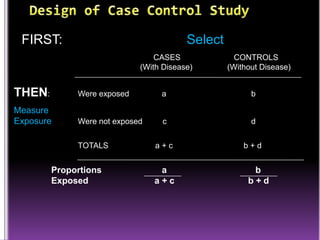
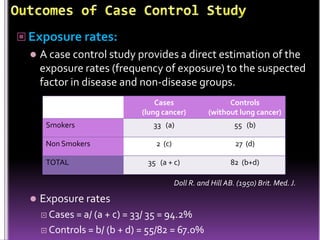
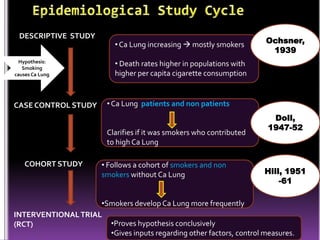
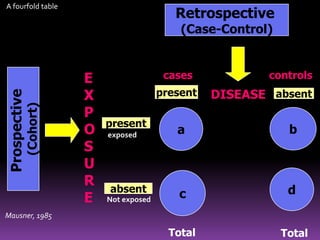
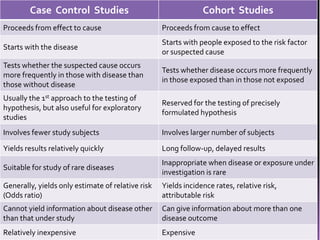
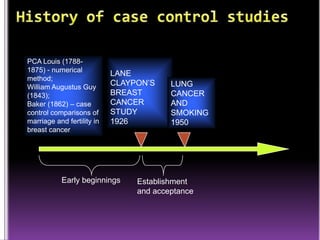
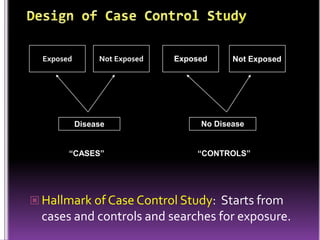
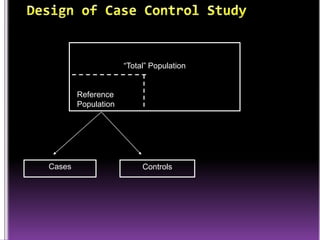
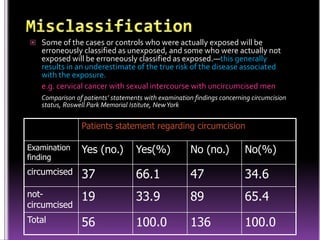
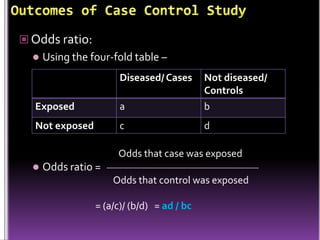
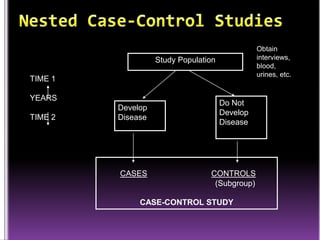
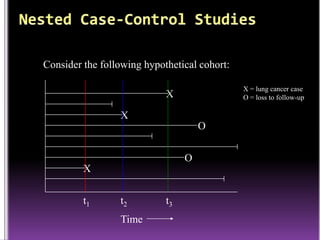
This document summarizes a seminar presentation on case control studies. It begins by defining epidemiological study cycles and analytical study types such as case control and cohort studies. It then focuses on case control studies, defining them, discussing their history, design, outcomes, limitations, advantages and applications. Examples of notable case control studies are provided, such as Lane Claypon's 1926 breast cancer study and studies from the 1950s linking smoking to lung cancer. Key aspects of case control study methodology like selection of cases and controls, and matching to control for confounding variables are explained.