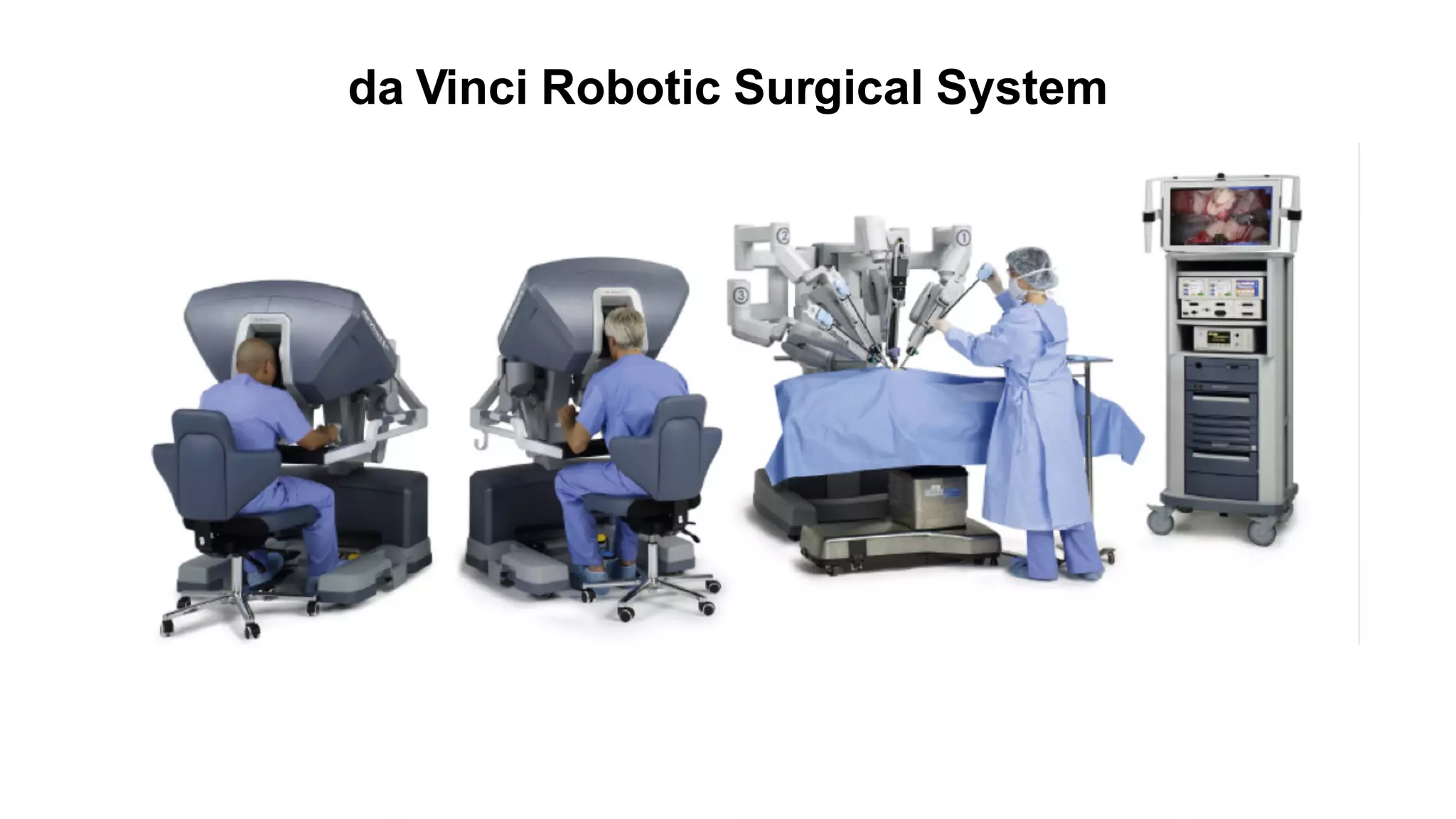
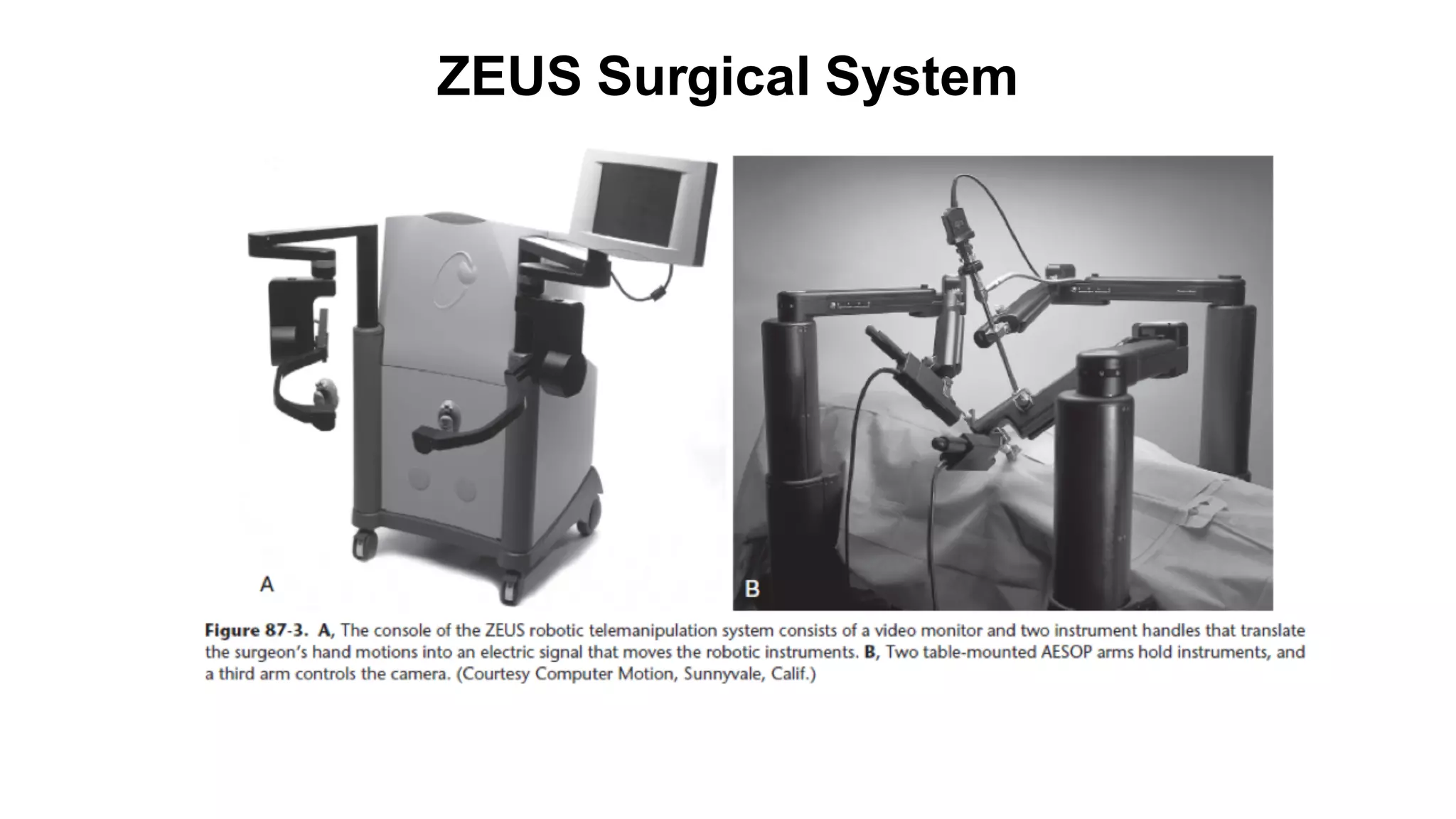
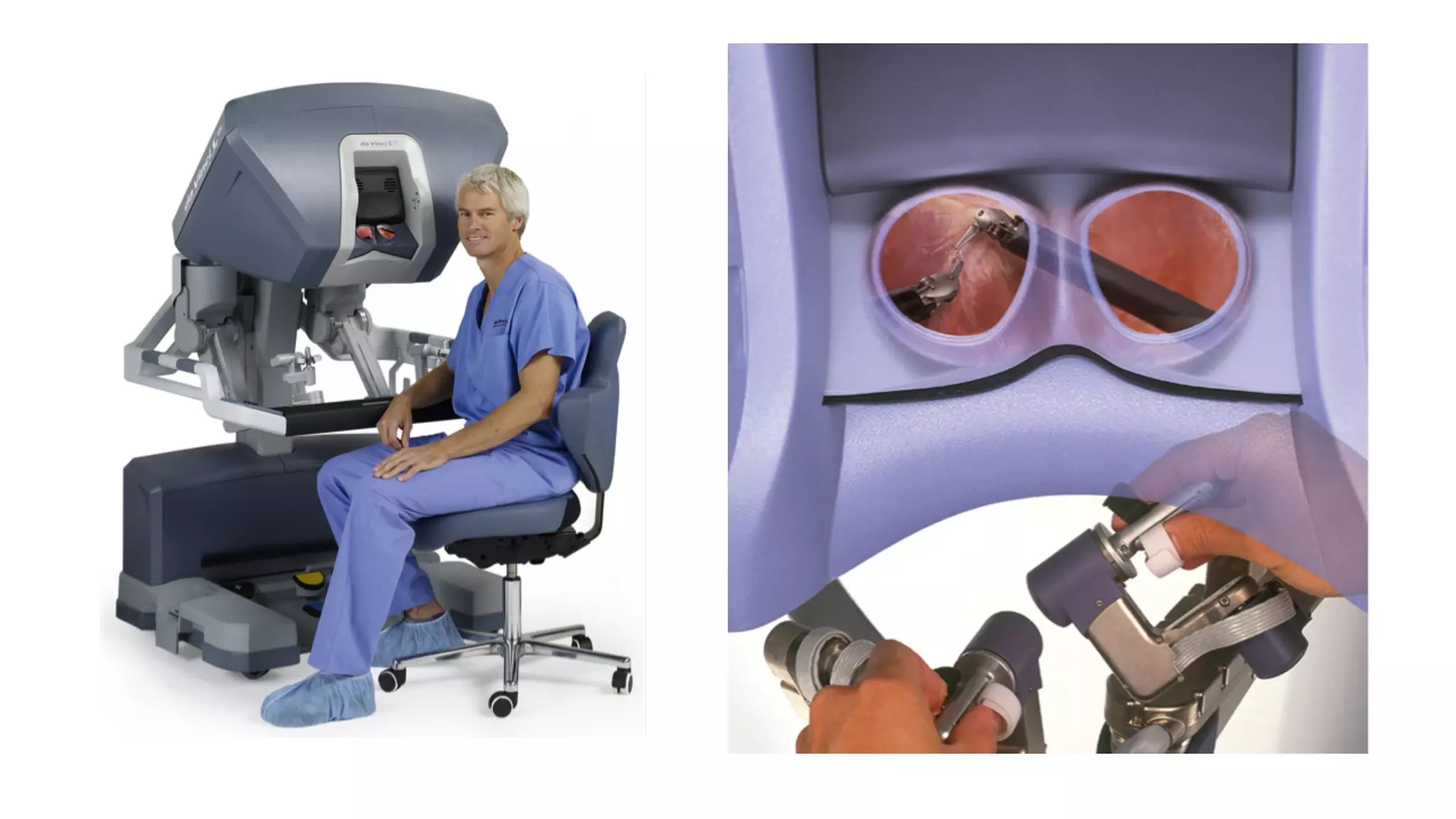
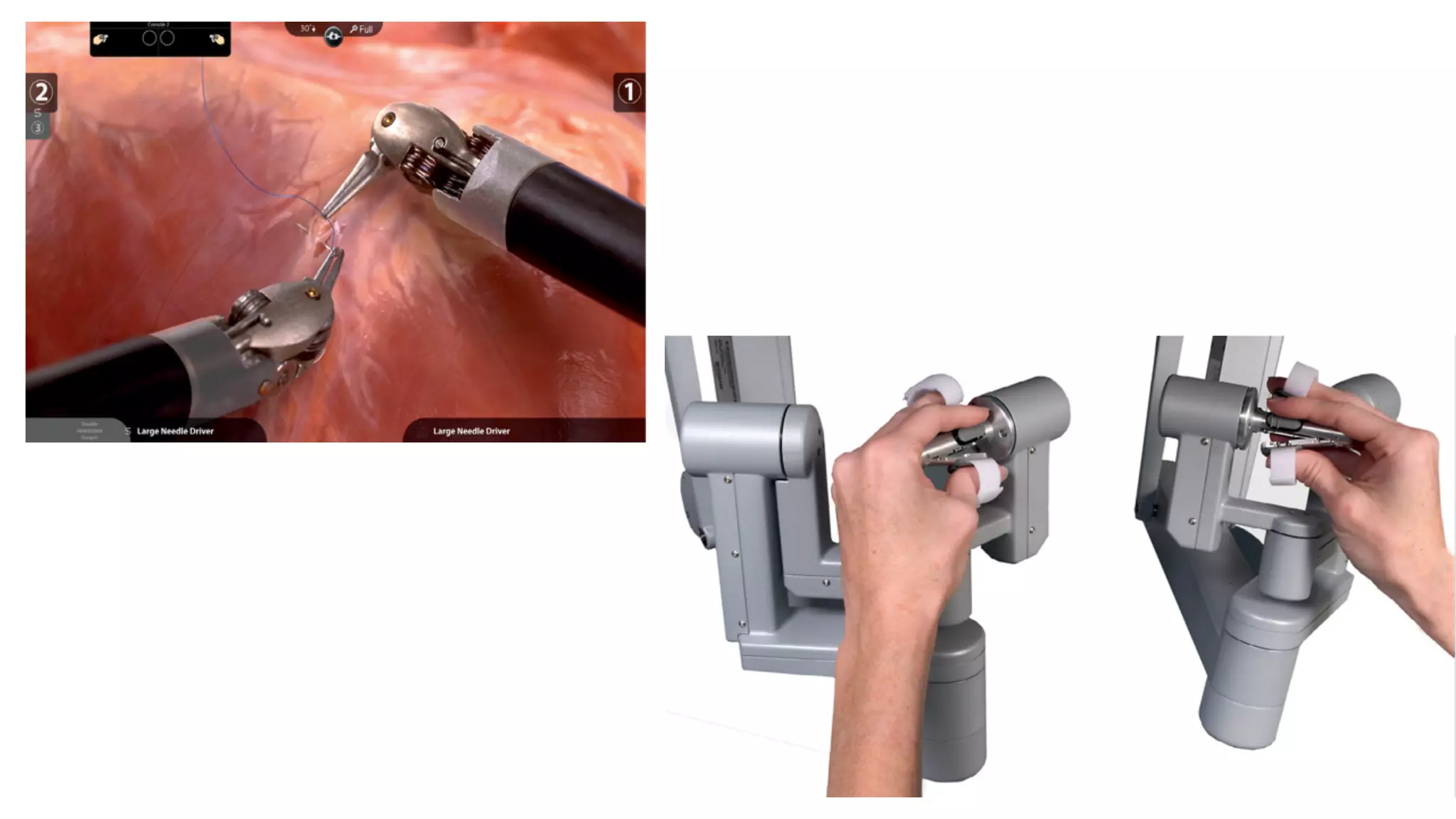
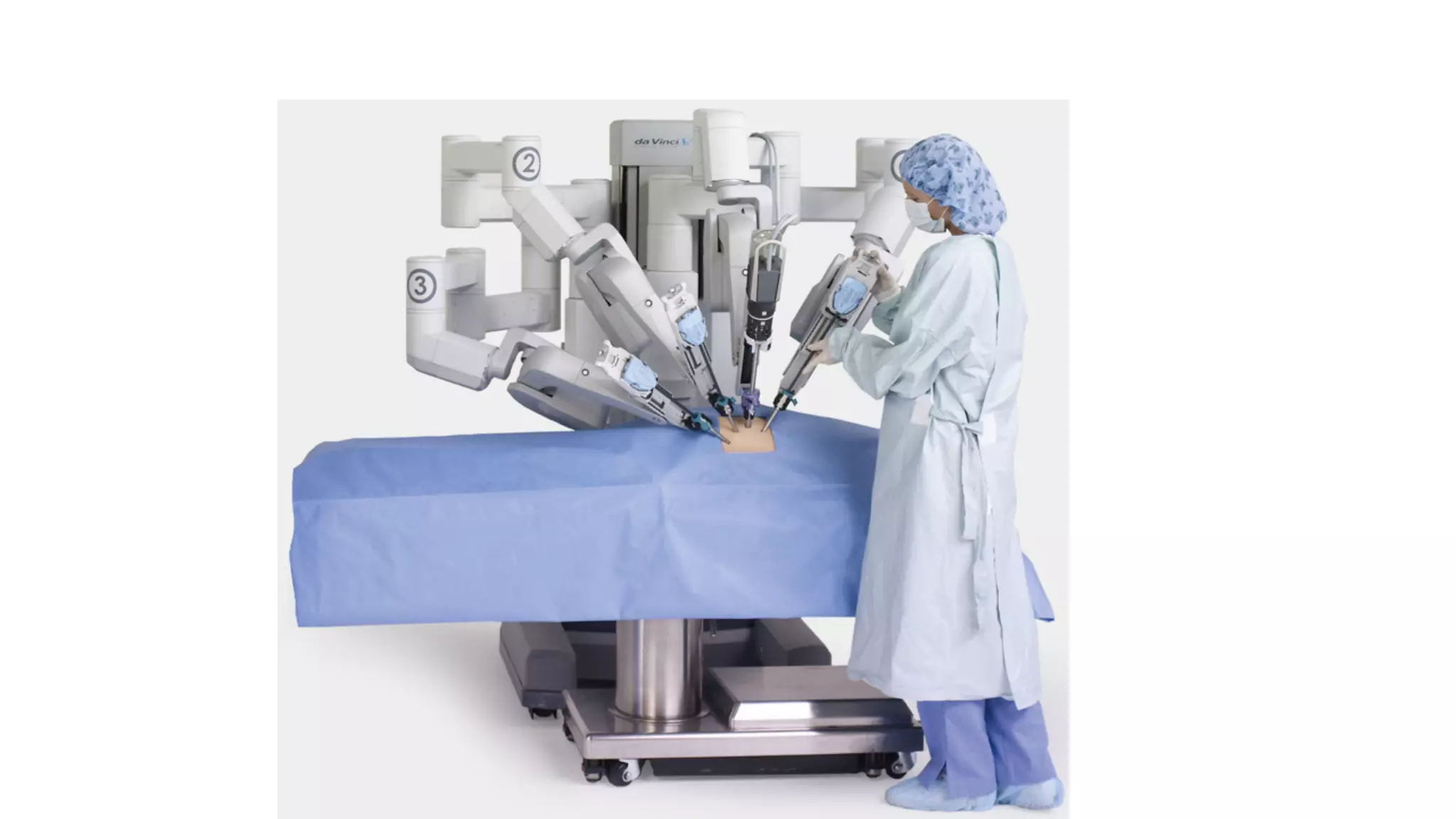
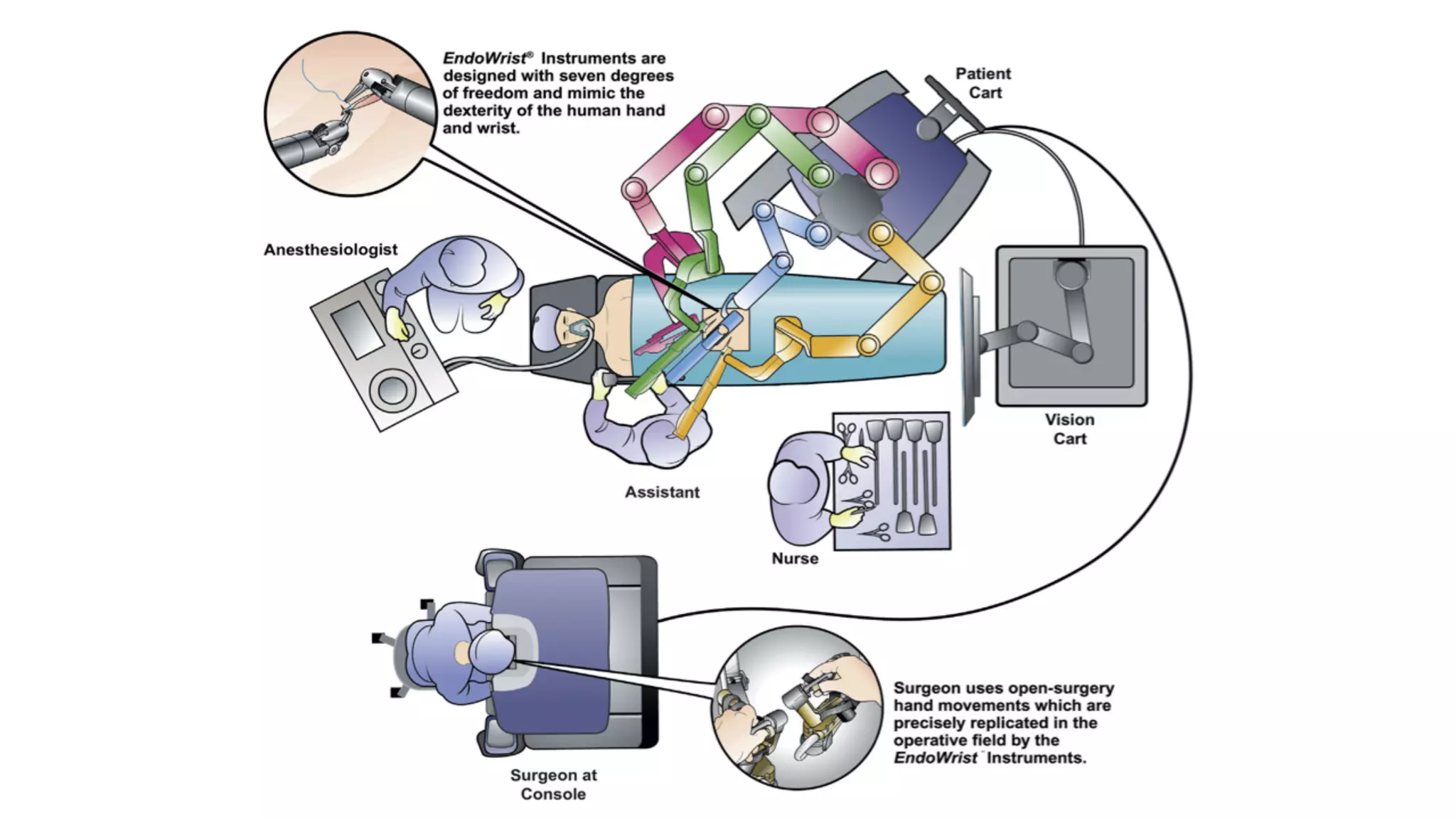
Robotic surgery offers benefits to patients such as less pain, shorter recovery times, and improved cosmetic results compared to open surgery. However, it presents unique challenges for anesthesiologists. The patient must be optimally positioned before docking the robotic system, as repositioning is difficult afterward. Access to the patient is also limited by the size and positioning of the robot. Physiologic changes like hypothermia and respiratory acidosis related to prolonged pneumoperitoneum must be monitored and addressed. Pressure points require special padding due to prolonged immobilization.