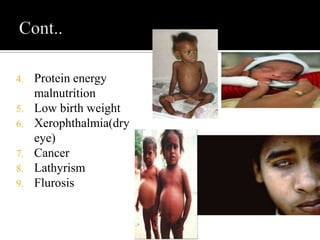
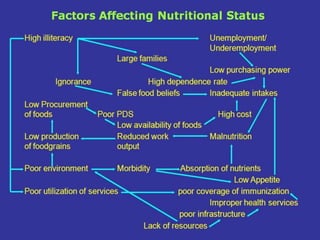
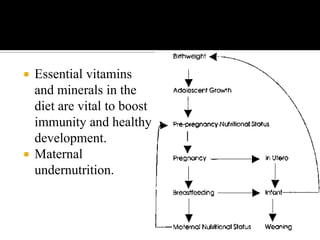
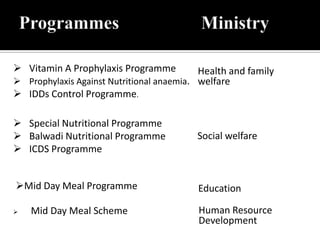
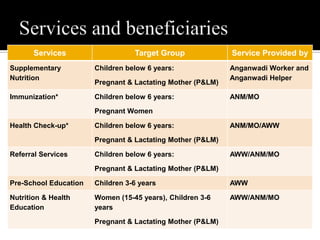
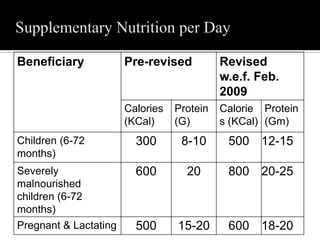
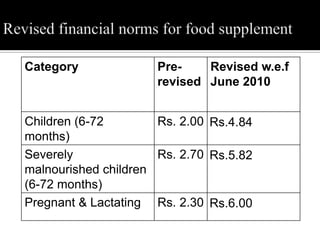
The document discusses major nutritional problems in India including communicable diseases, population issues, environmental sanitation, medical care access, and specific deficiencies like anemia, iodine deficiency, obesity, and malnutrition. It notes that while mortality has decreased, undernutrition reduction has been slower. Most children and women suffer from anemia and micronutrient deficiencies. Nutrition is critical for health, development, learning, and breaking cycles of poverty. The document outlines several government programs aimed at improving nutrition, including ICDS, vitamin A supplementation, anemia prophylaxis, and iodine deficiency disorder control. It discusses the objectives, beneficiaries, and implementation of these programs.