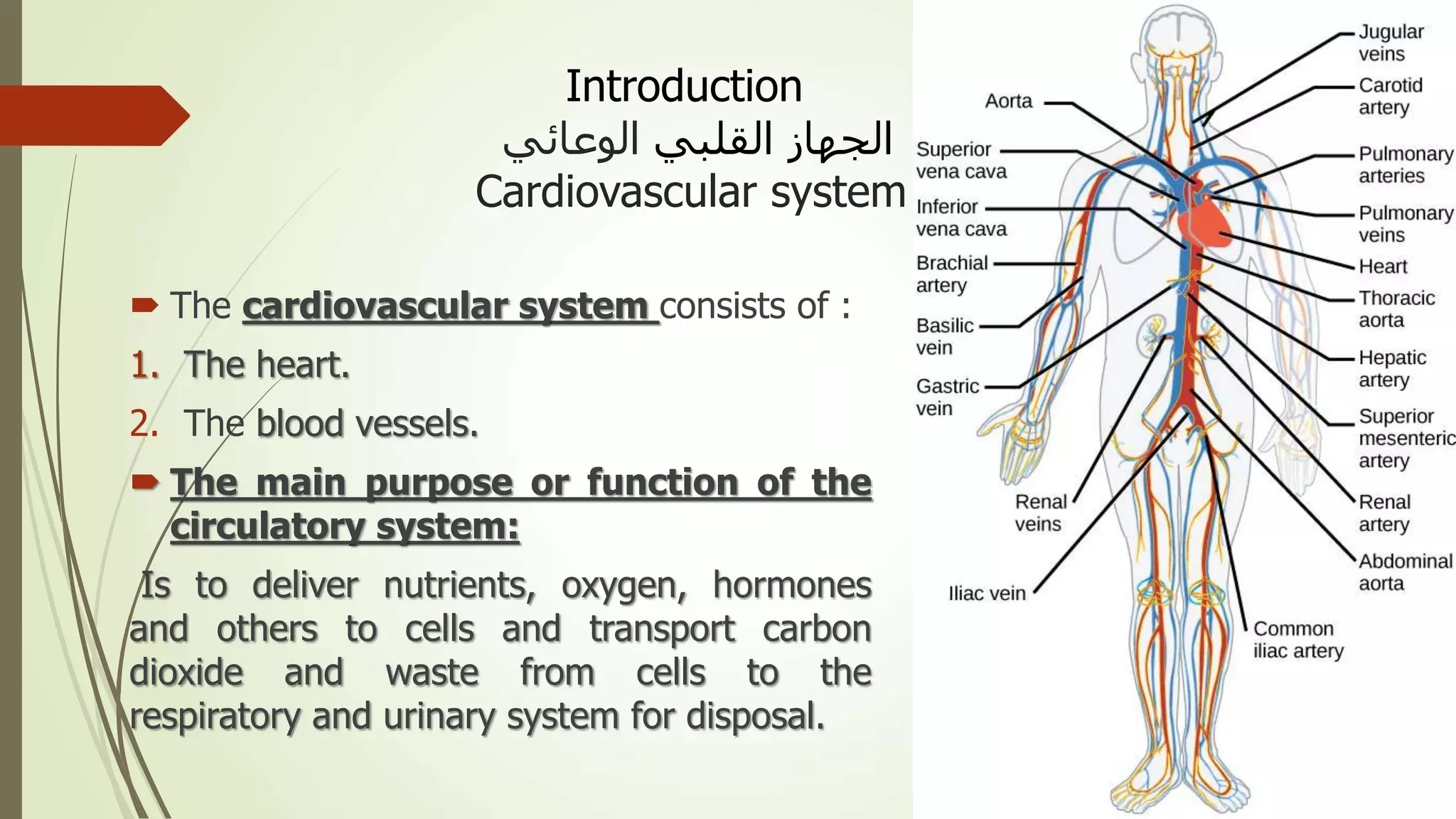
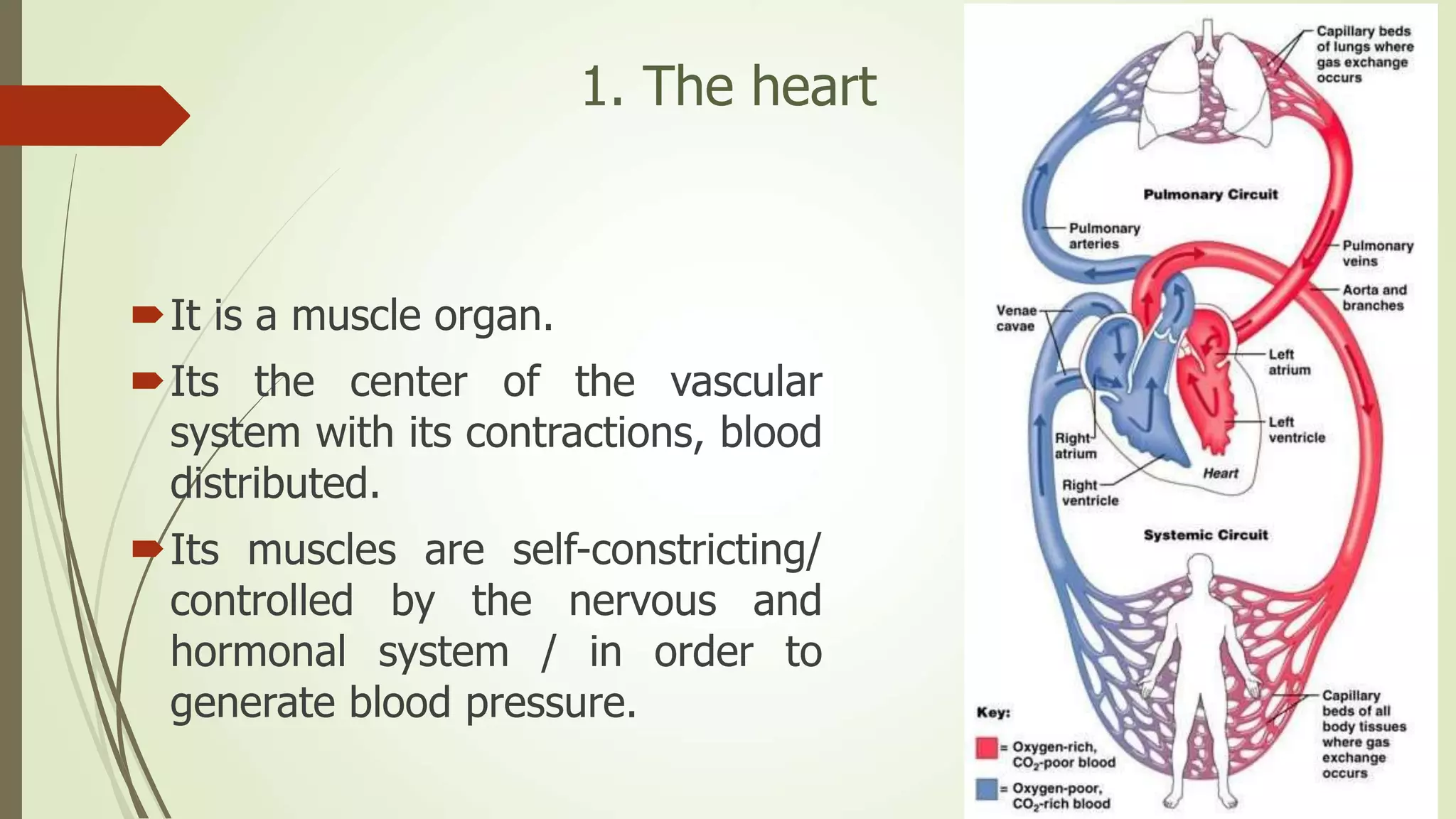
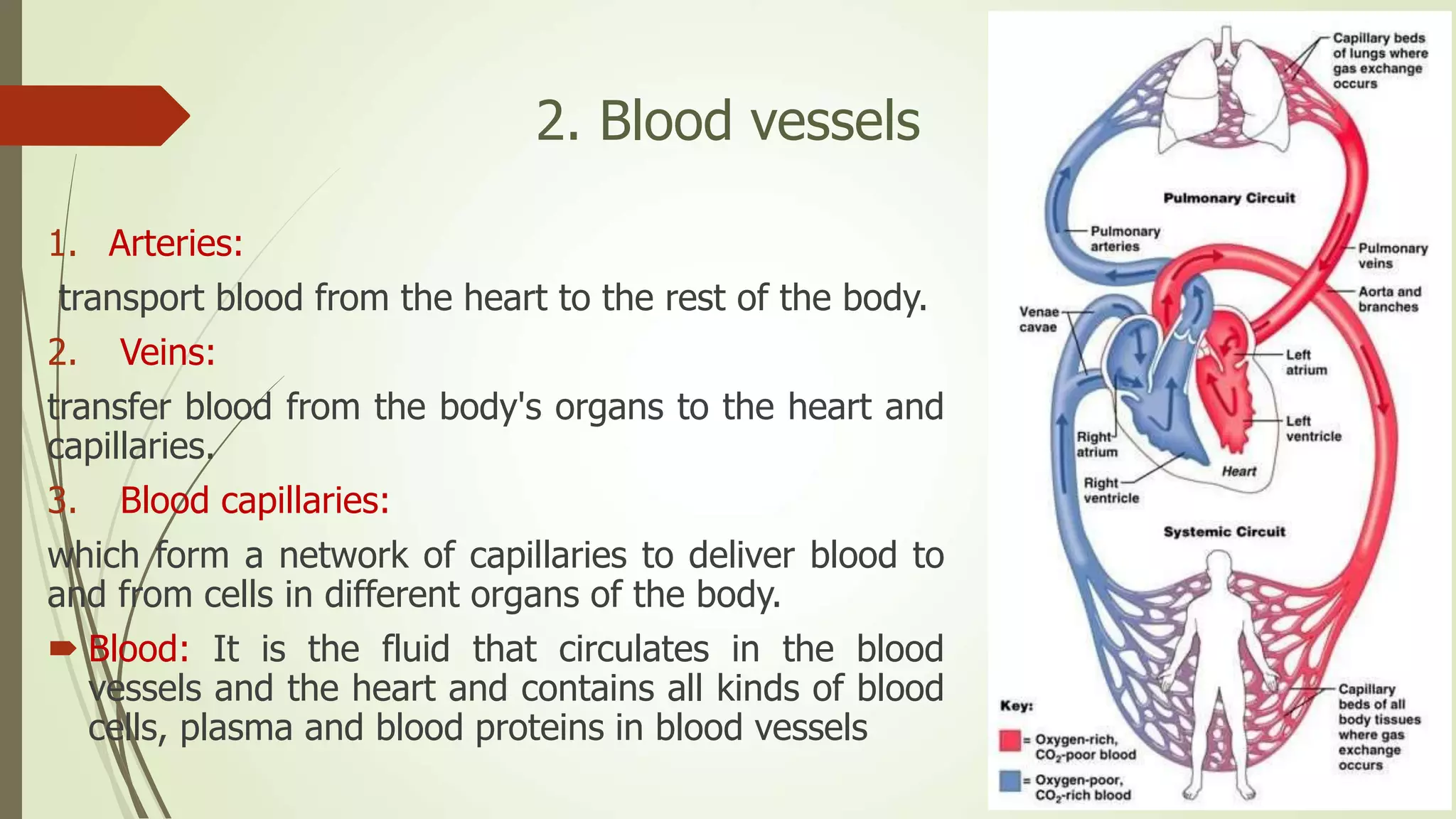
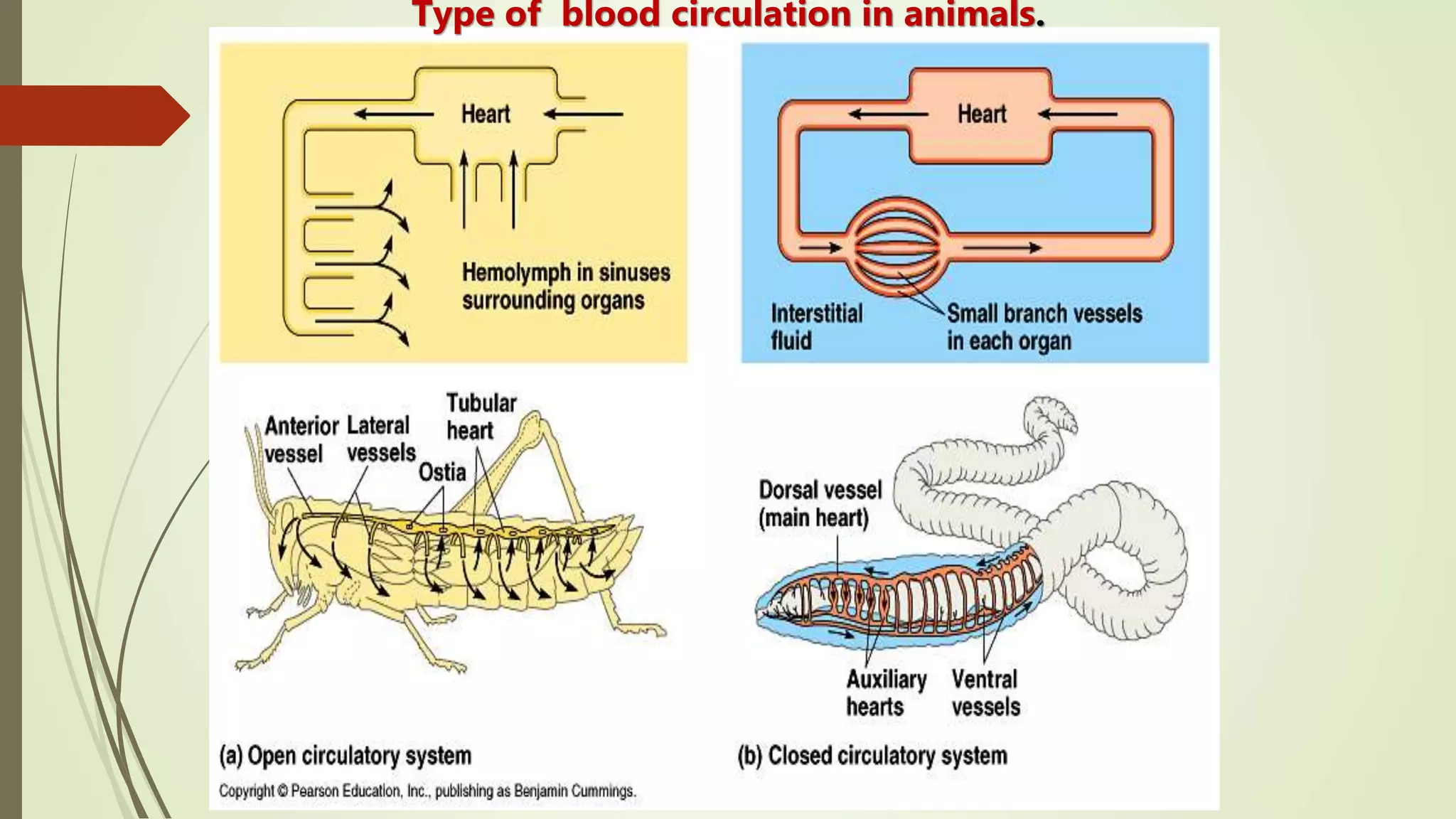
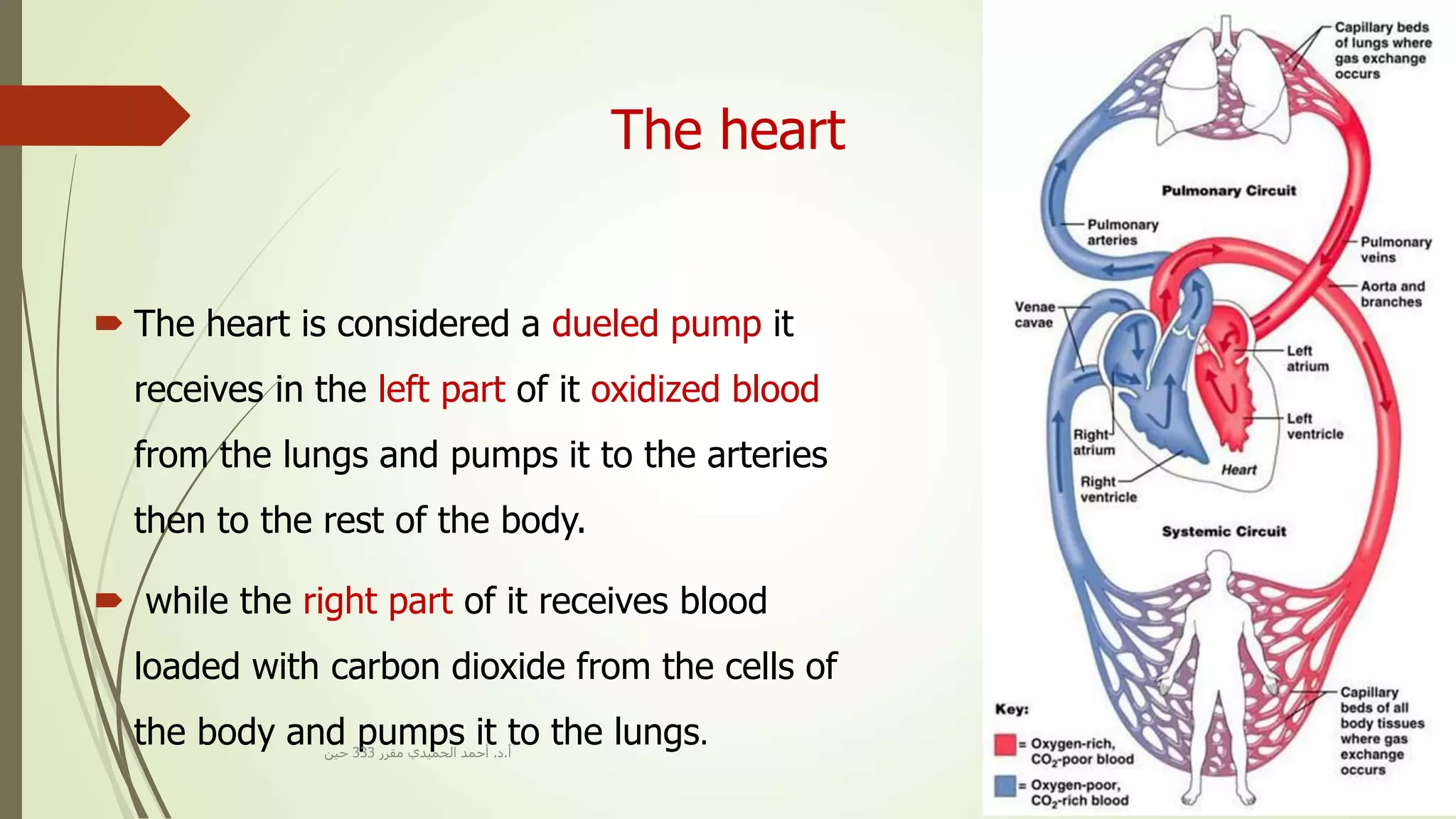
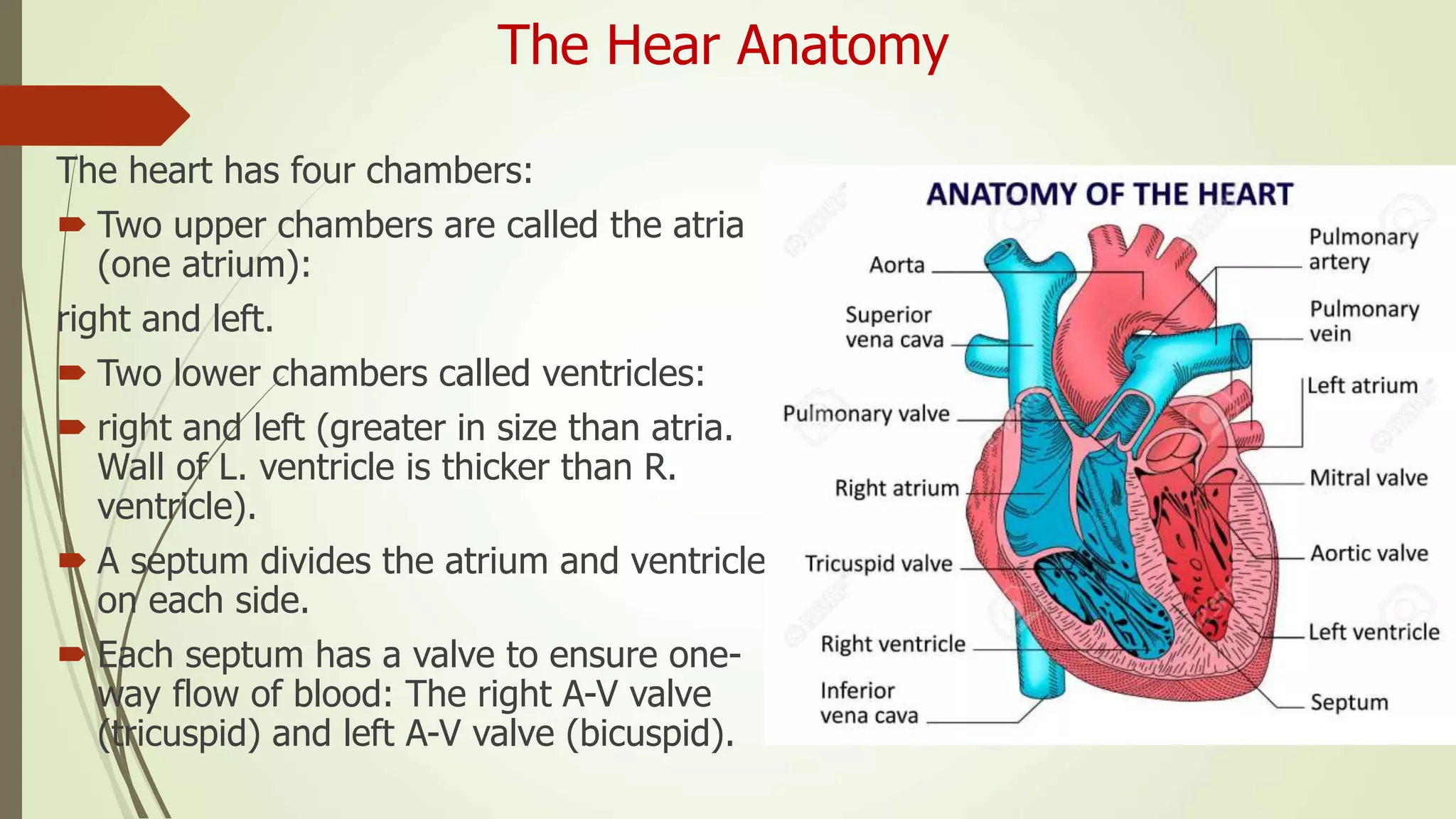
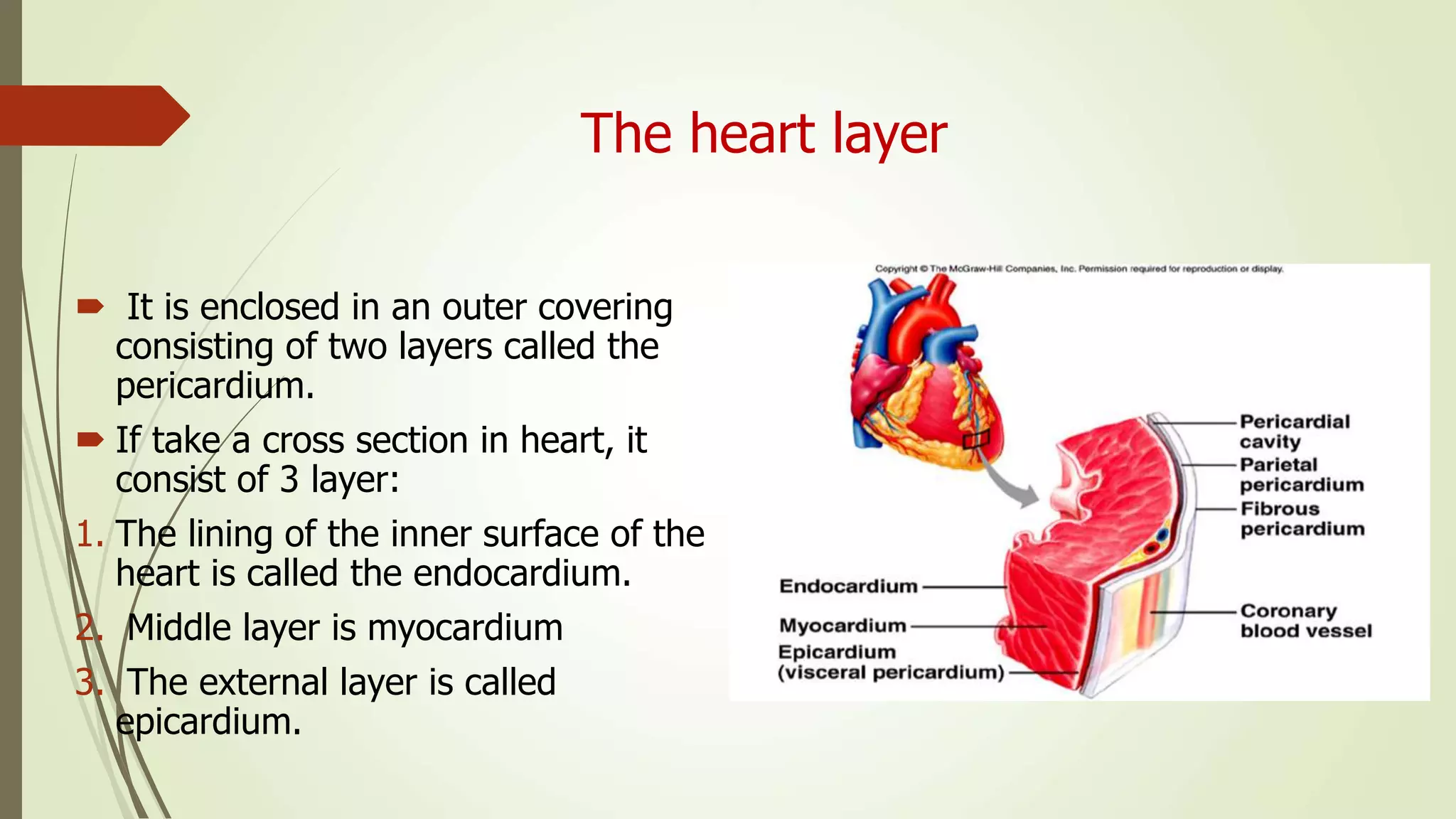
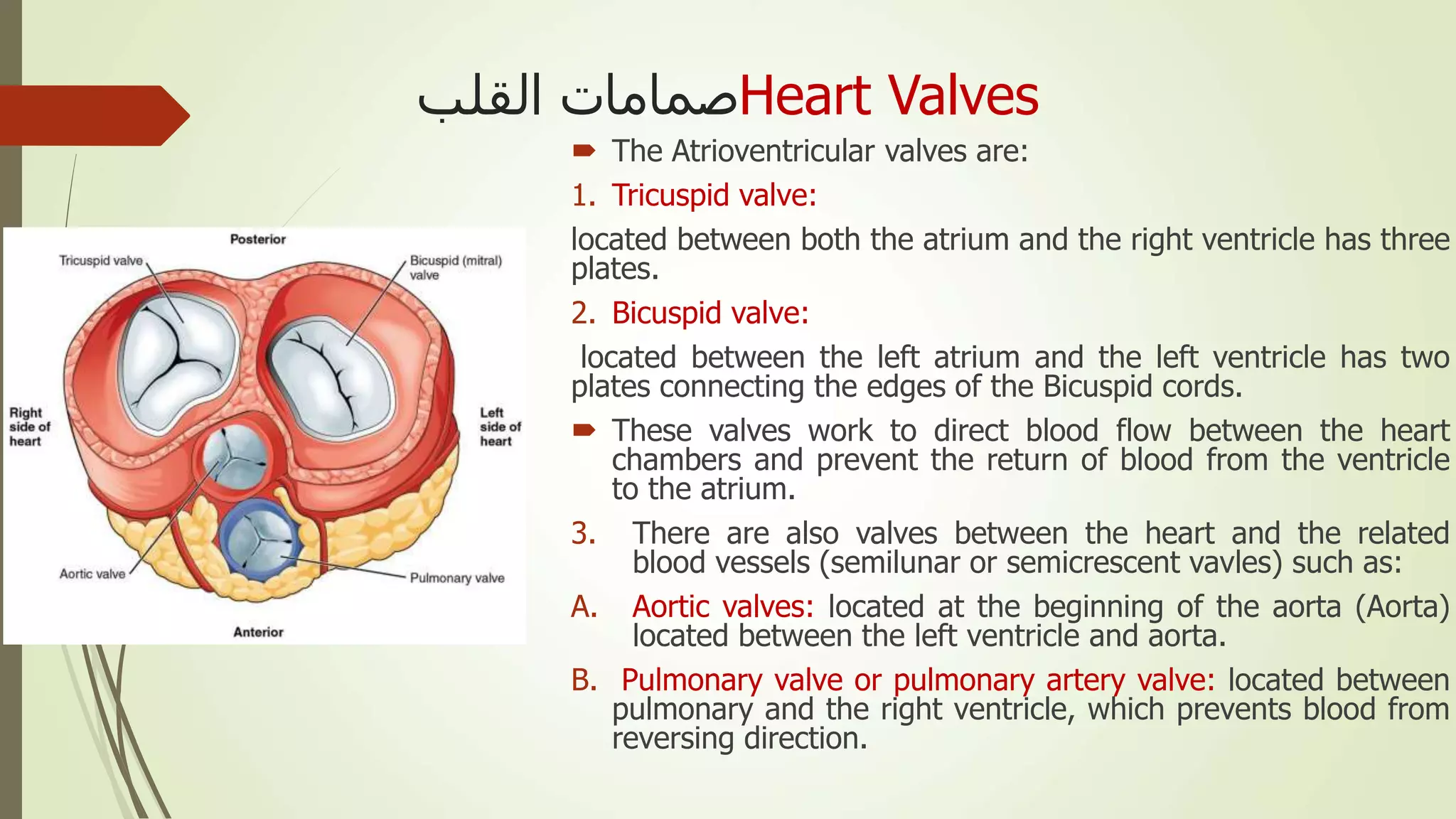
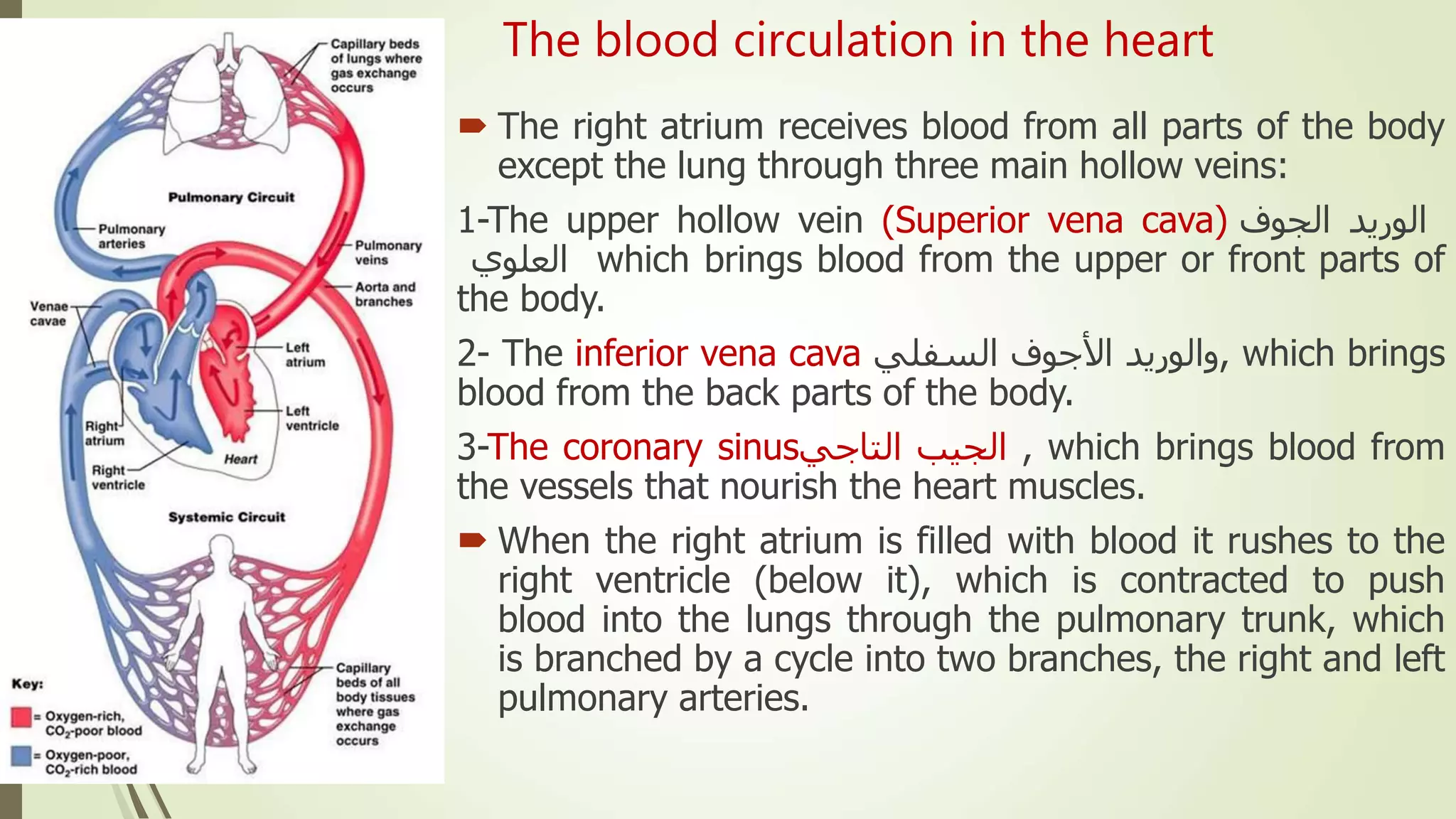
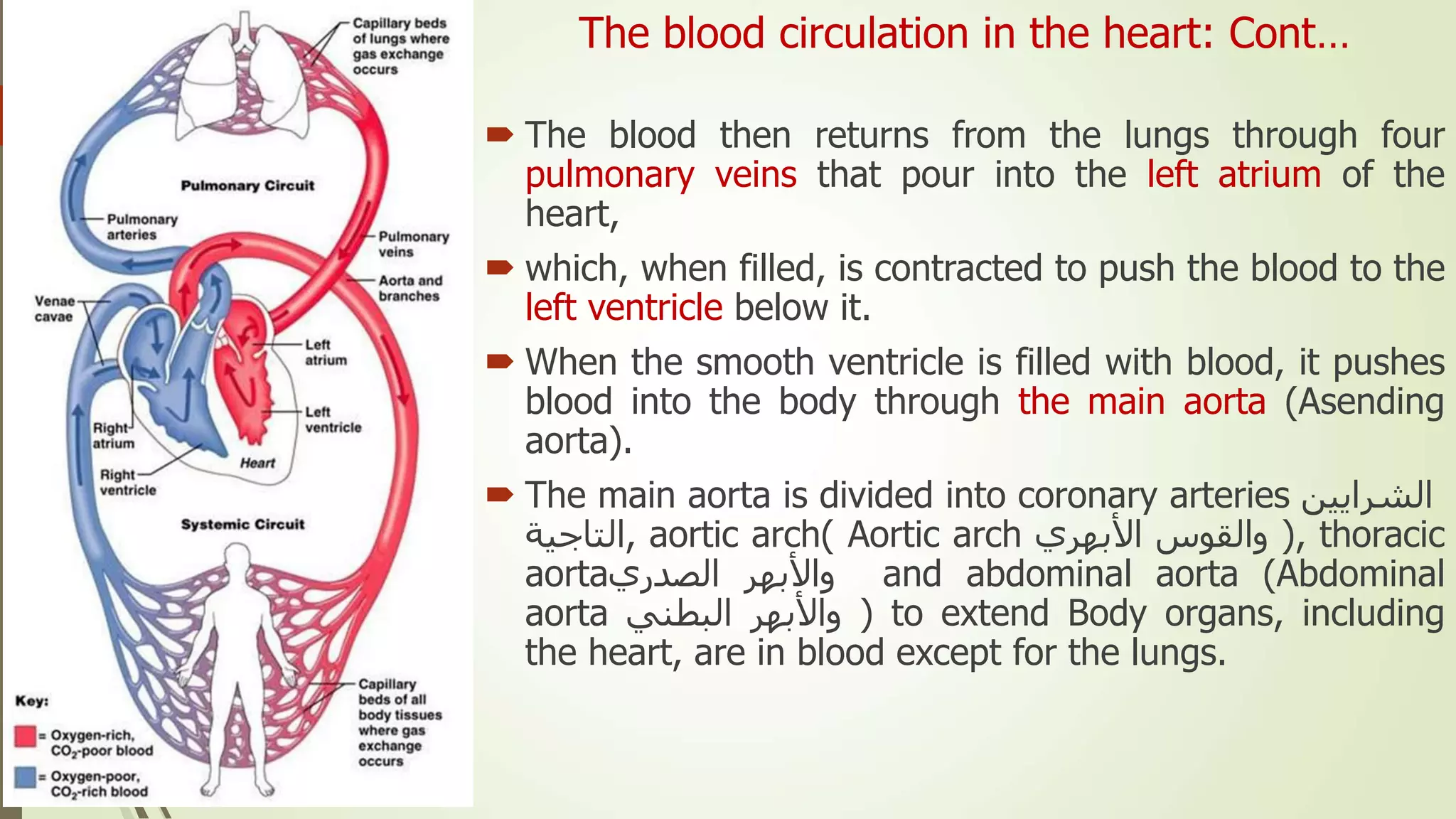
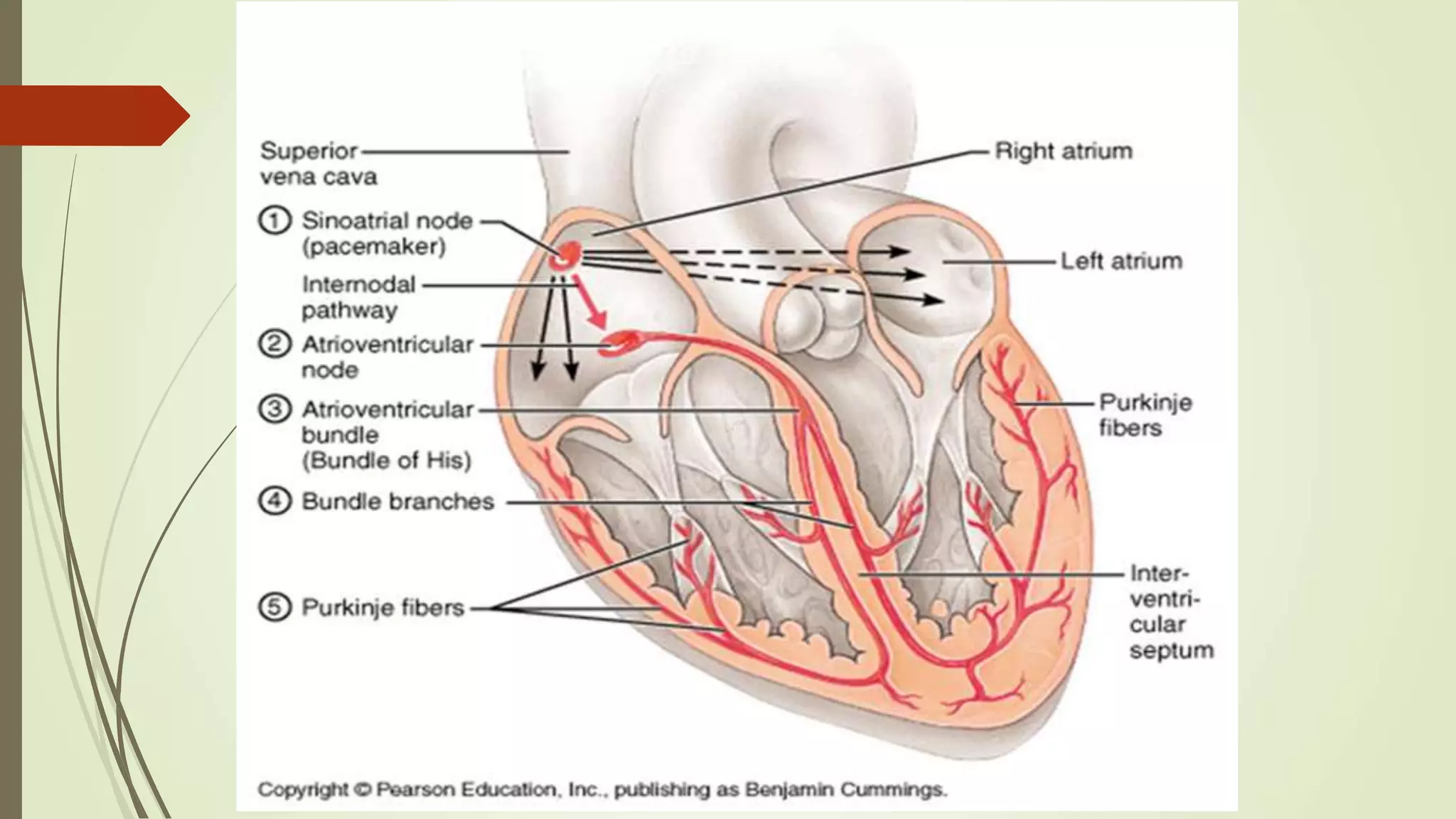
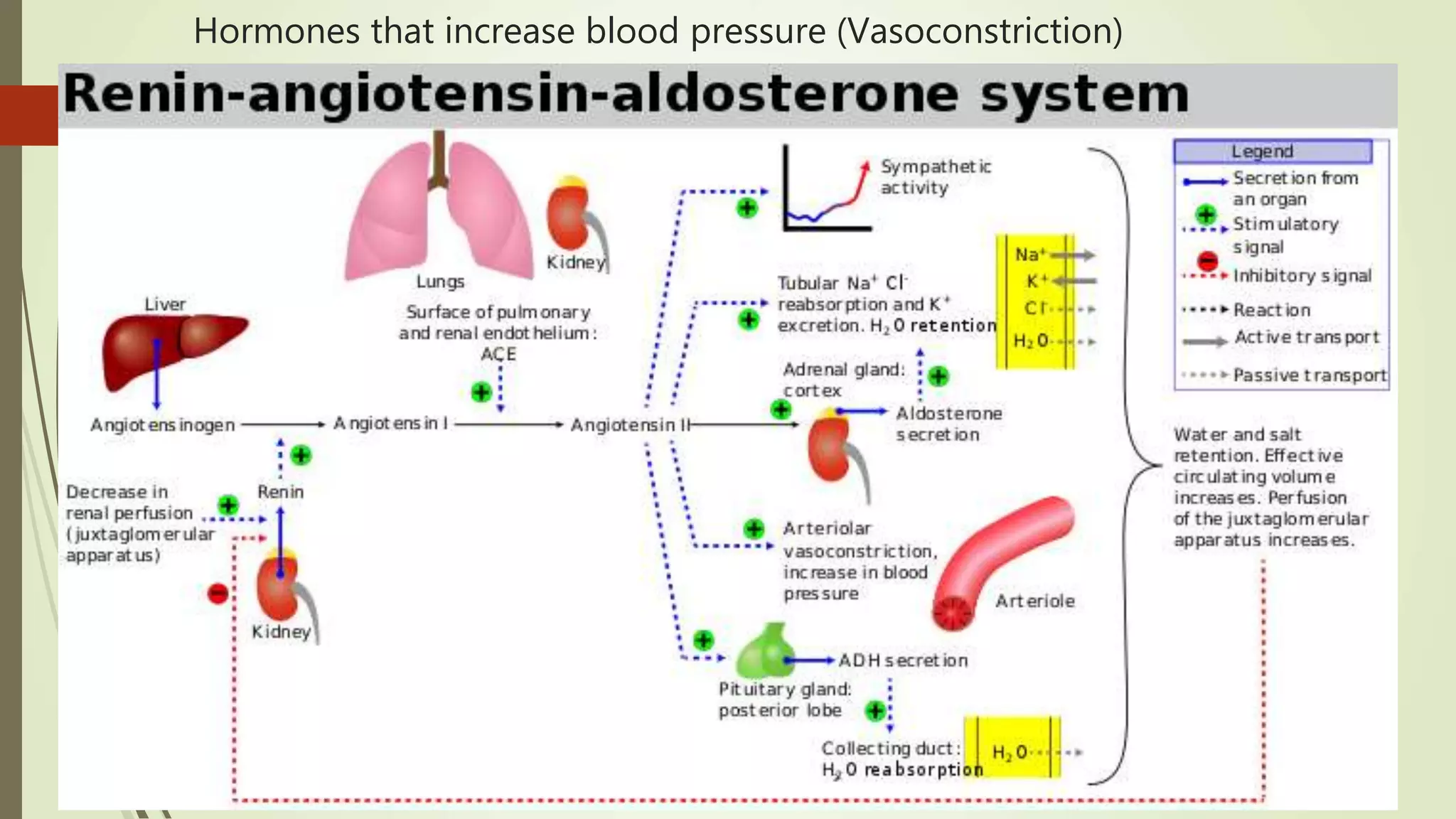
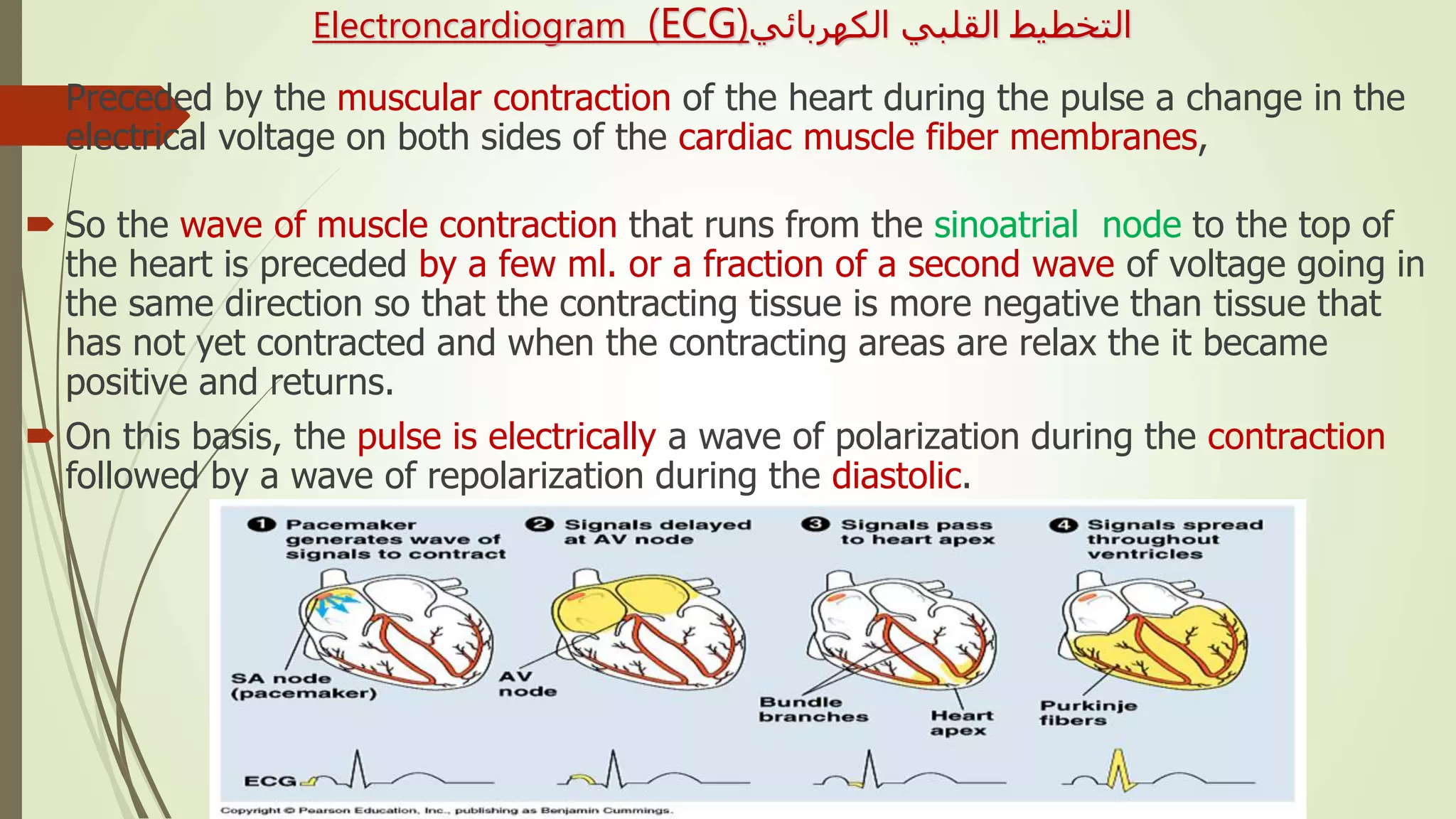
The document provides an overview of the cardiovascular system. It discusses the main components which include the heart and blood vessels. The heart is made up of four chambers - two atria and two ventricles separated by valves. Blood flows from the heart through arteries to the body and returns to the heart via veins. The circulatory system transports nutrients, oxygen, hormones and waste products around the body. There are two main types of blood circulation - closed circulation found in vertebrates and open circulation in invertebrates.