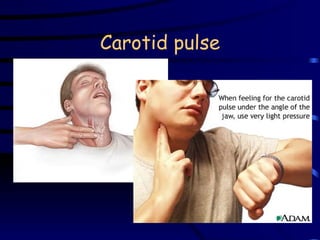
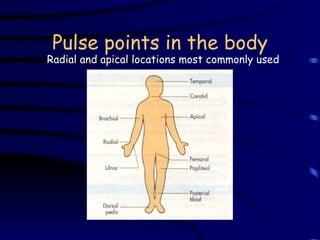
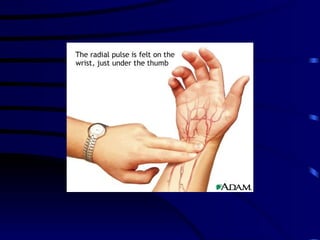
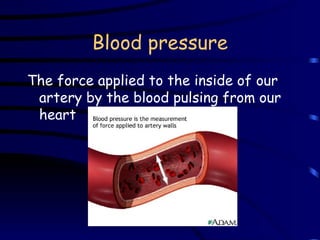
Vital signs provide important health information. The most common vital signs measured are temperature, pulse, blood pressure, and respiration. Alterations in vital signs can indicate a need for further intervention. Personal care workers are responsible for accurately recording clients' vital signs according to workplace protocols and reporting any abnormalities to supervisors or medical professionals.