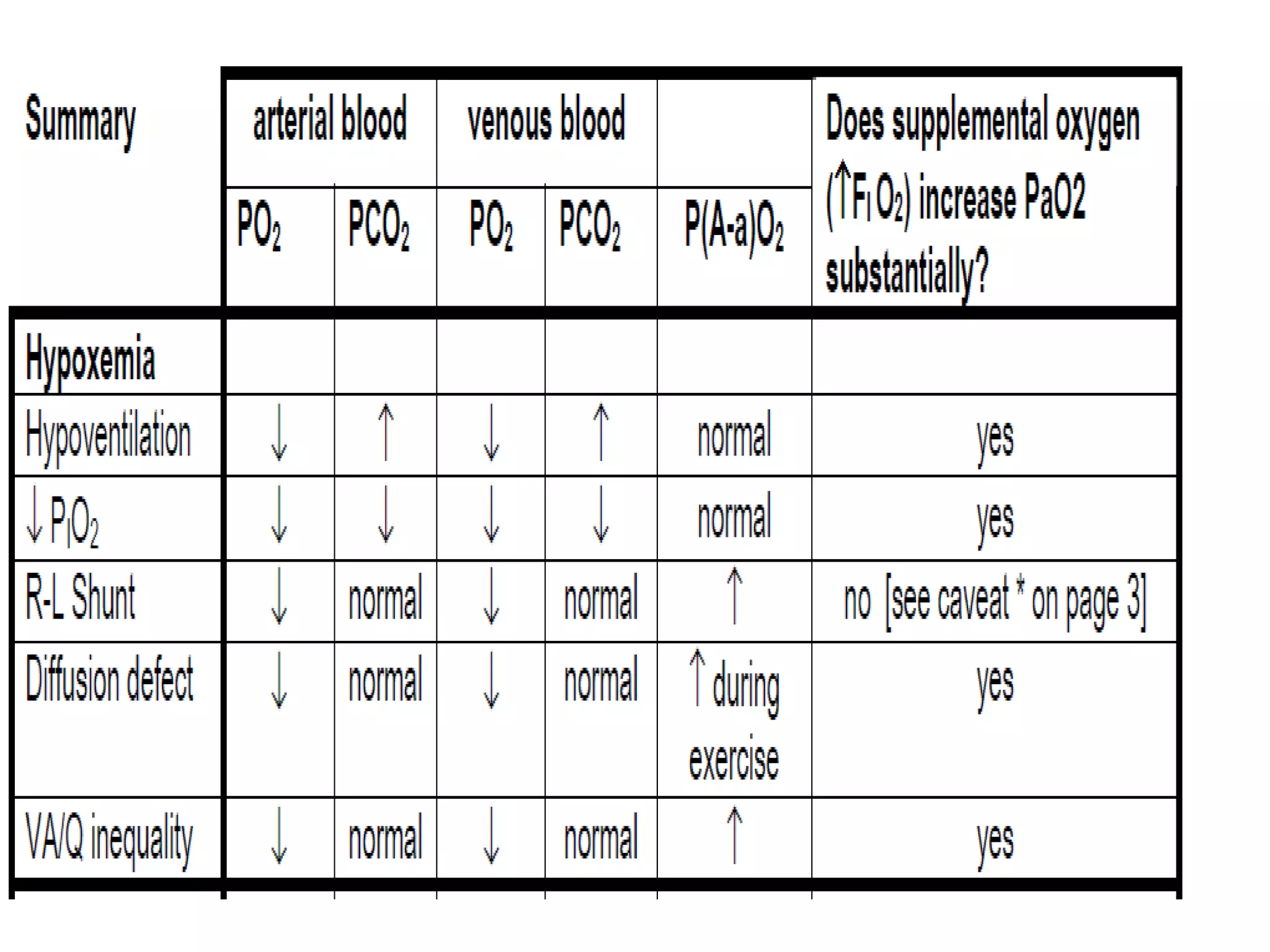
1. Hypoxemia, defined as low oxygen levels in arterial blood, can be caused by hypoventilation, low inspired oxygen, right-to-left shunts, ventilation-perfusion mismatching, or diffusion impairment in the lungs.
2. Physical exam and arterial blood gas analysis are used to diagnose hypoxemia and its underlying causes. Treatment focuses on oxygen supplementation, treating the underlying condition, correcting acid-base imbalances, and mechanical ventilation if needed.
3. The causes, mechanisms, diagnosis and management of hypoxemia are complex but critical for treatment of respiratory failure.








![LOW INSPIRED OXYGEN [ PI O2 ]
• Examples-
• A decrease in barometric pressure [e.g. breathing at high
altitude].
• A decrease in FIO2 – accidental [e.g. anesthetist does not
supply enough oxygen or improper installation of oxygen
supply lines or a leak in the breathing circuit].
• P(A-a)O2 normal
• PaCO2 is decreased. This reduction in PaCO2 (hypocapnia) is
due to hyperventilation in response to hypoxemia.
• Peripheral chemoreceptors sense the low arterial PO2 and
initiate an increase in ventilation through their input to the
medullary respiratory centre](https://image.slidesharecdn.com/approachtohypoxemia-160308182108/75/Approach-to-hypoxemia-11-2048.jpg)


![RIGHT TO LEFT SHUNT
• Congenital abnormalities
• i) intra-cardiac shunt [e.g. Tetralogy of Fallot: ventricular
septal defect + pulmonary artery stenosis]
• ii) intra-pulmonary fistulas [direct communication between a
branch of the pulmonary artery and a pulmonary vein].](https://image.slidesharecdn.com/approachtohypoxemia-160308182108/75/Approach-to-hypoxemia-14-2048.jpg)
![RIGHT TO LEFT SHUNT
• Physiologic shunt: In disease states, a portion of the
cardiac output goes through the regular pulmonary vasculature
but
does not come into contact with alveolar air due to filling of
the alveolar spaces with fluid [e.g. pneumonia, drowning,
pulmonary edema]
• An important diagnostic feature of a shunt is that the arterial
PO2 does not rise to the normal level when the patient is given
100% oxygen to breathe.](https://image.slidesharecdn.com/approachtohypoxemia-160308182108/75/Approach-to-hypoxemia-15-2048.jpg)