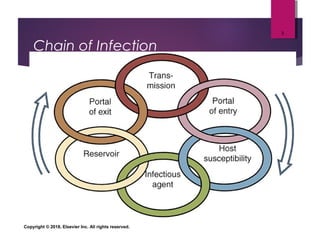
1) The document discusses infection control and medical asepsis, including hand hygiene, isolation precautions, and caring for patients with multidrug-resistant organisms.
2) Key aspects of infection control are reducing transmission of infections, protecting patients and healthcare providers, and practicing proper hand hygiene.
3) Medical asepsis and isolation precautions aim to reduce the spread of organisms and prevent the transfer of infections between patients or from patients to healthcare providers.