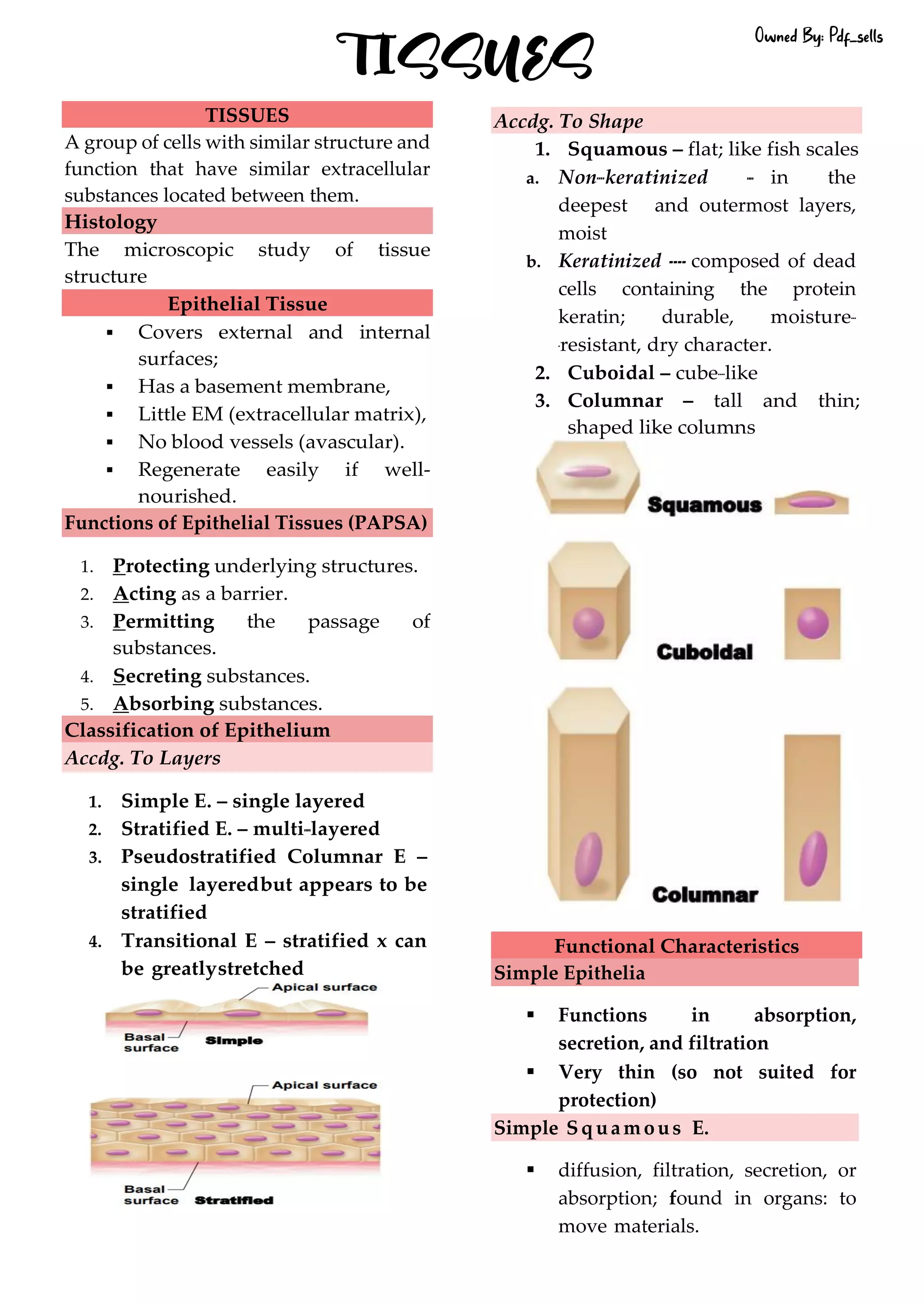
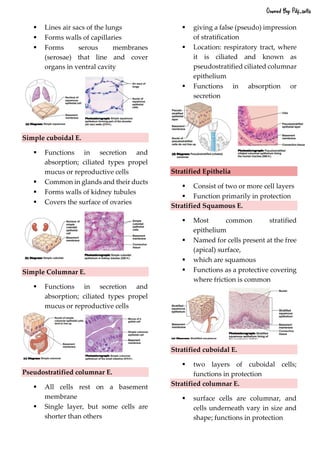
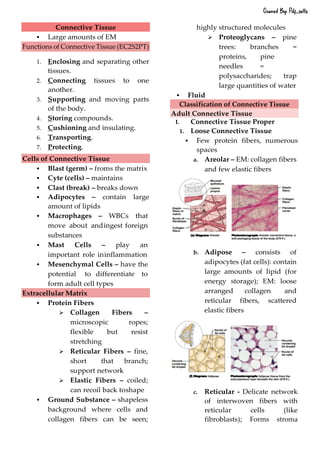
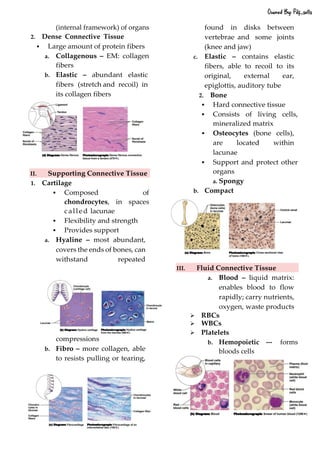
This document defines and describes the four main types of tissues in the human body - epithelial, connective, muscular and nervous tissue. It provides detailed information on the classification, structure and functions of each type of tissue. The key roles of tissues include protection, connection, support, movement and coordination within the body.