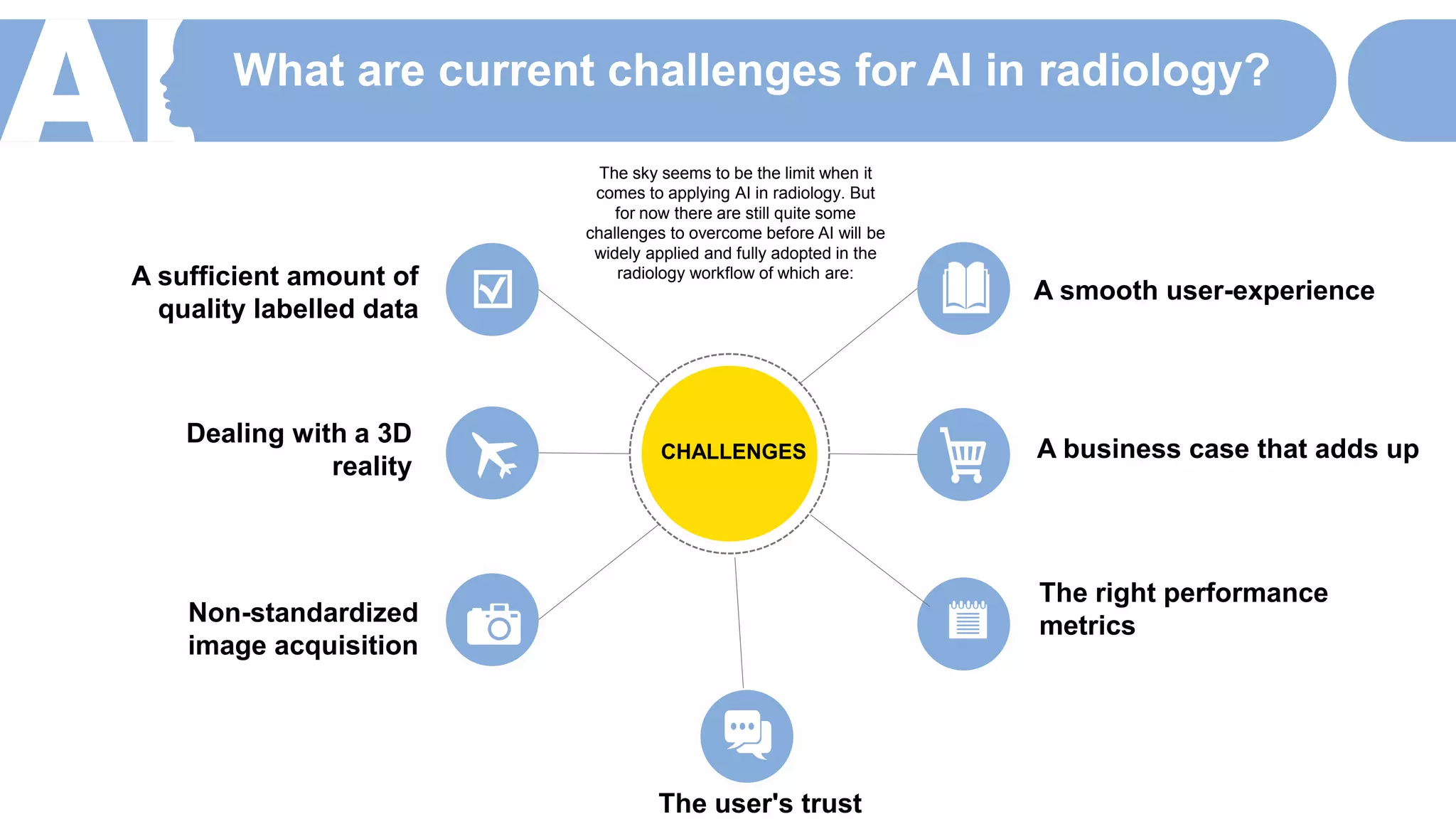
The document discusses the role of artificial intelligence (AI) in radiology, highlighting its potential to enhance diagnostic accuracy and improve workflow efficiency while recognizing inherent challenges such as data quality and user trust. AI can assist radiologists by taking over repetitive tasks and providing second opinions, ultimately aiming to improve patient outcomes. However, successful implementation requires addressing concerns related to user experience, financial viability, and robust performance metrics.