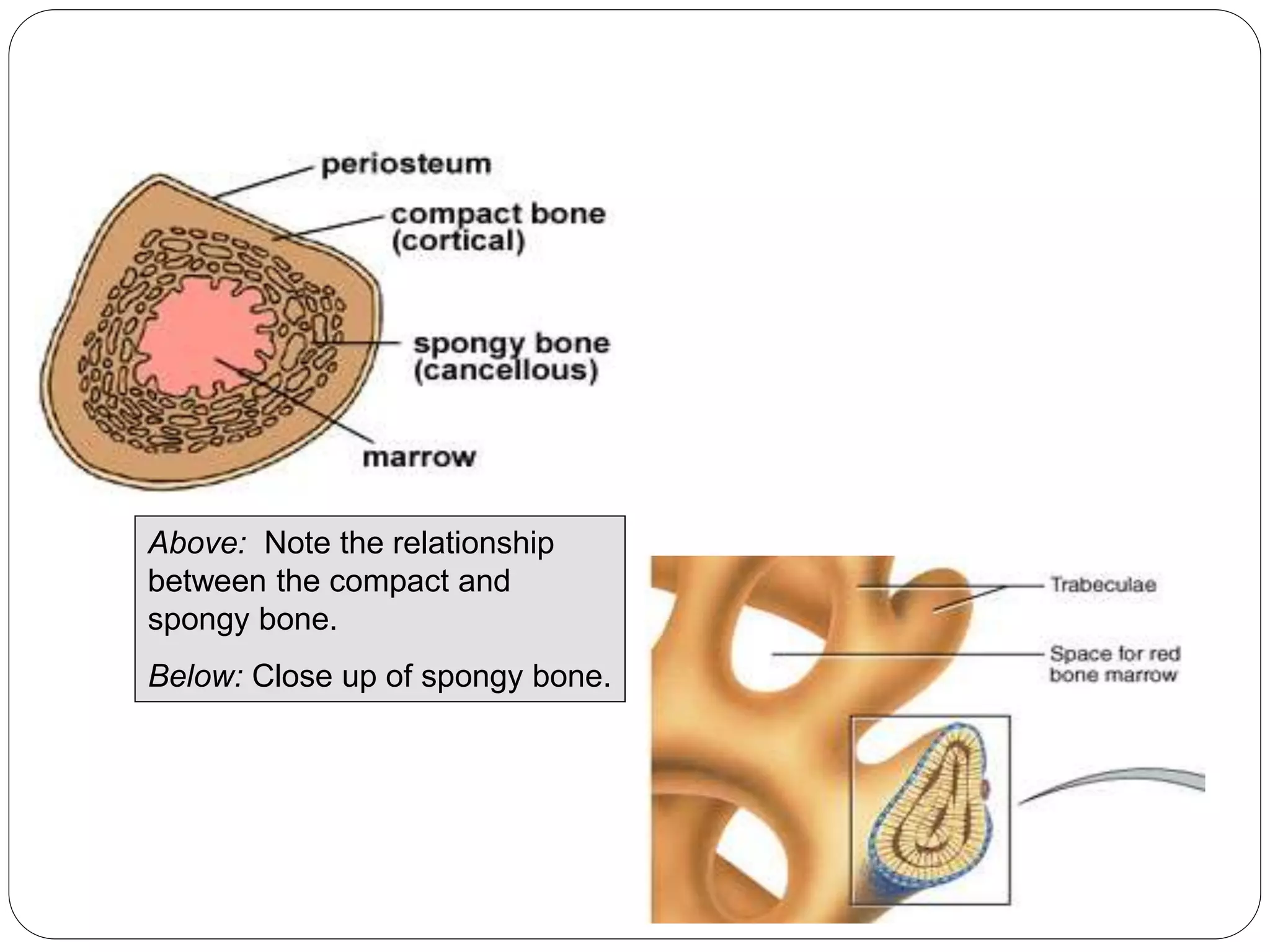
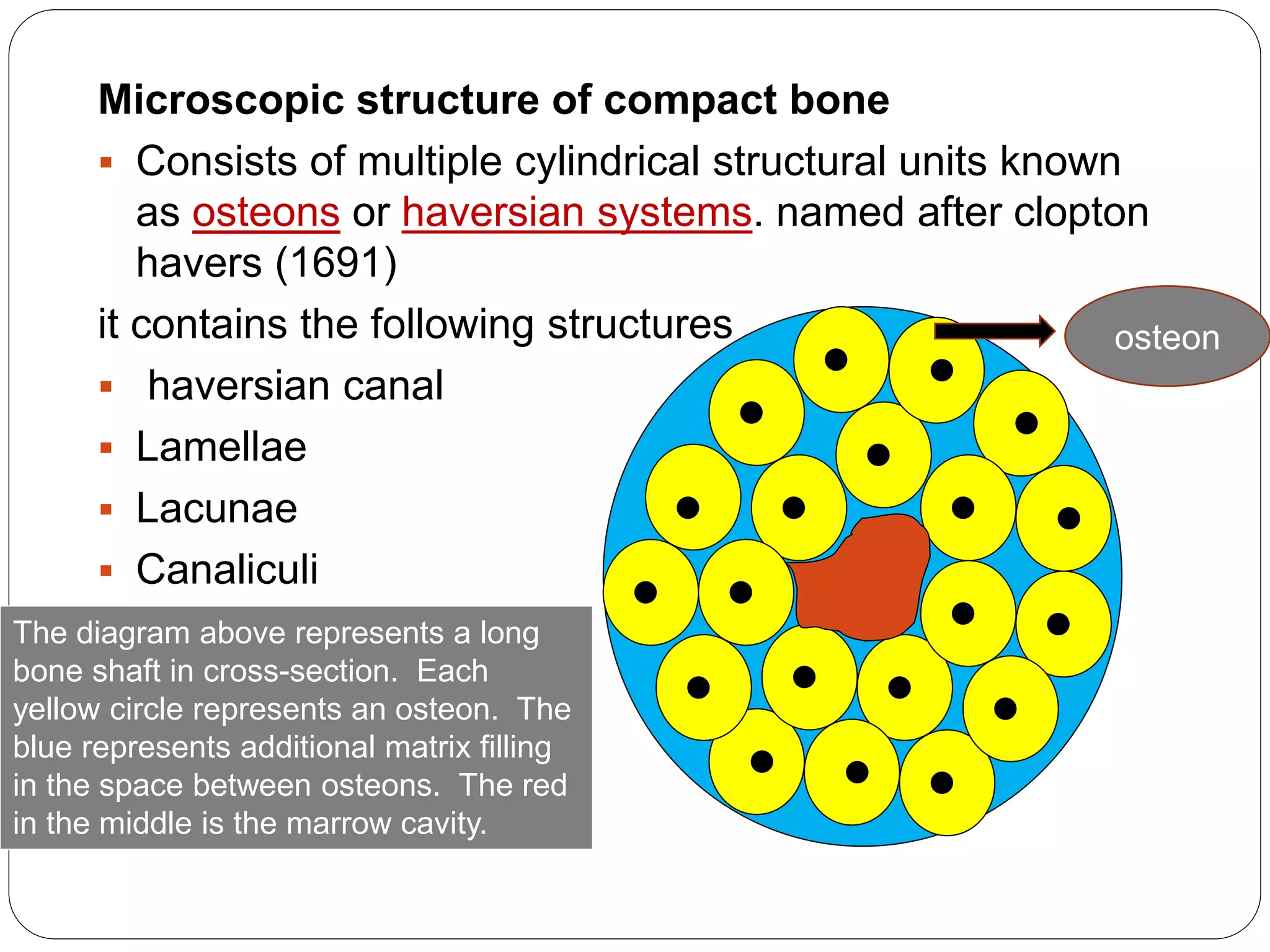
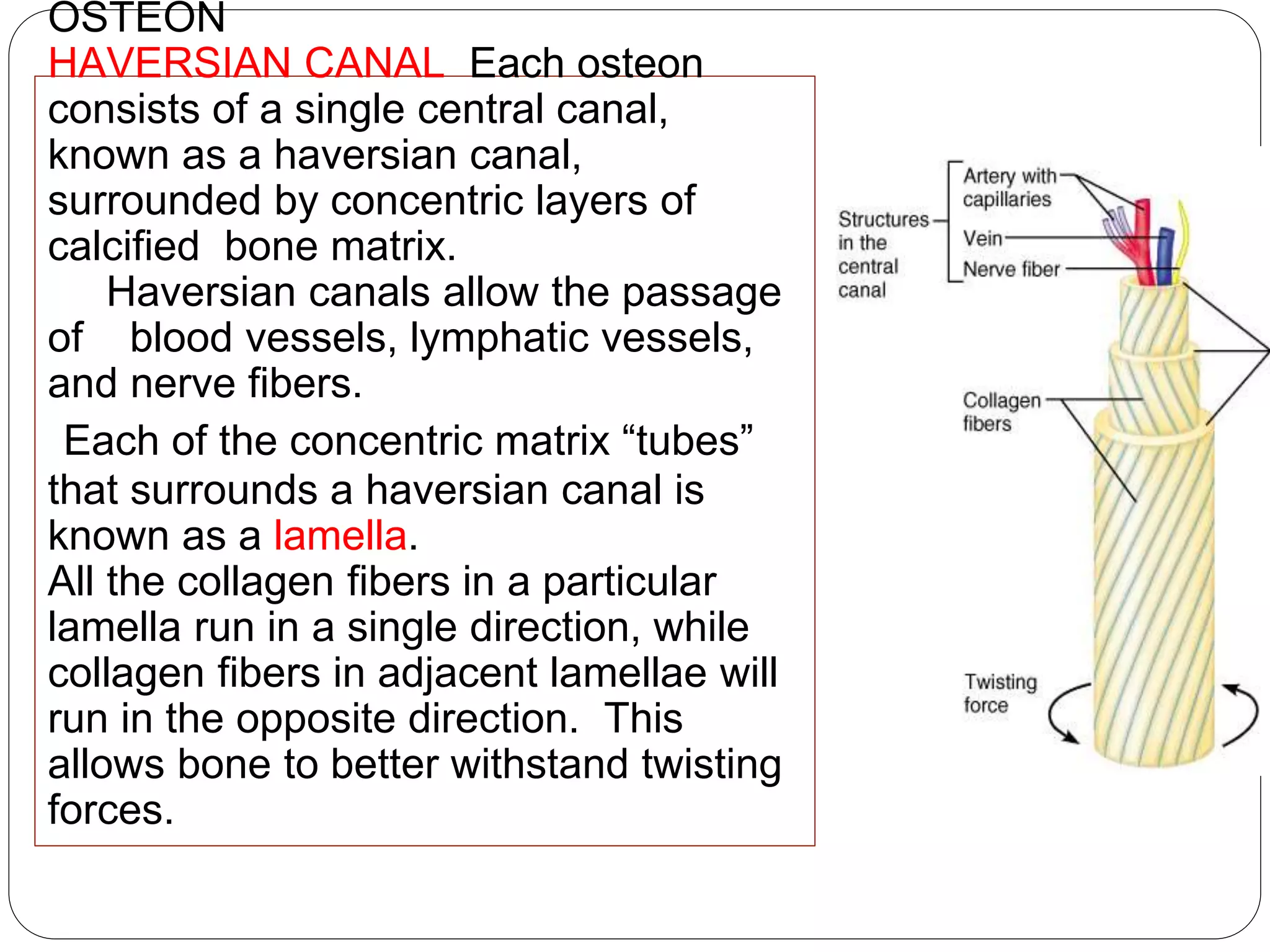
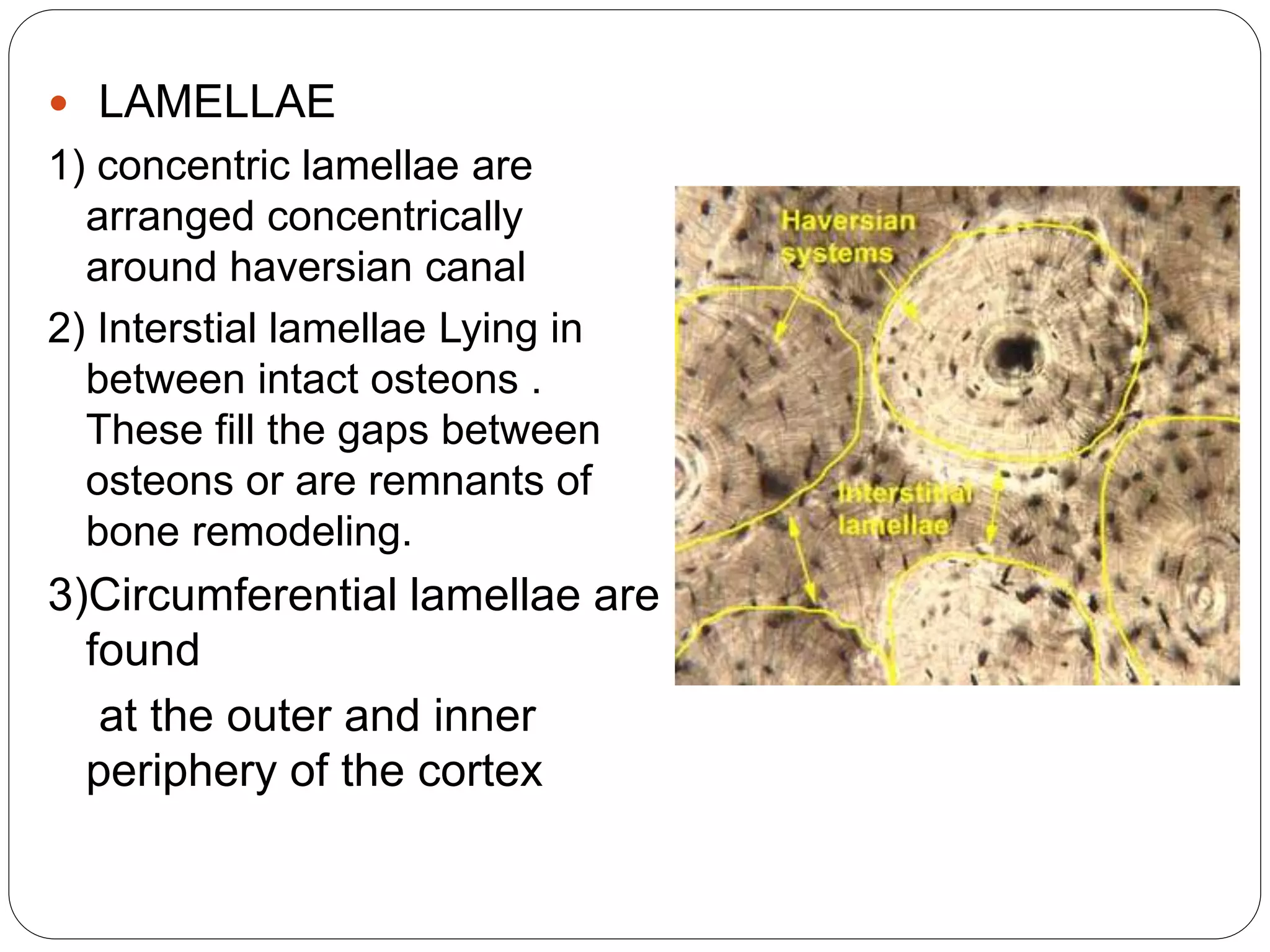
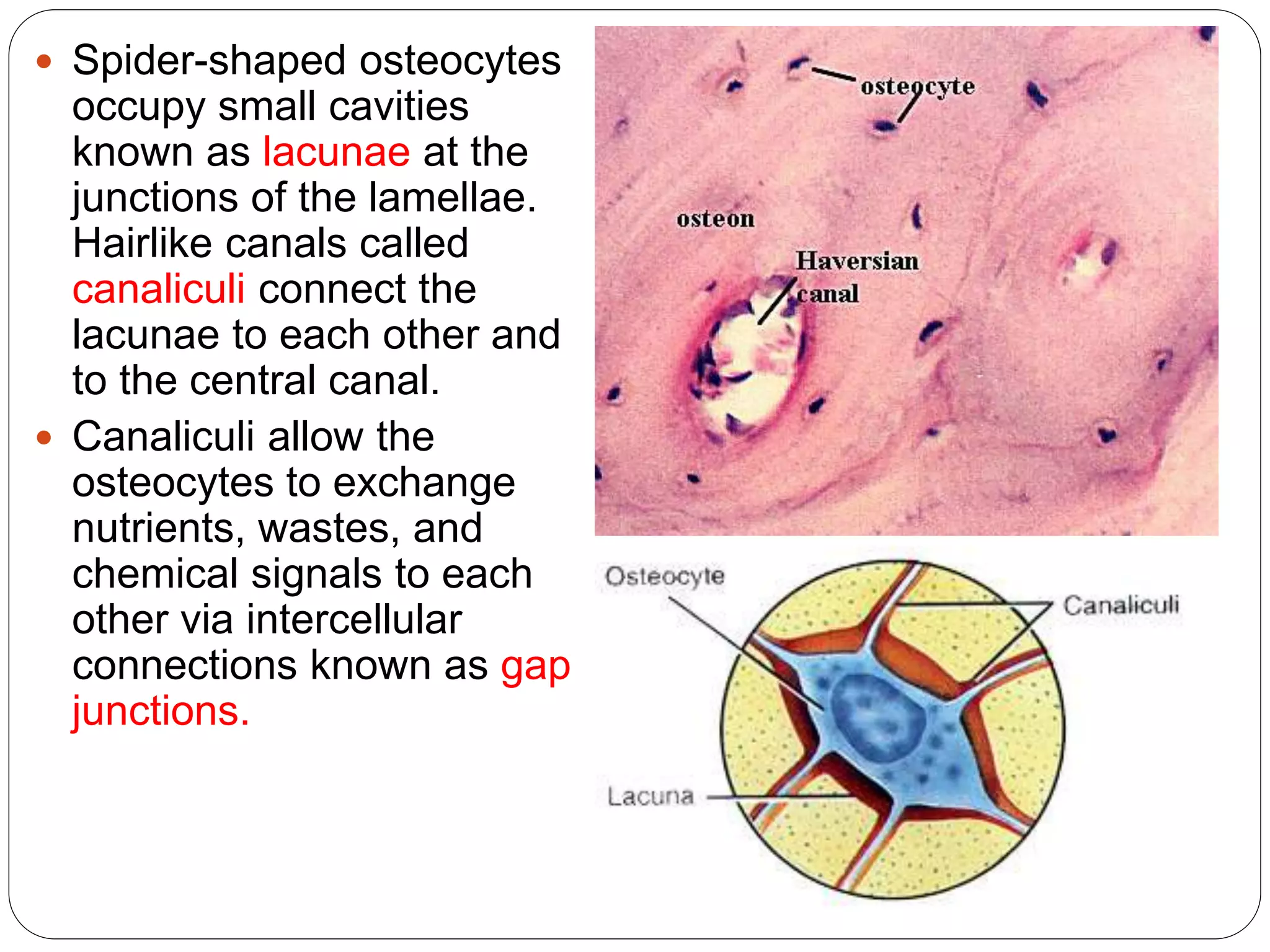
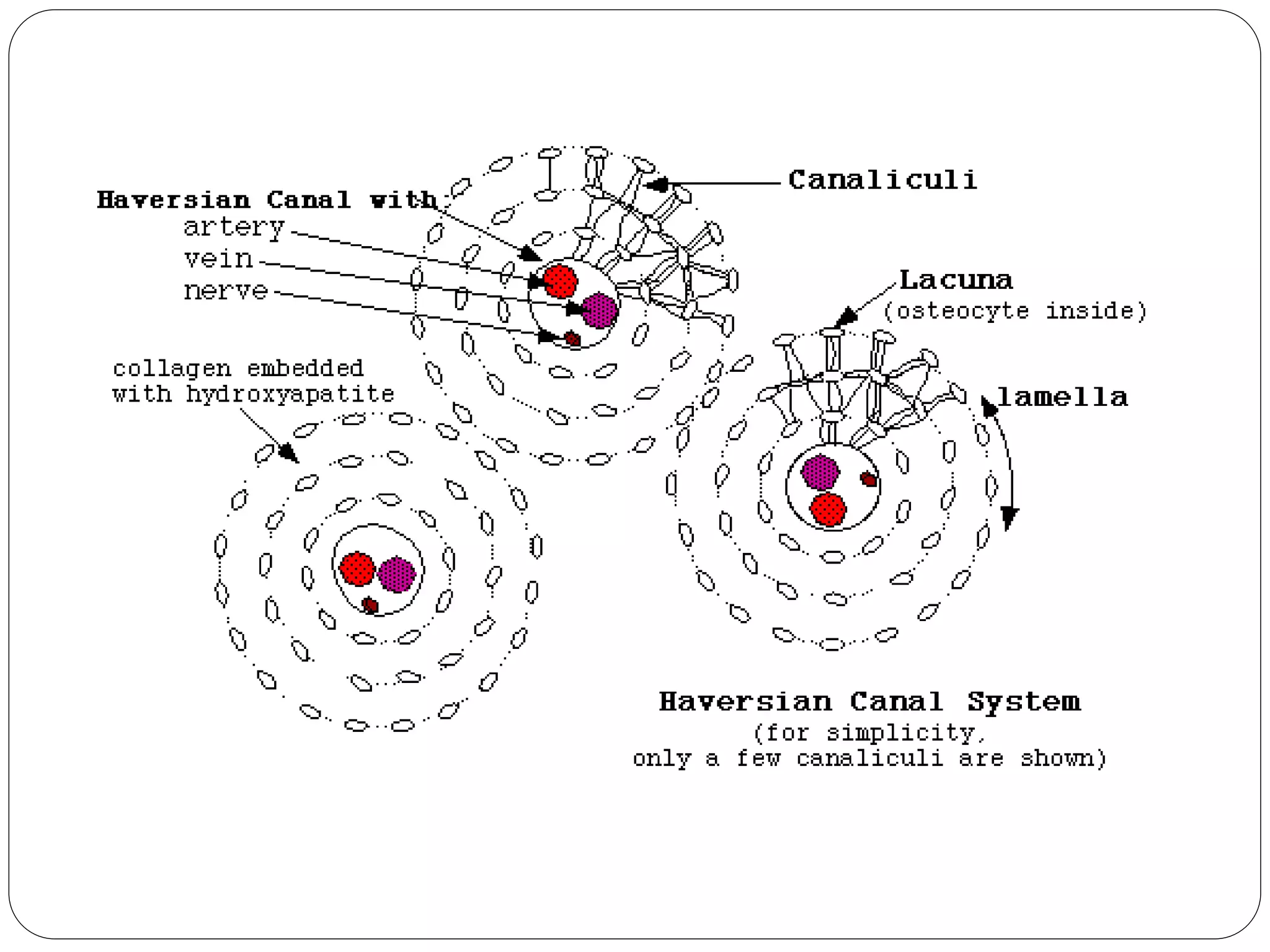
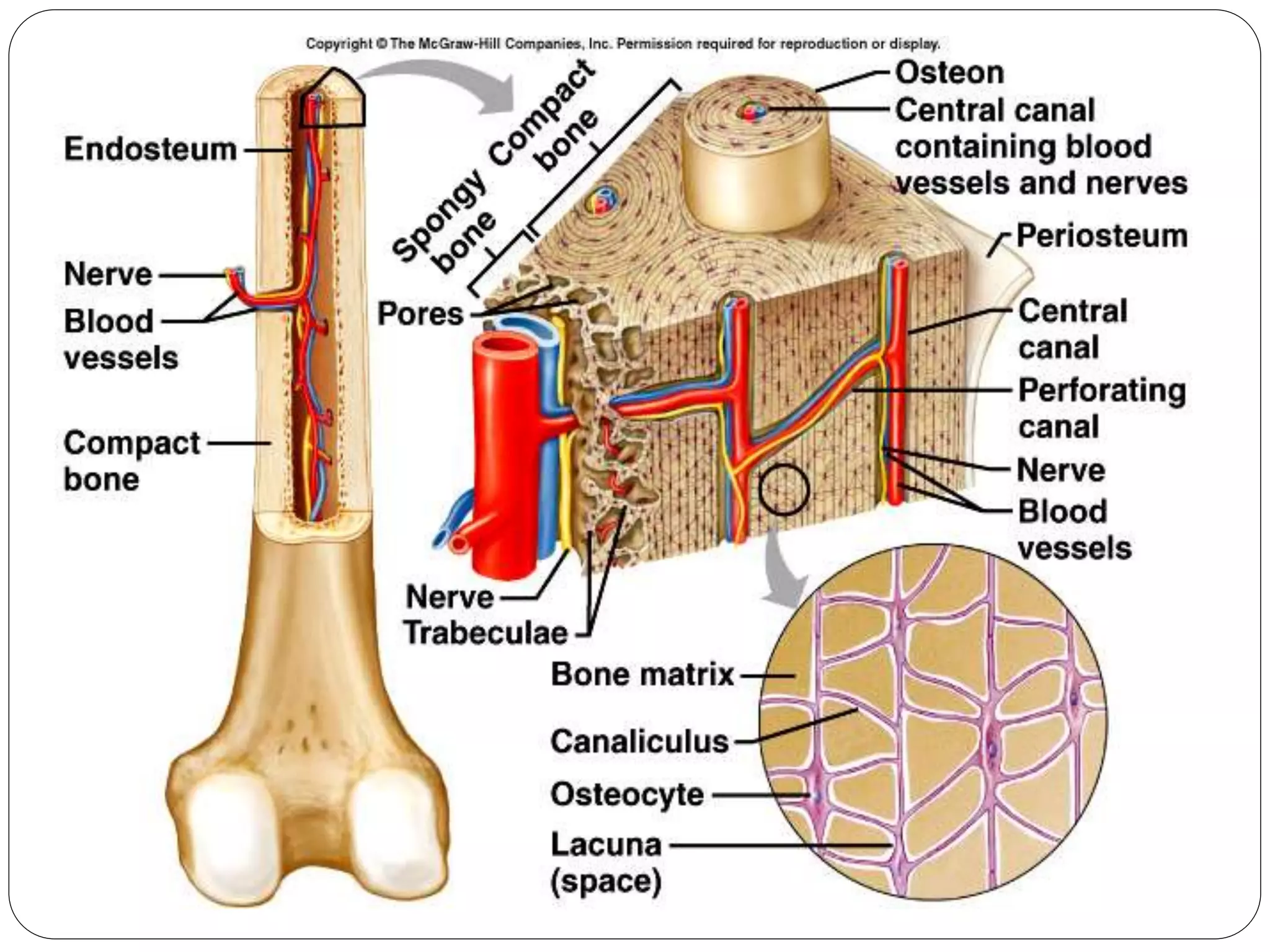
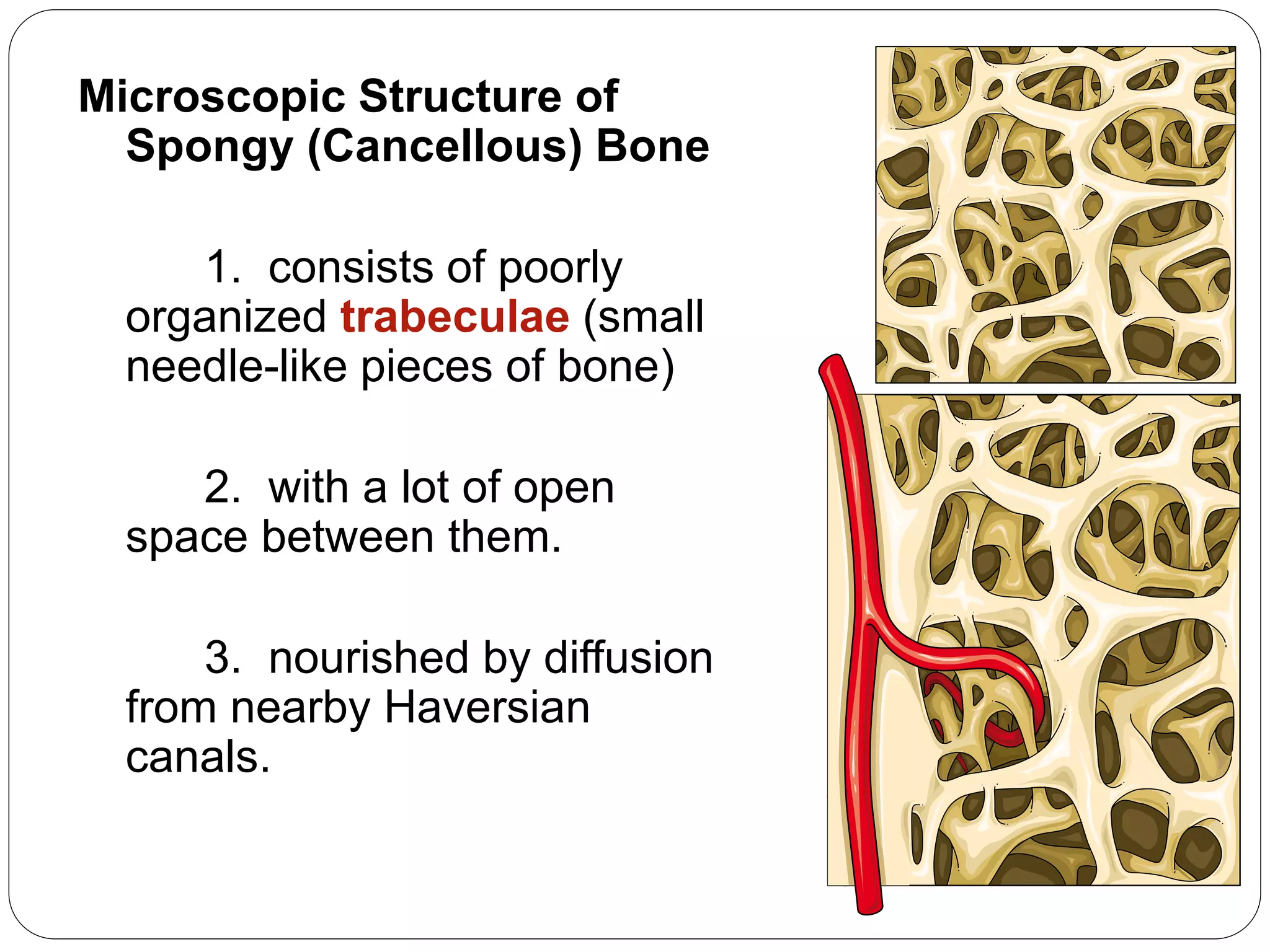
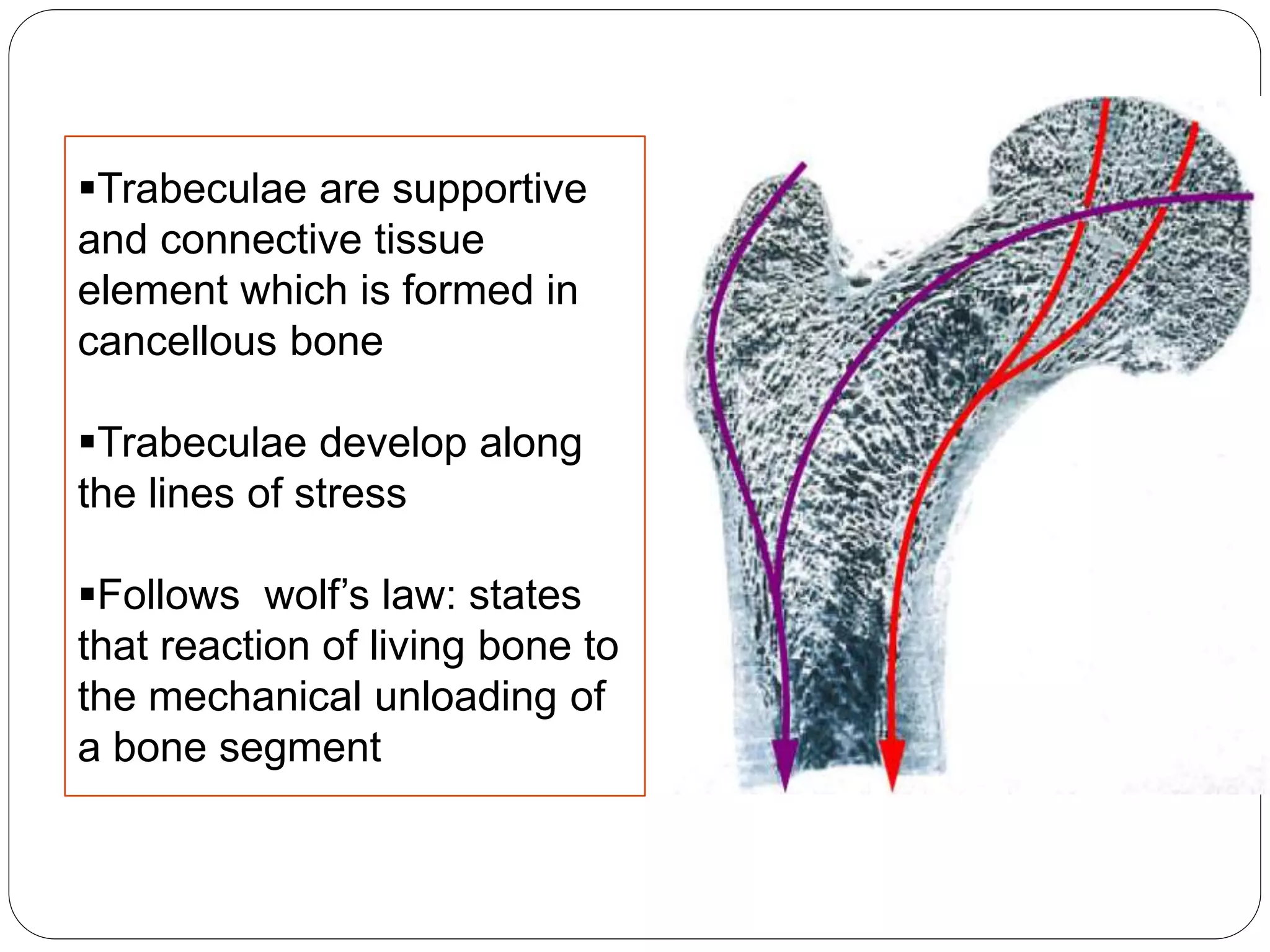
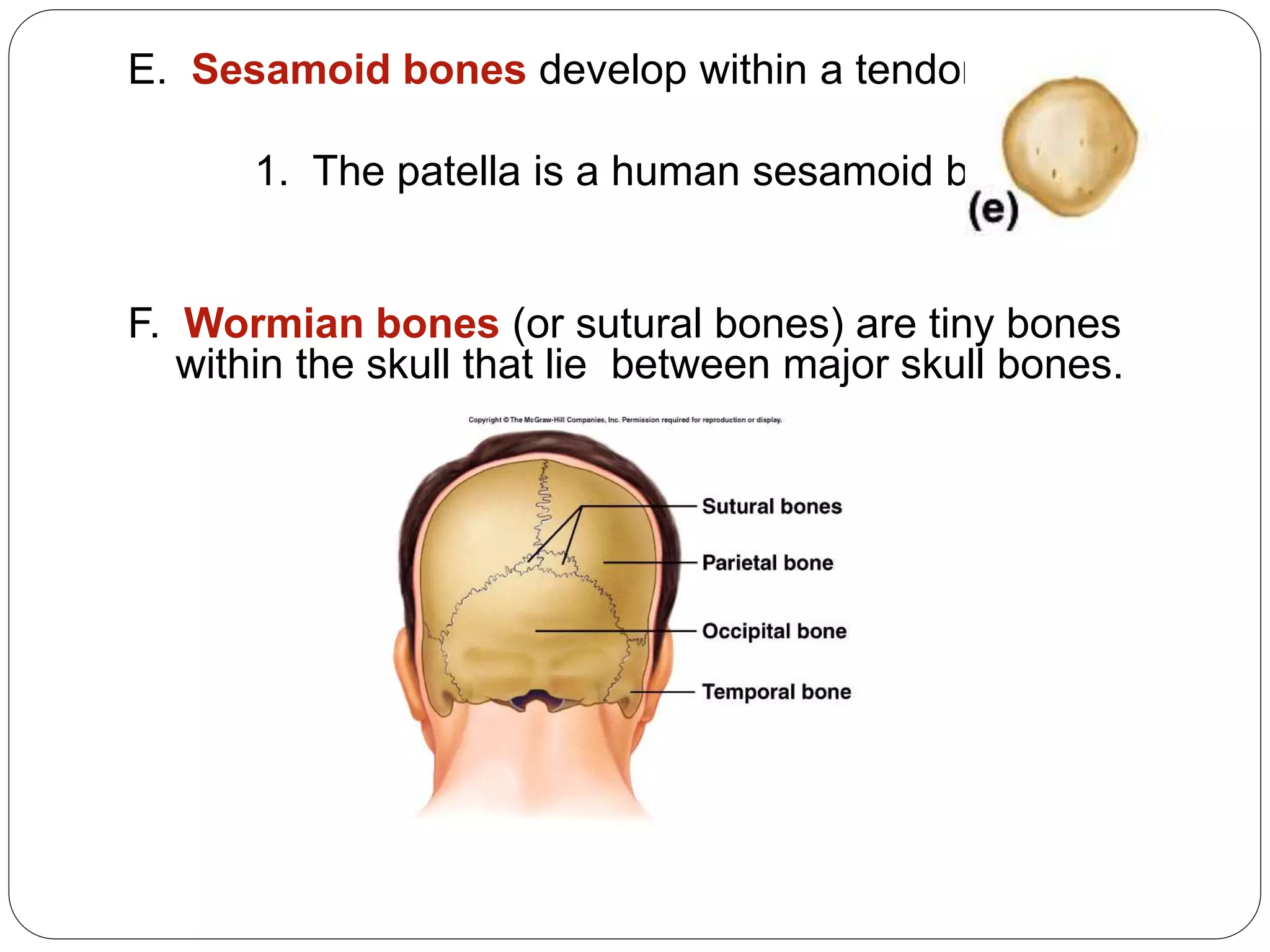
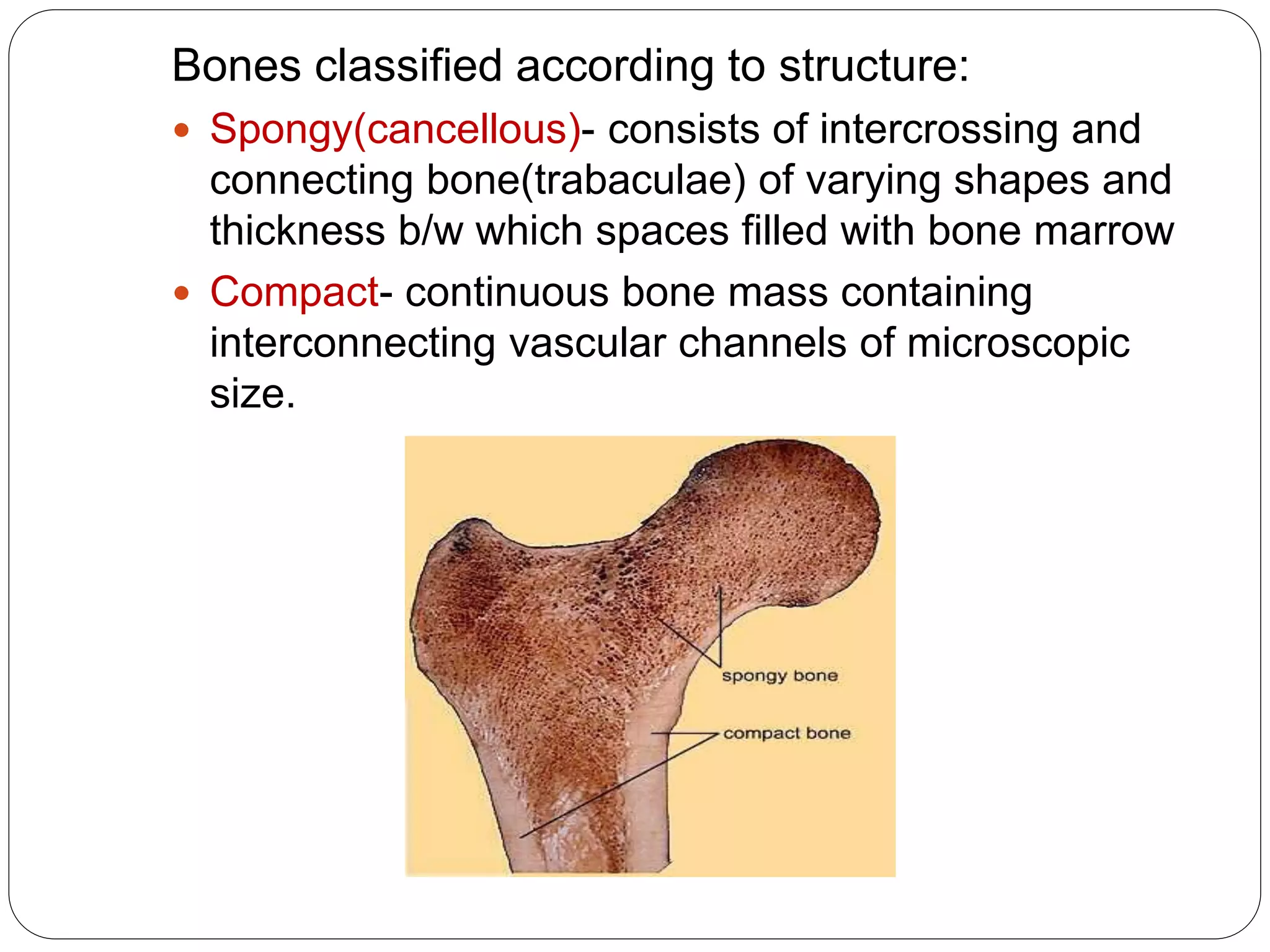
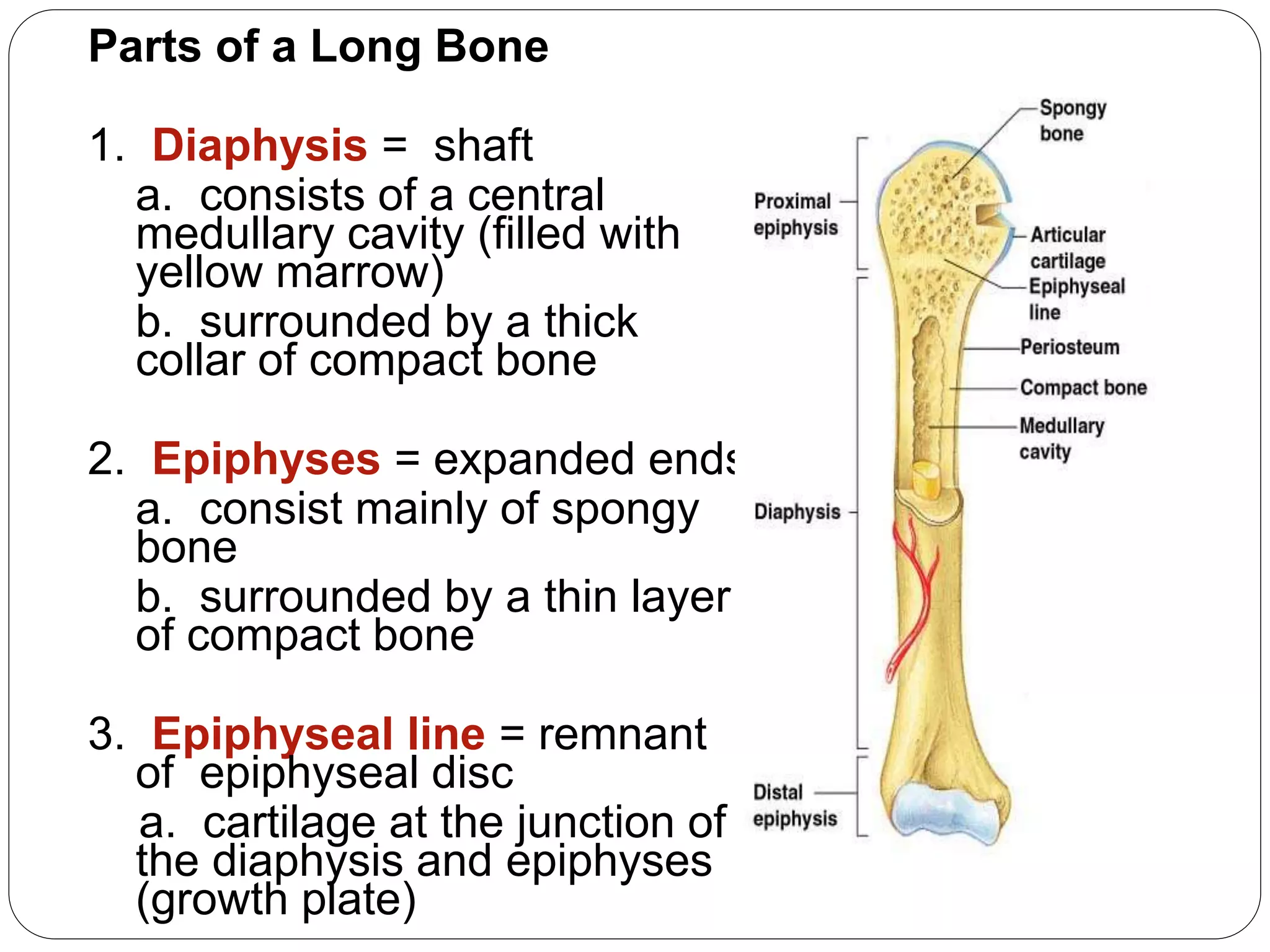
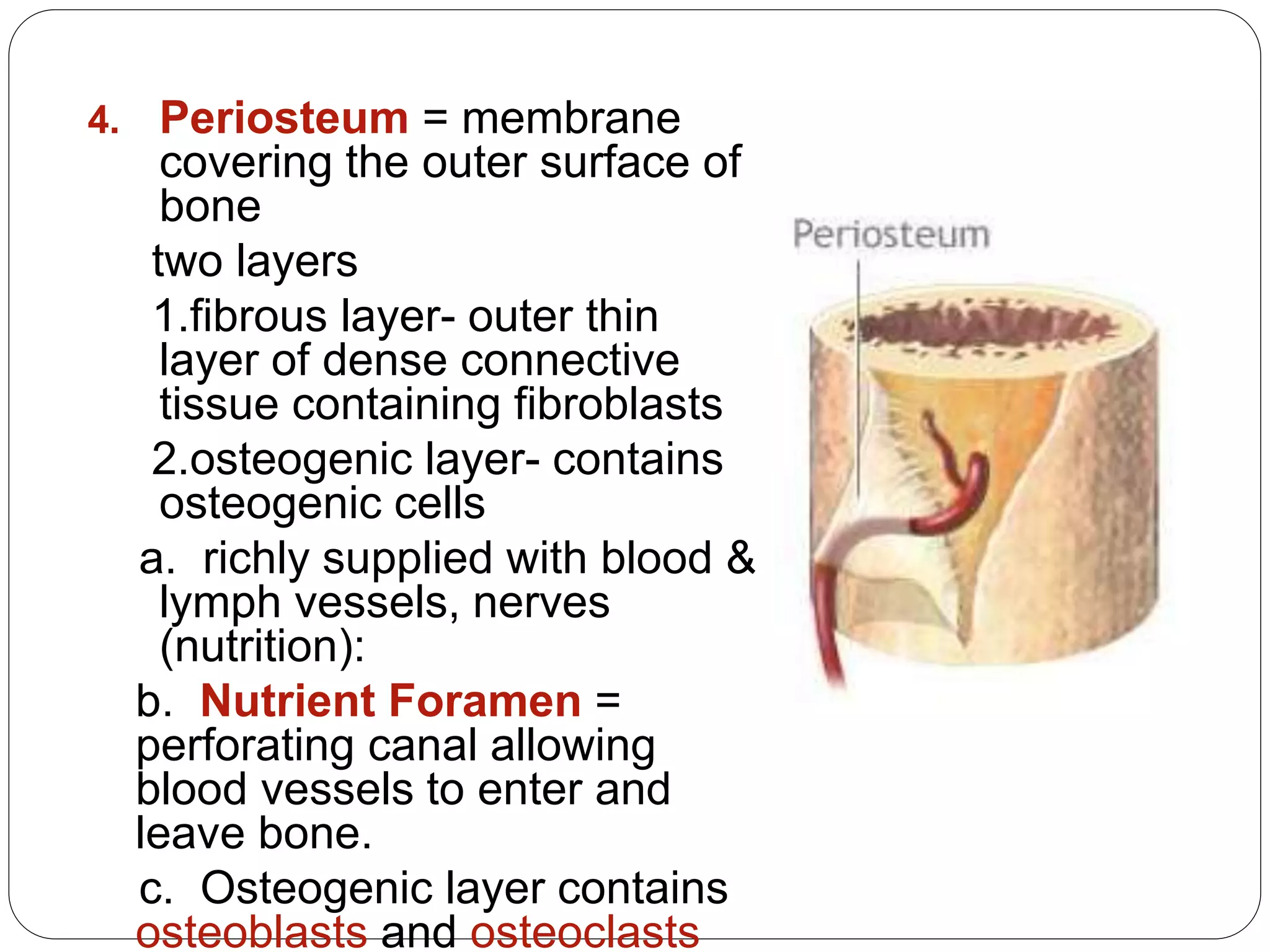
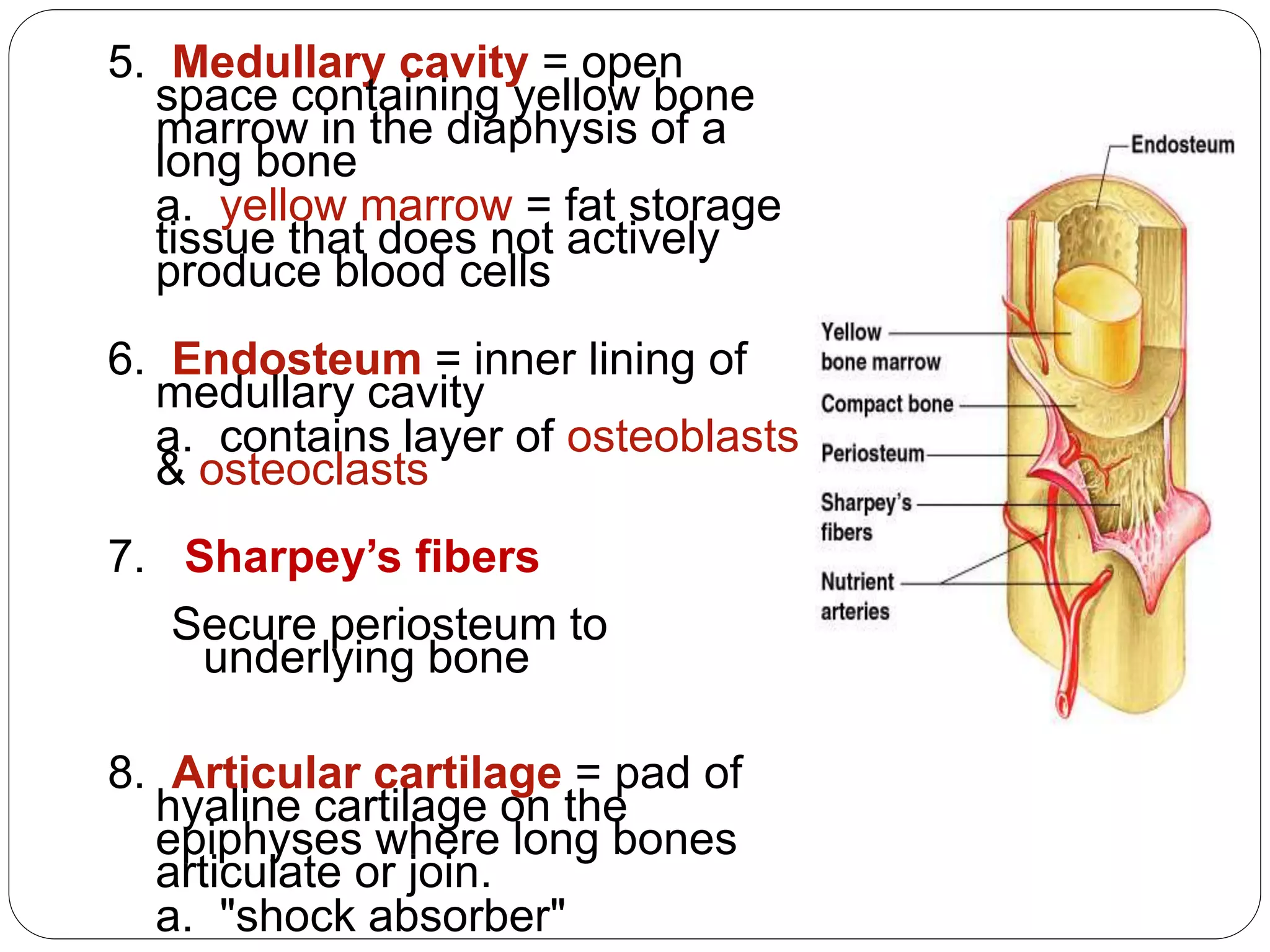
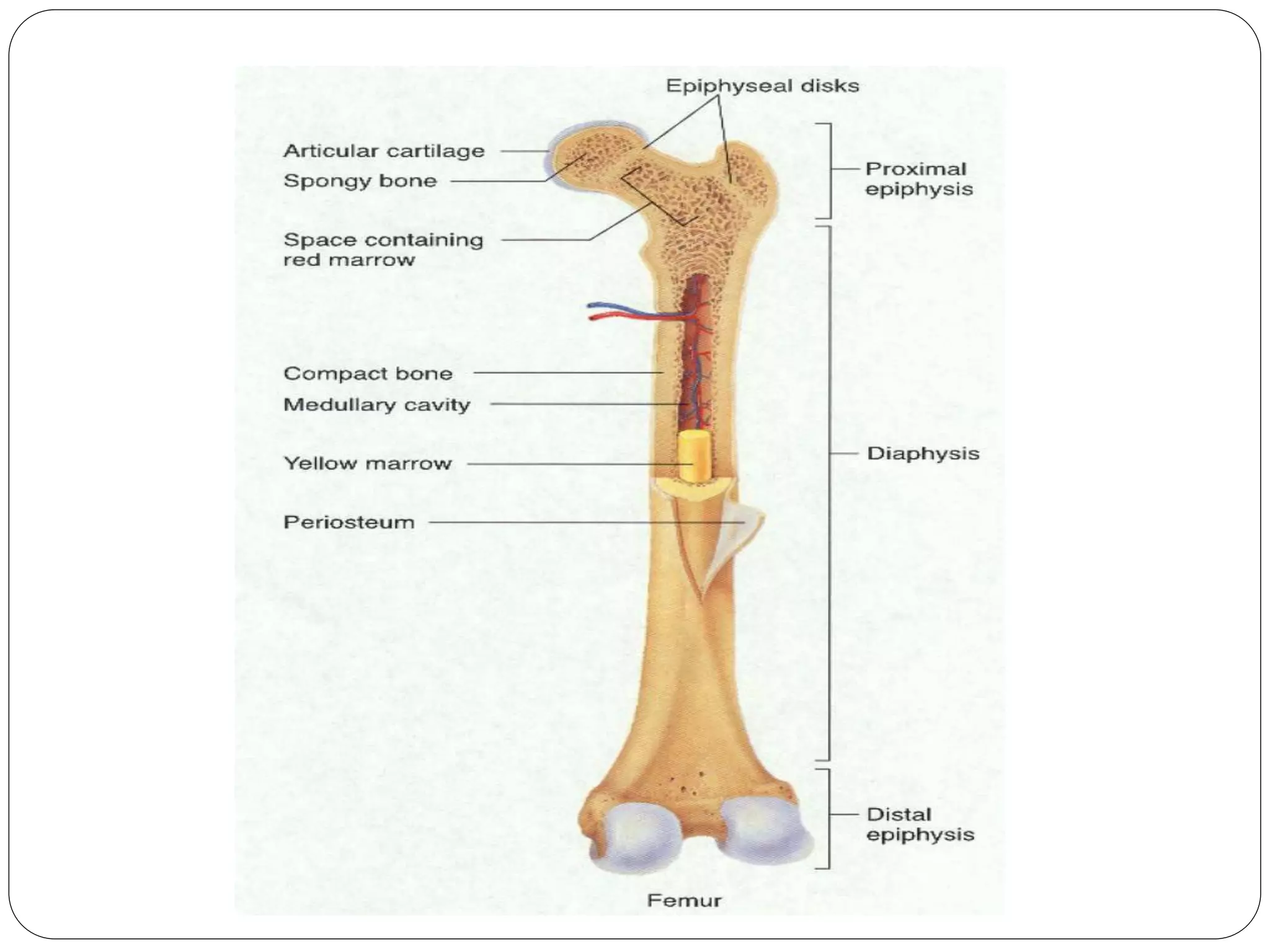
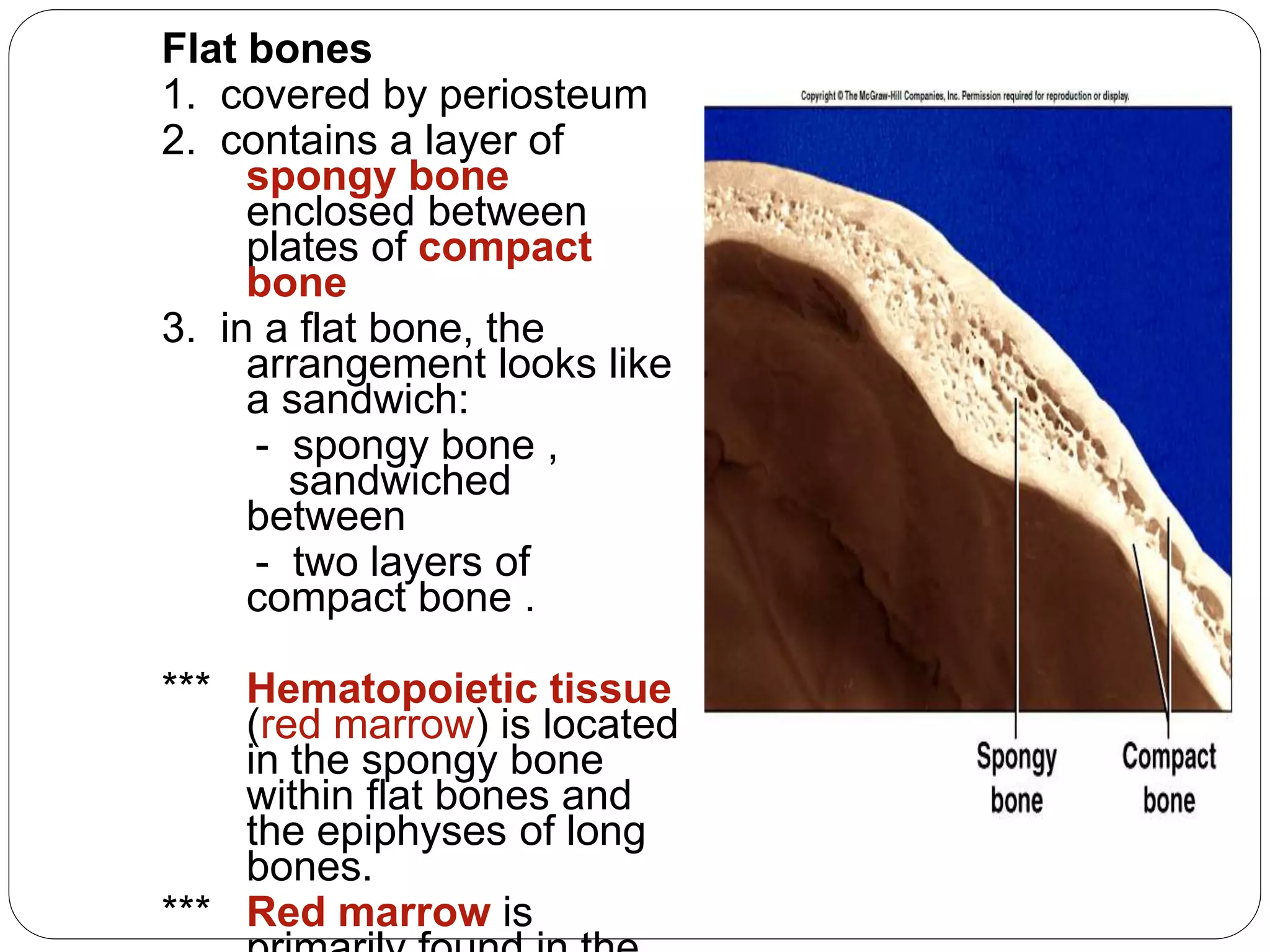
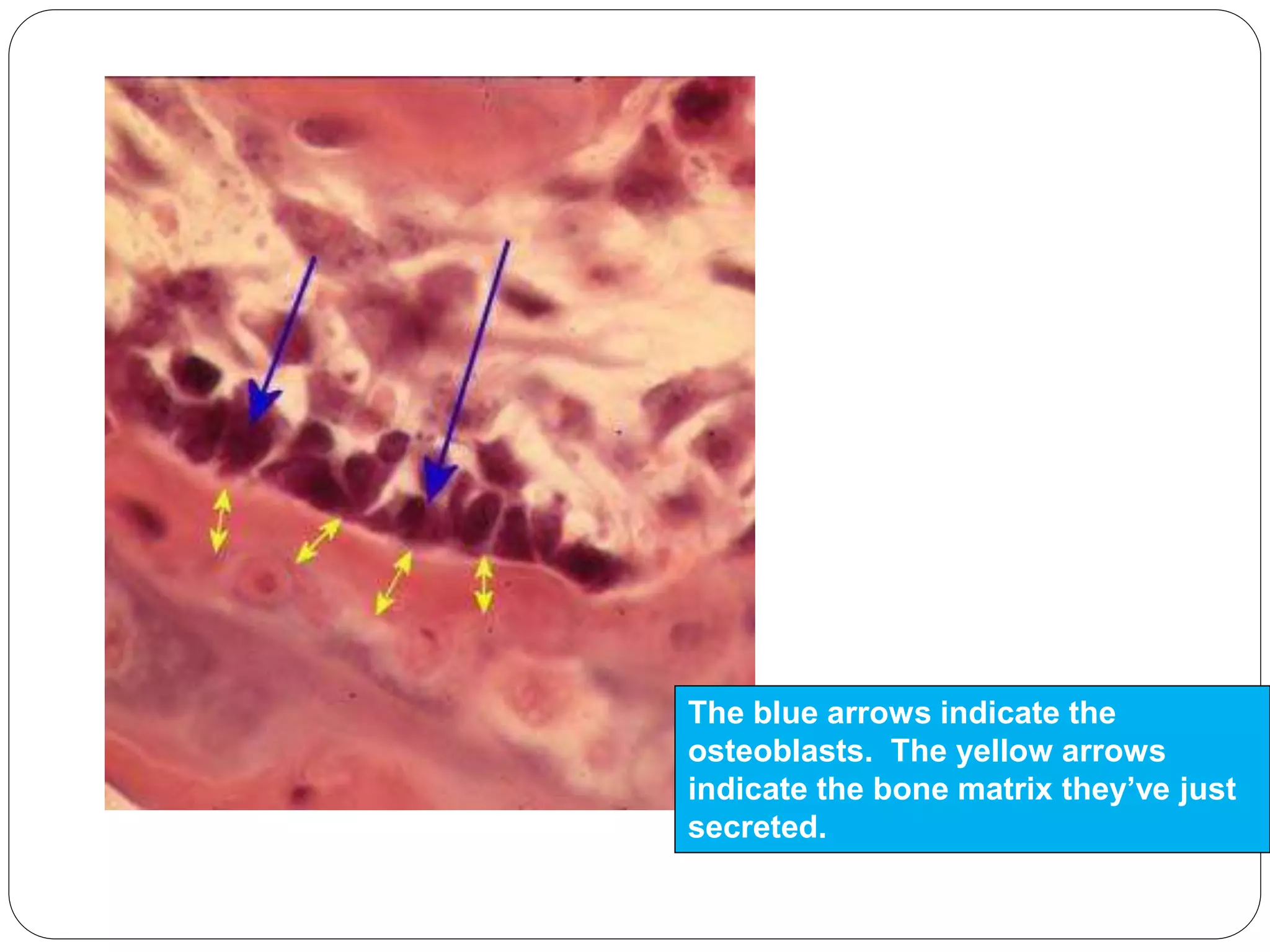
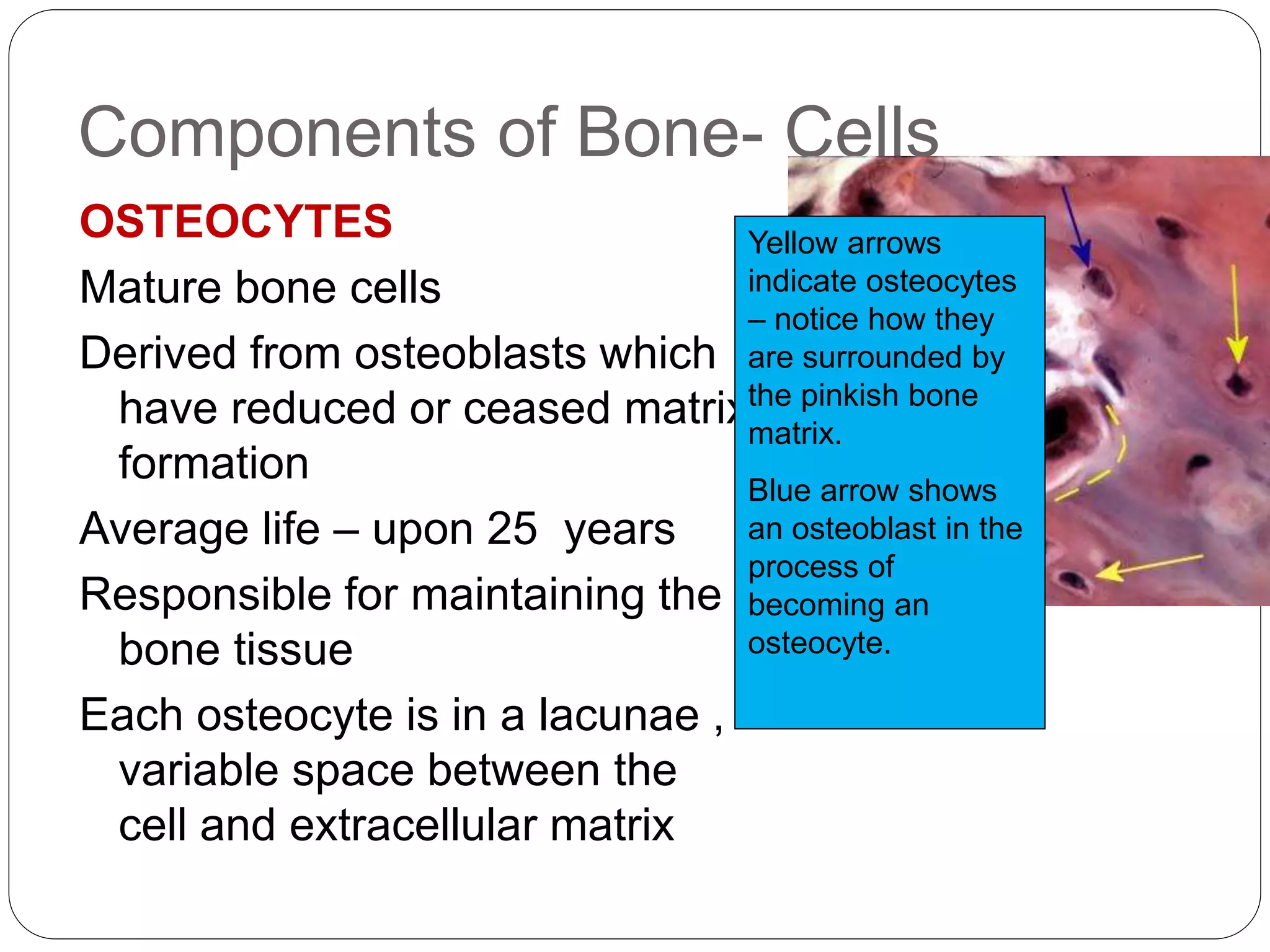
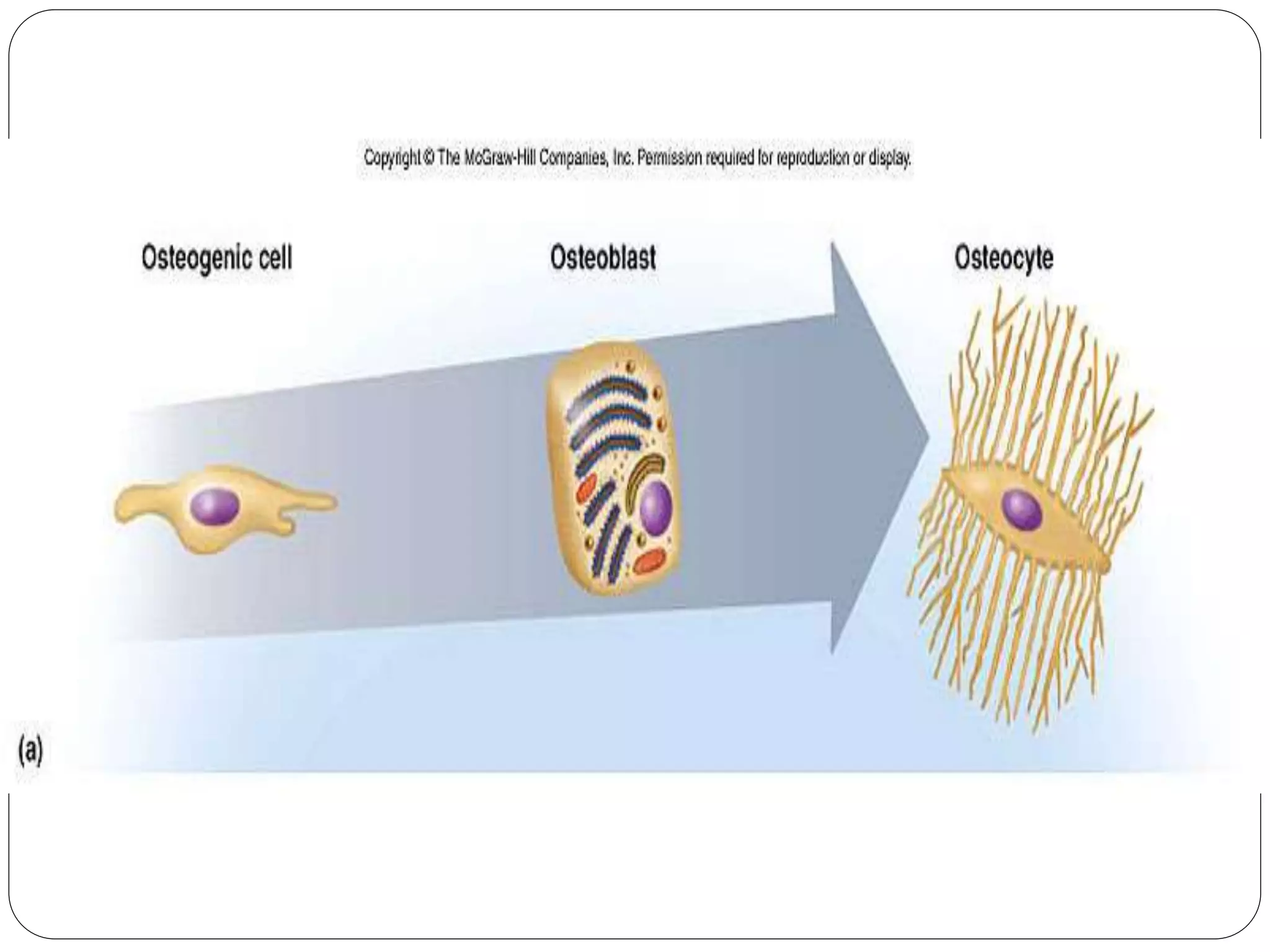
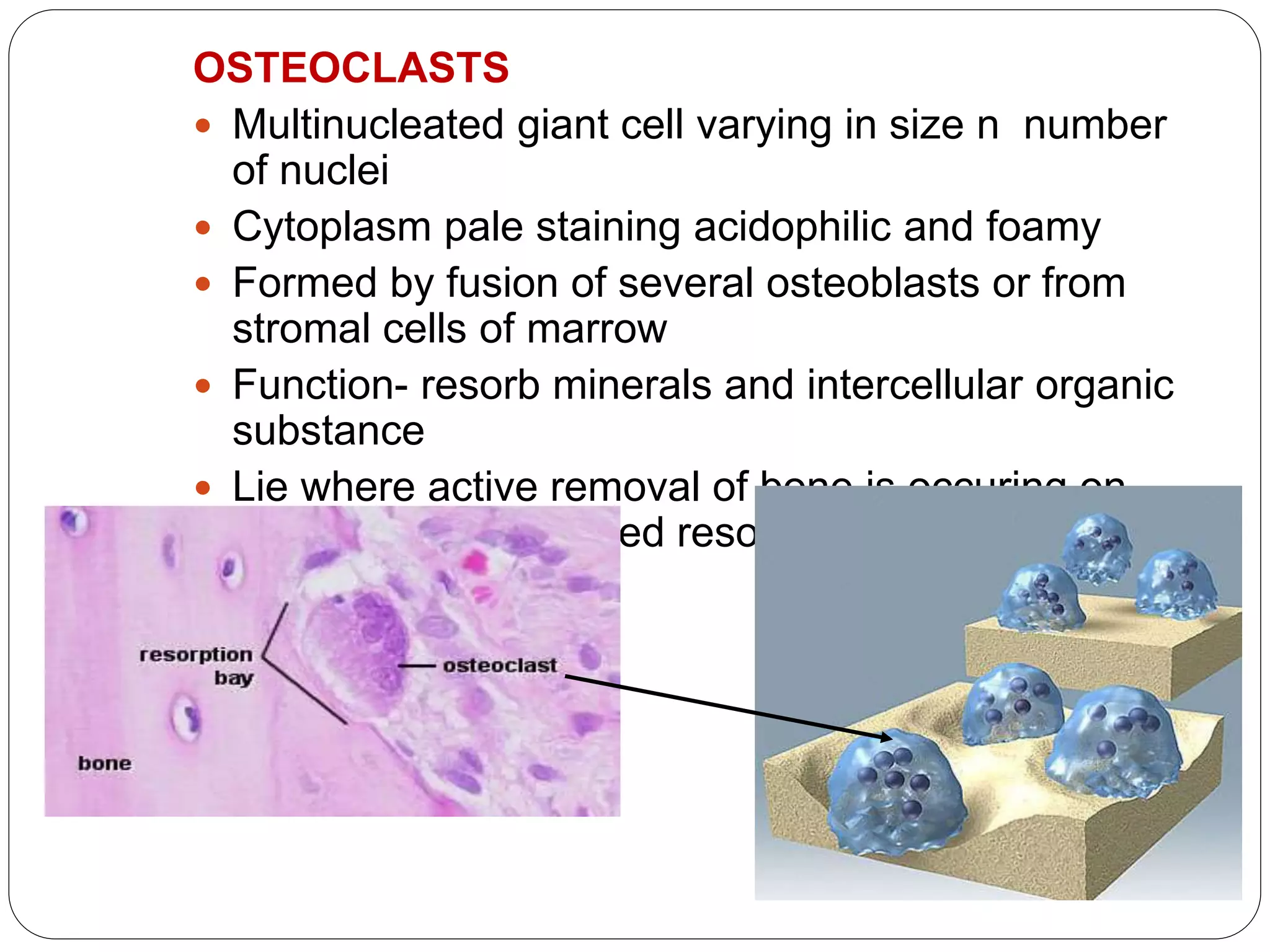
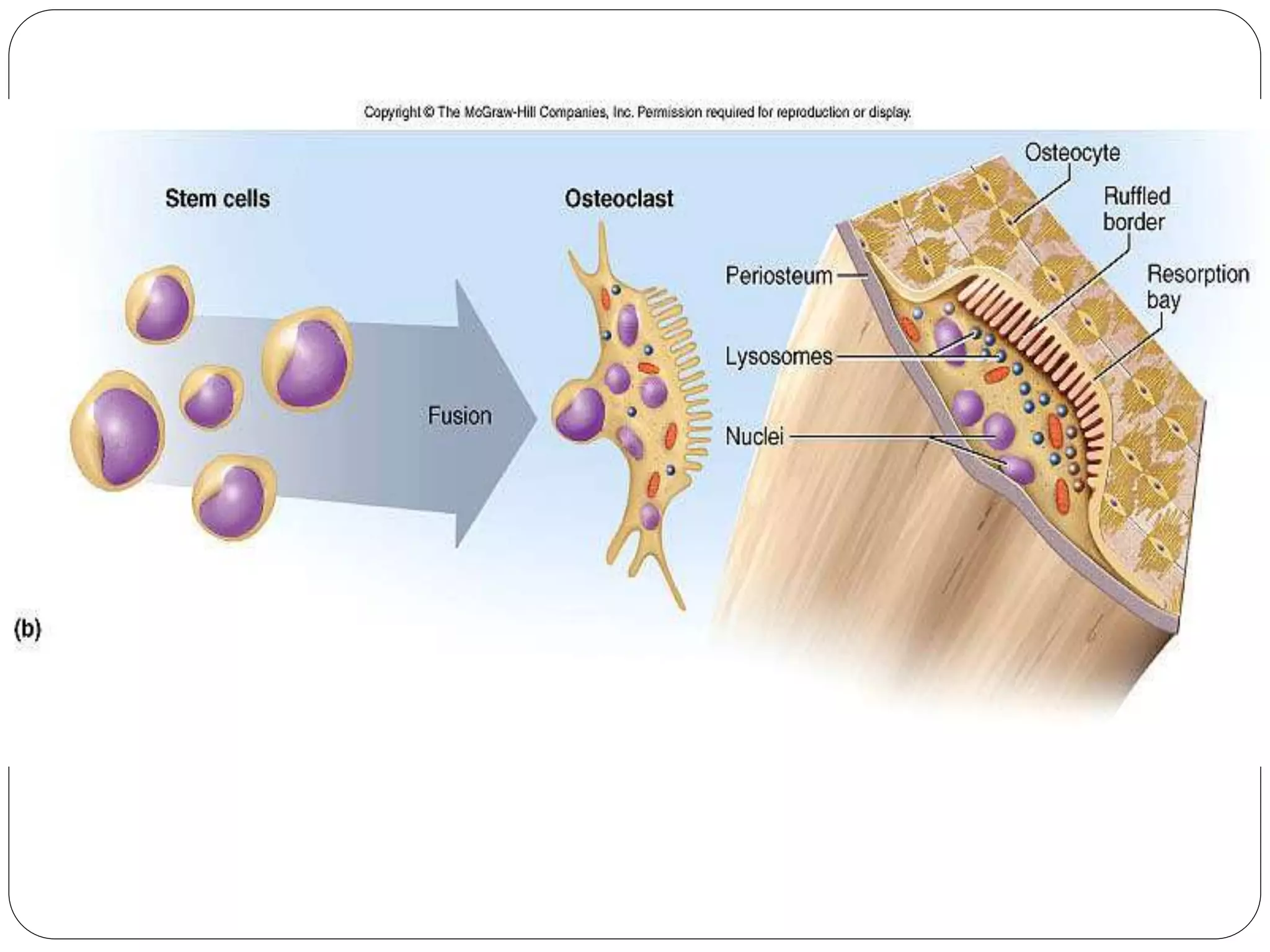
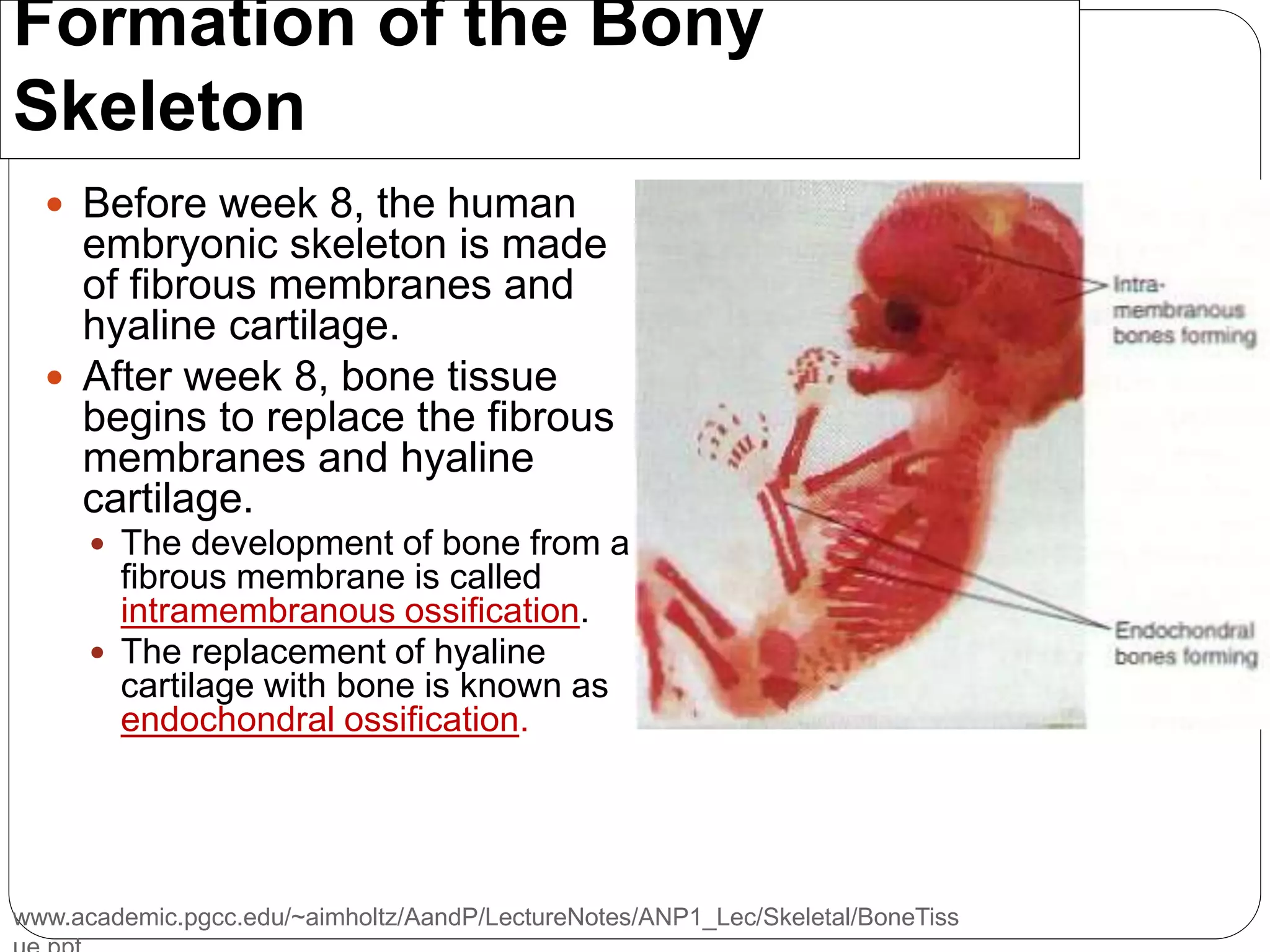
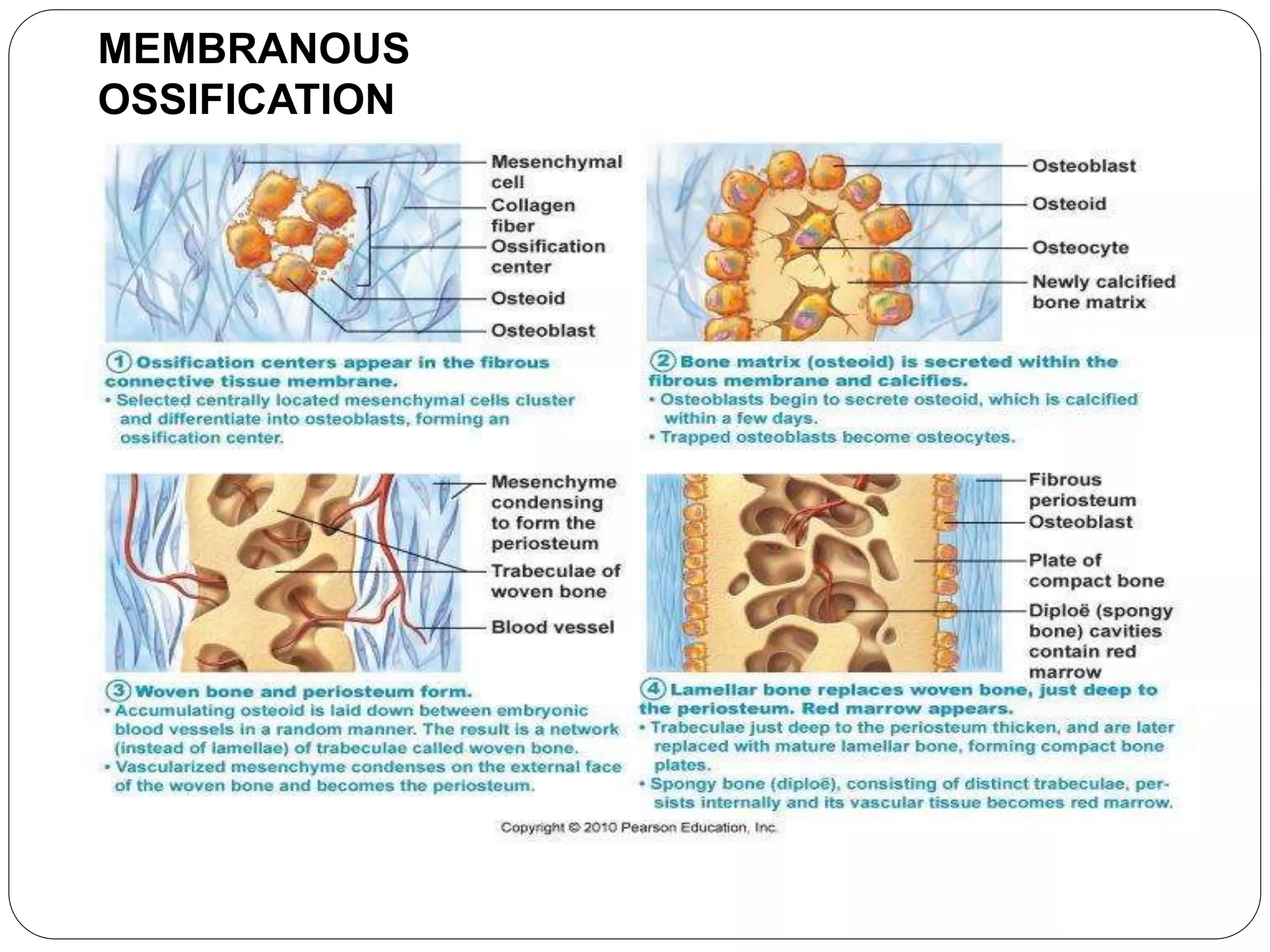
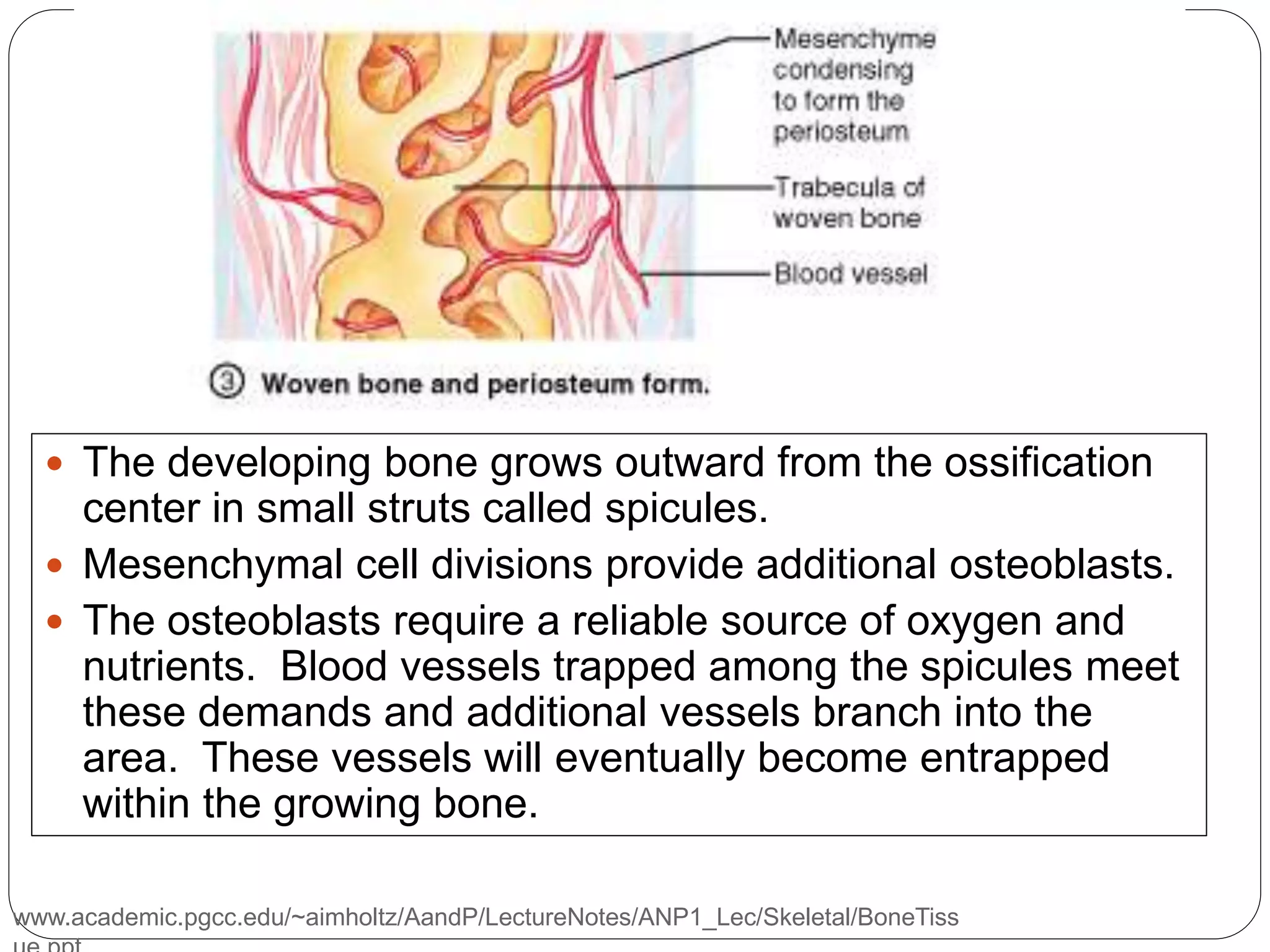
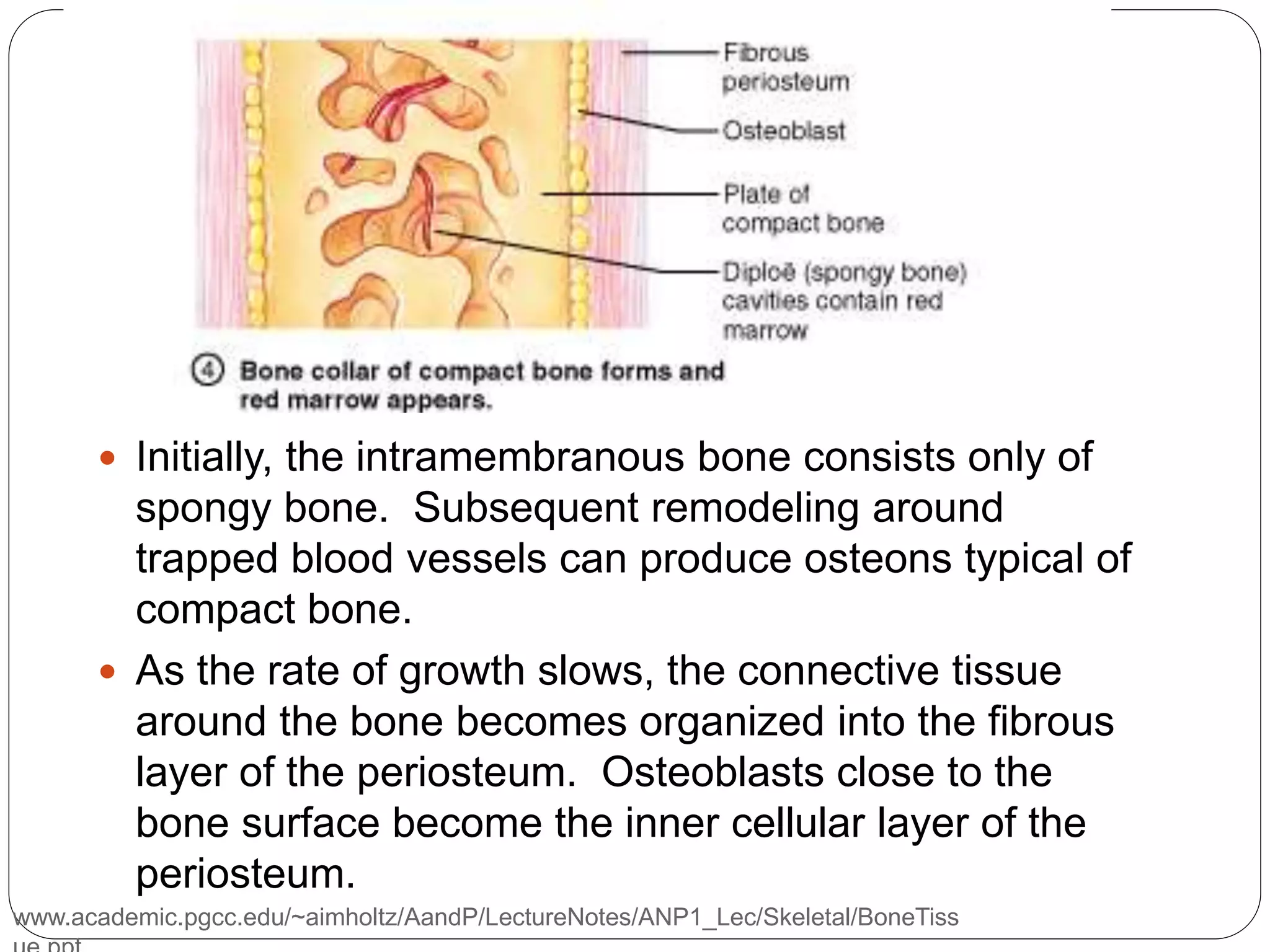
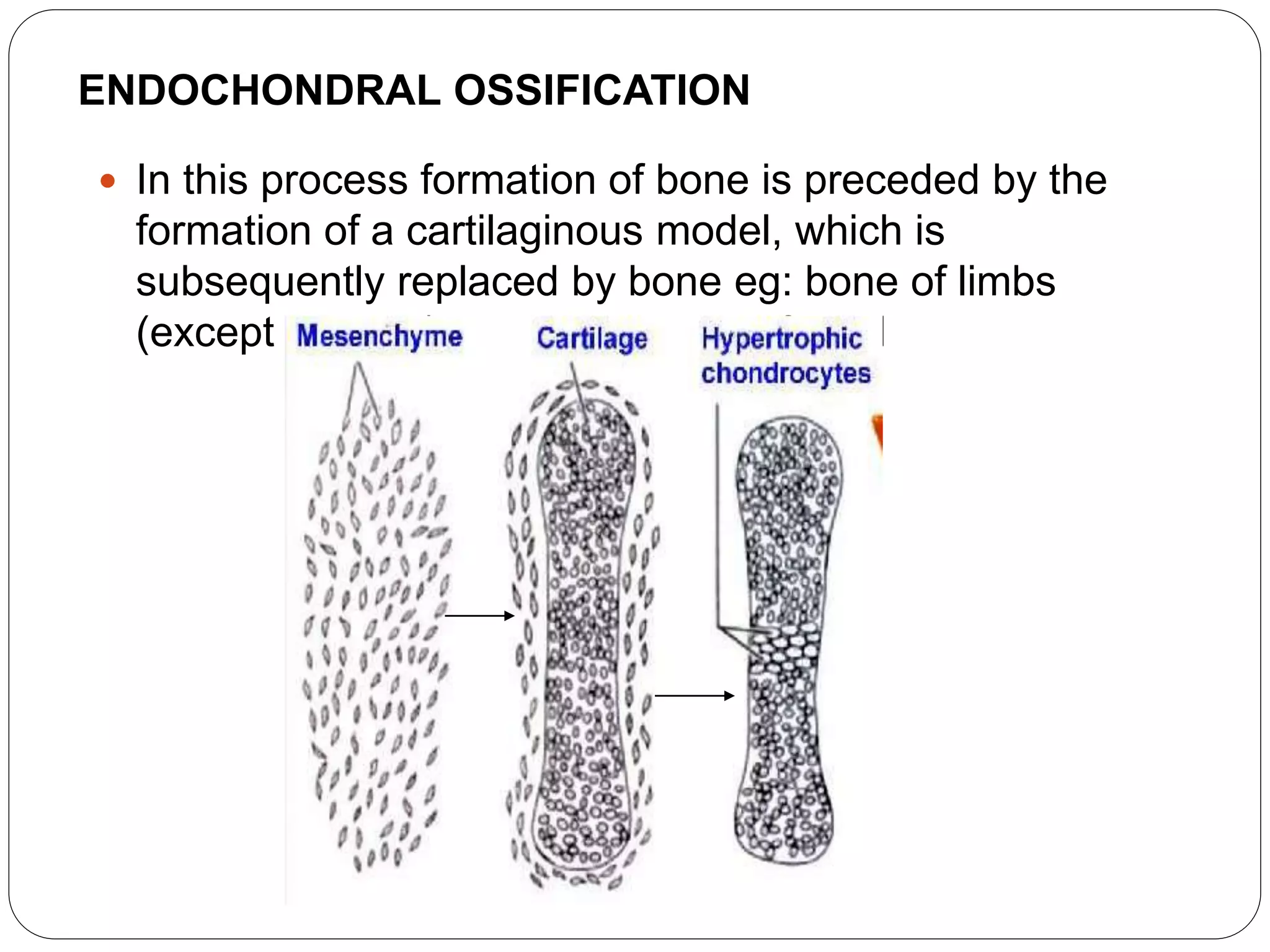
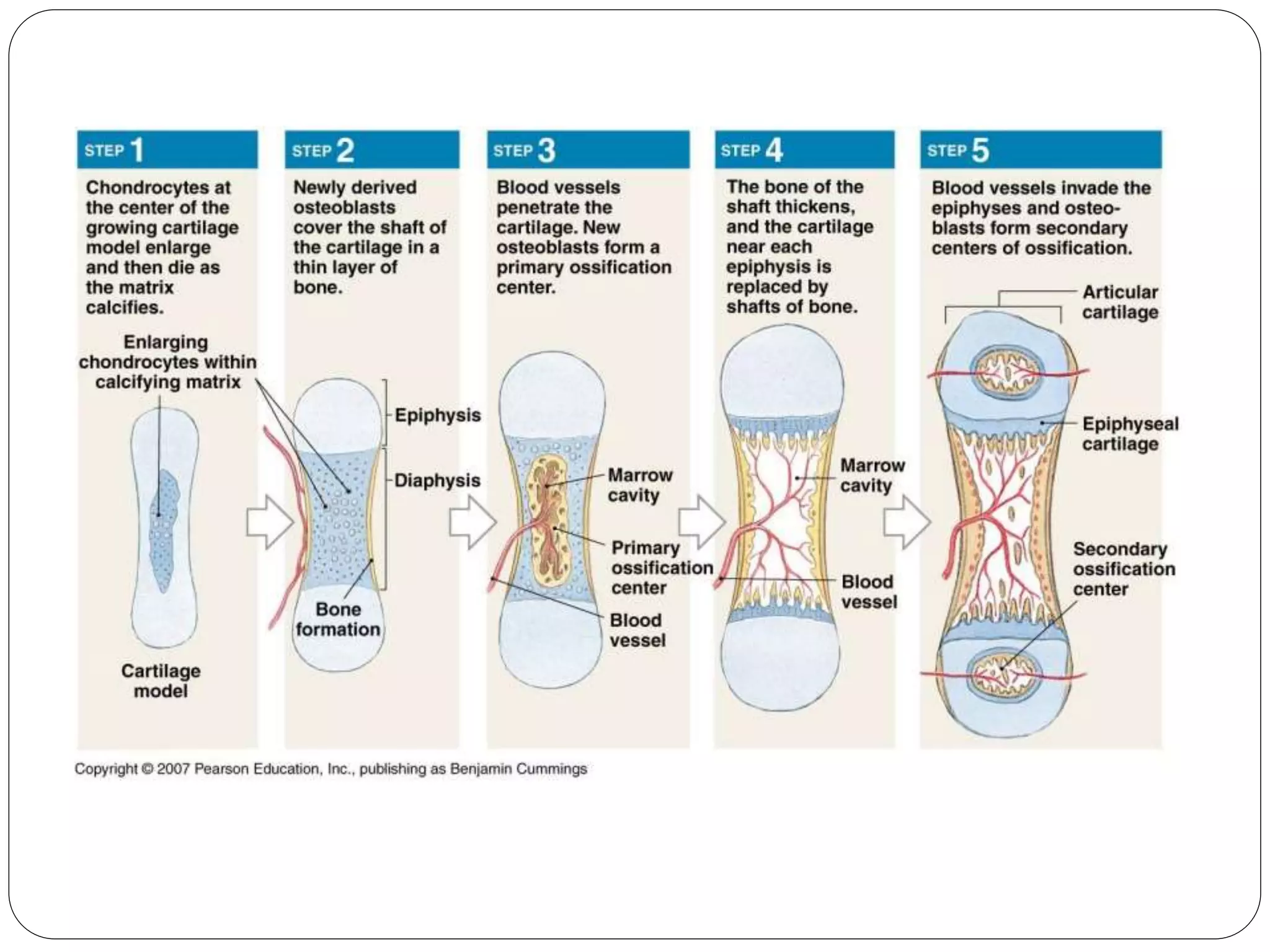
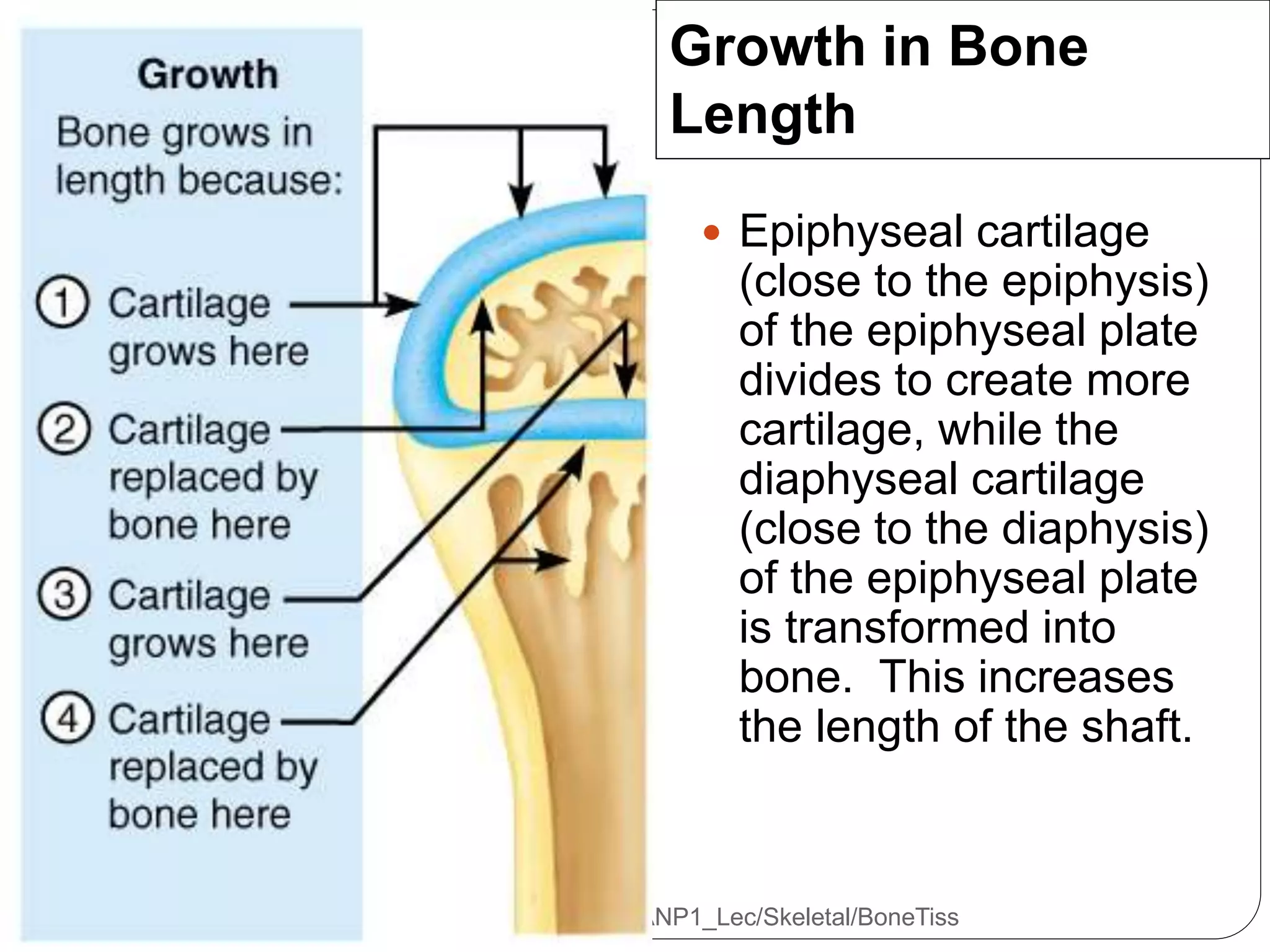
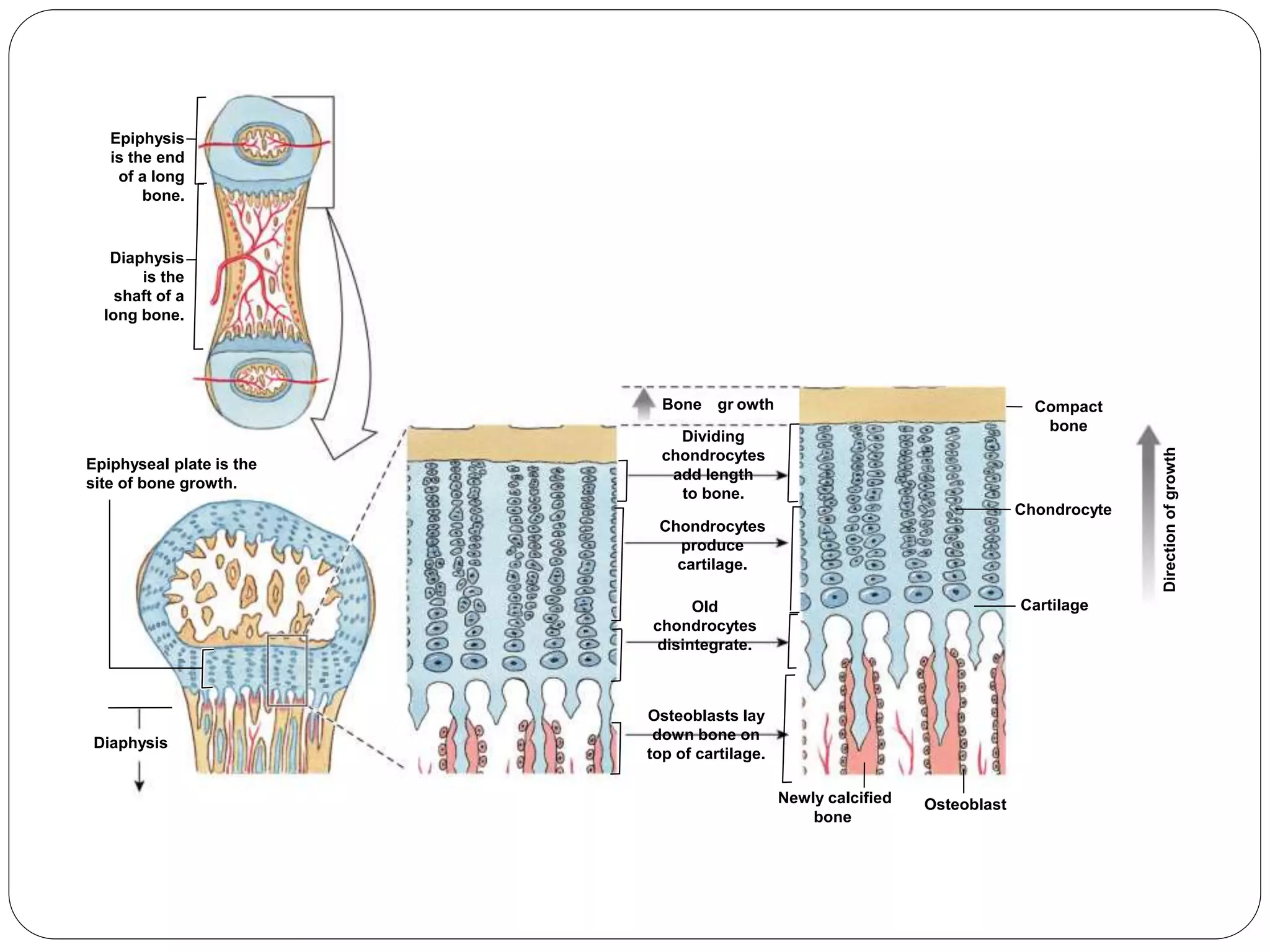
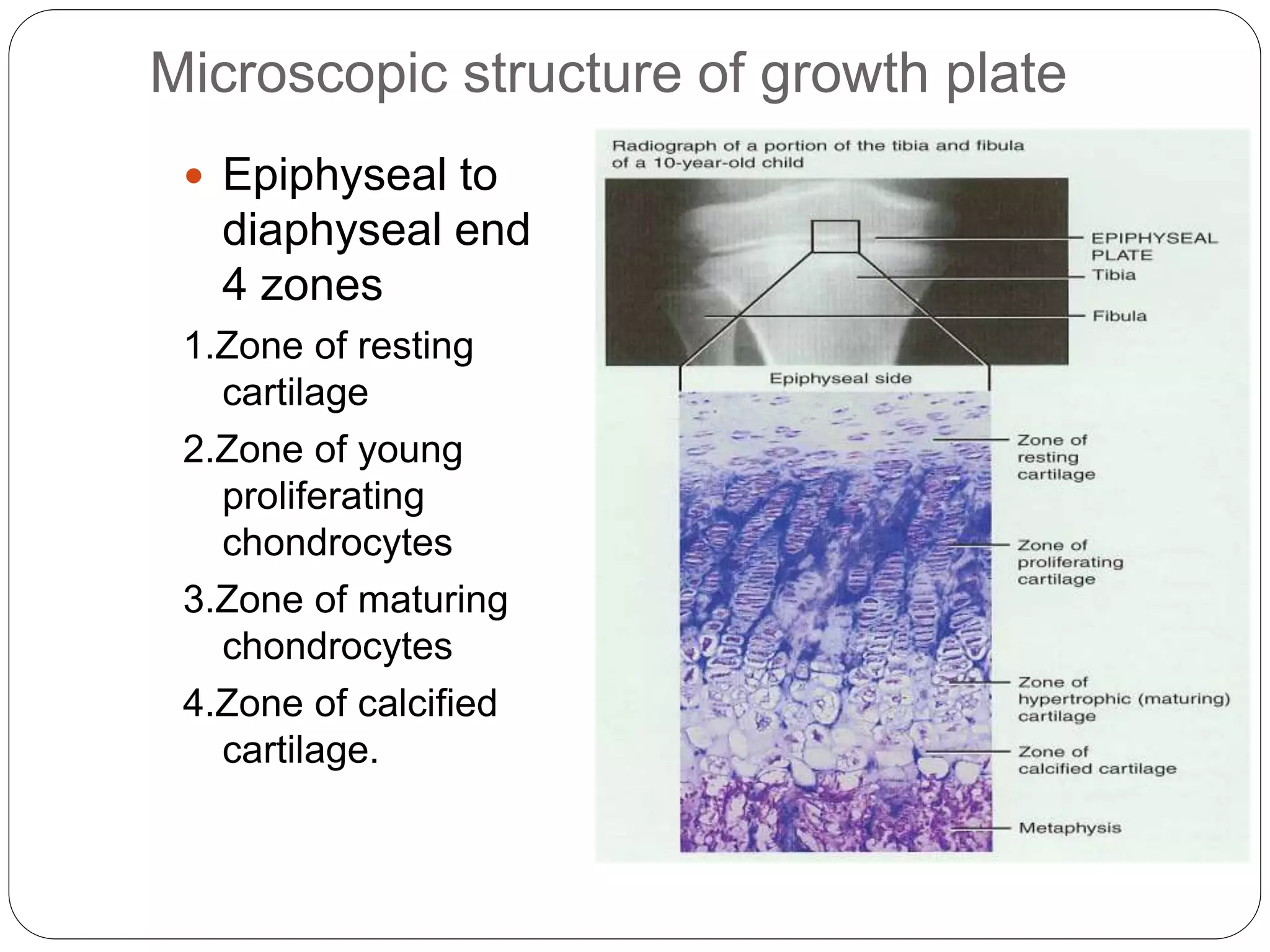
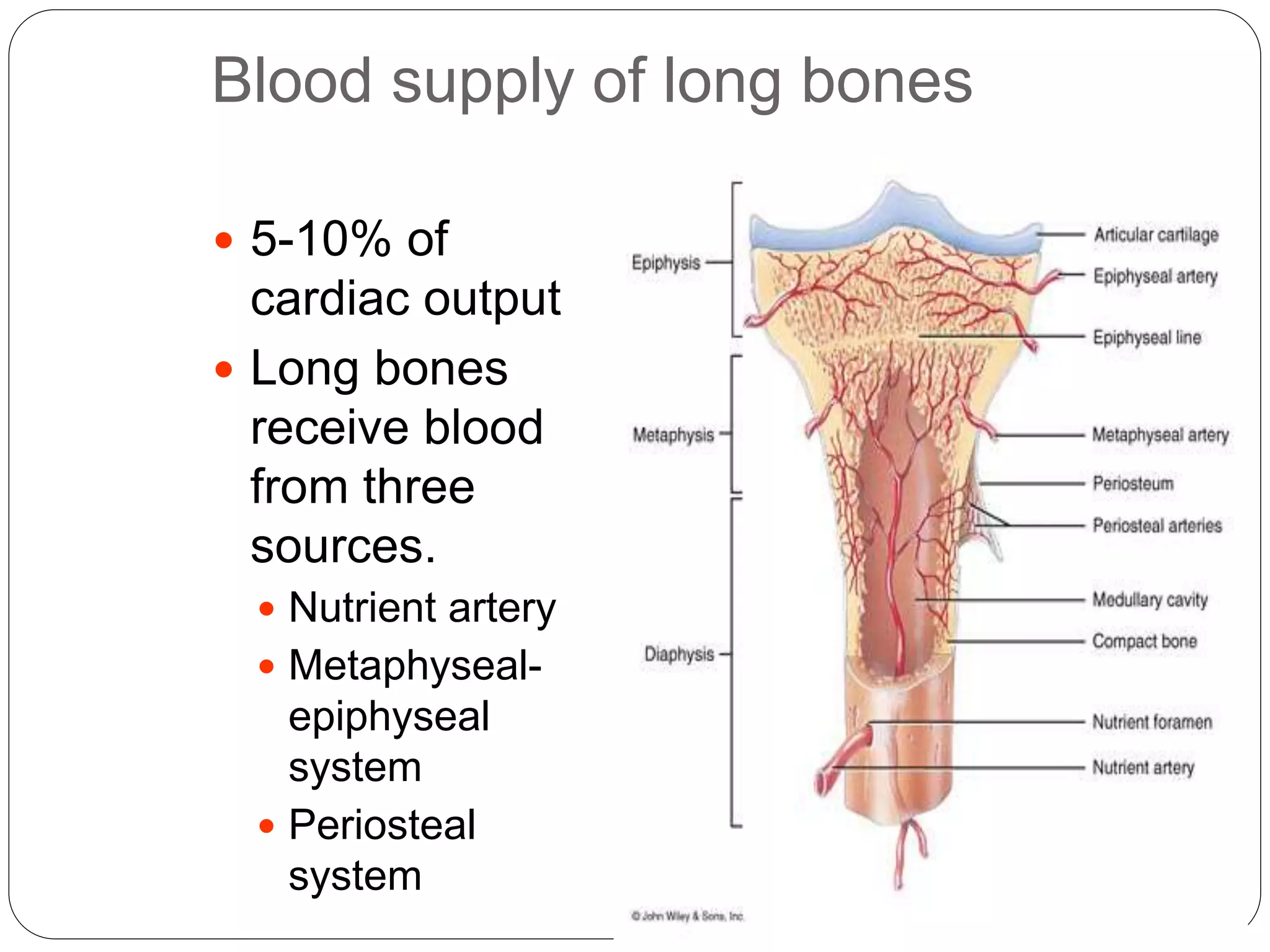
This document provides an overview of bone development, structure, and types. It discusses that bone is a mineralized connective tissue composed of cells and an intercellular matrix. There are two main types of bone tissue: compact bone, which makes up the hard outer surface and is made up of concentric lamellae; and spongy or cancellous bone, which is found in the interior and has a sponge-like appearance. Bone is also classified based on shape into long, short, flat, irregular, and sesamoid bones. The document outlines the development of bone through two processes: intramembranous ossification which forms flat bones; and endochondral ossification which replaces cartilage models with bone in