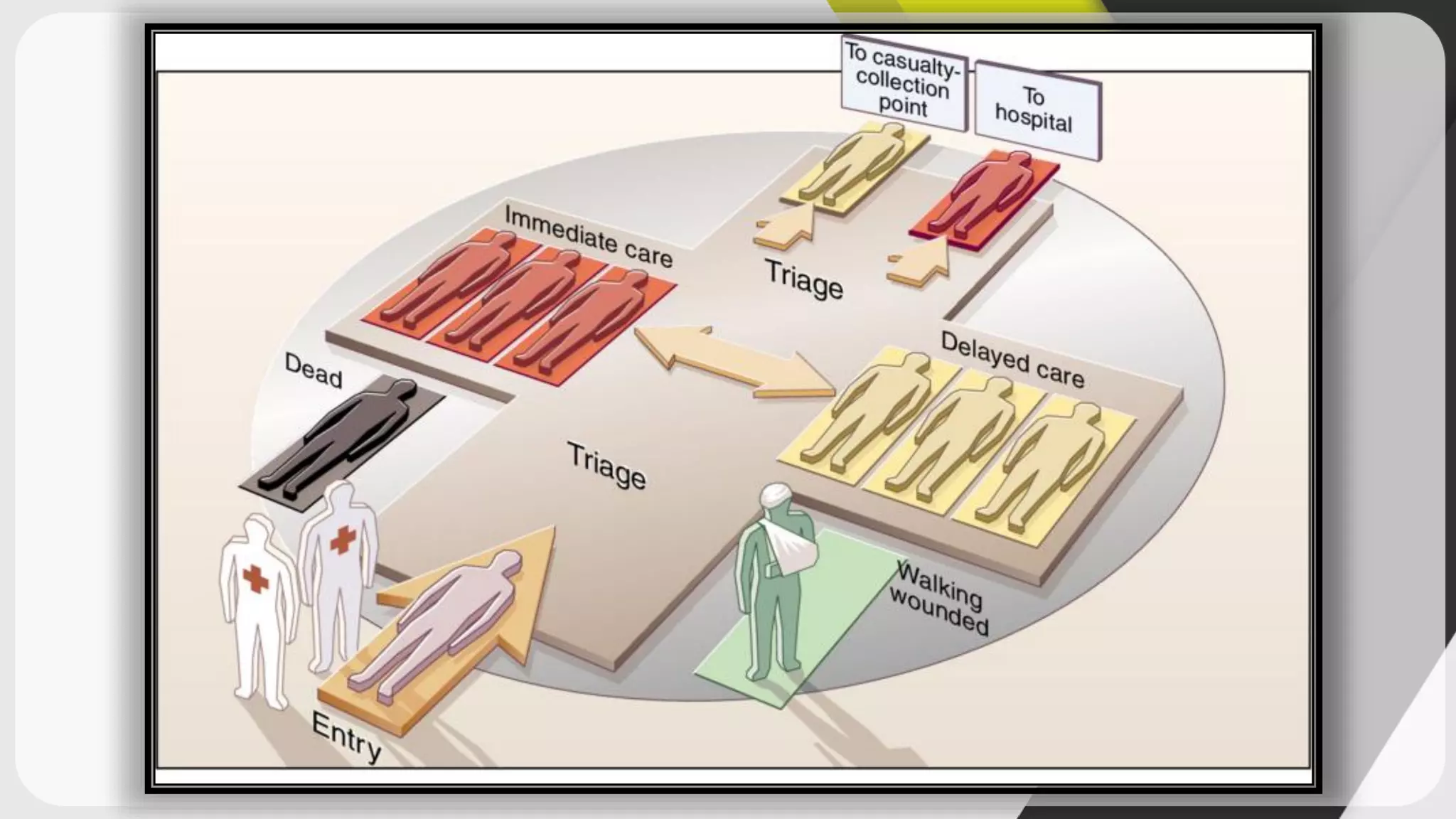
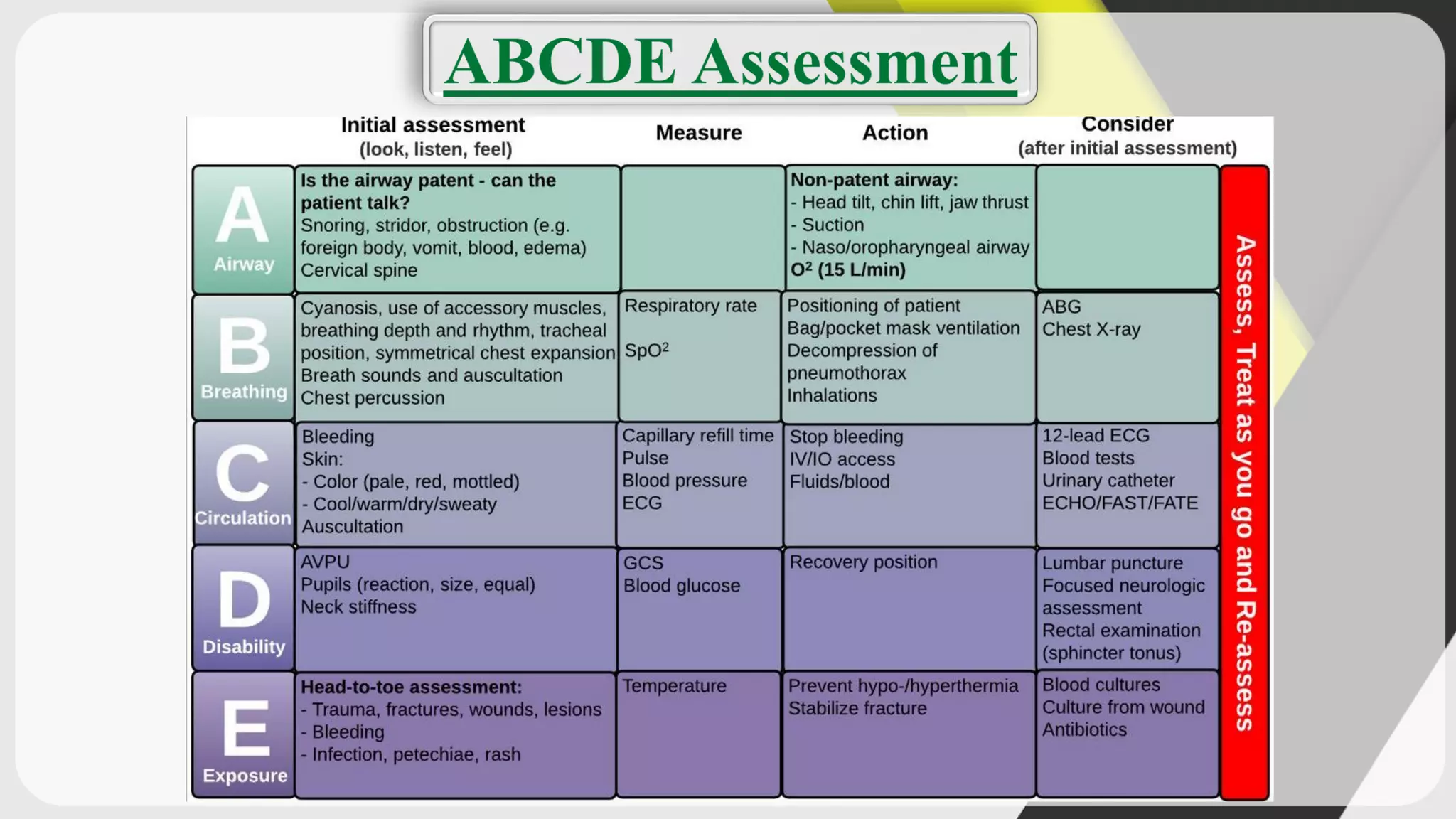
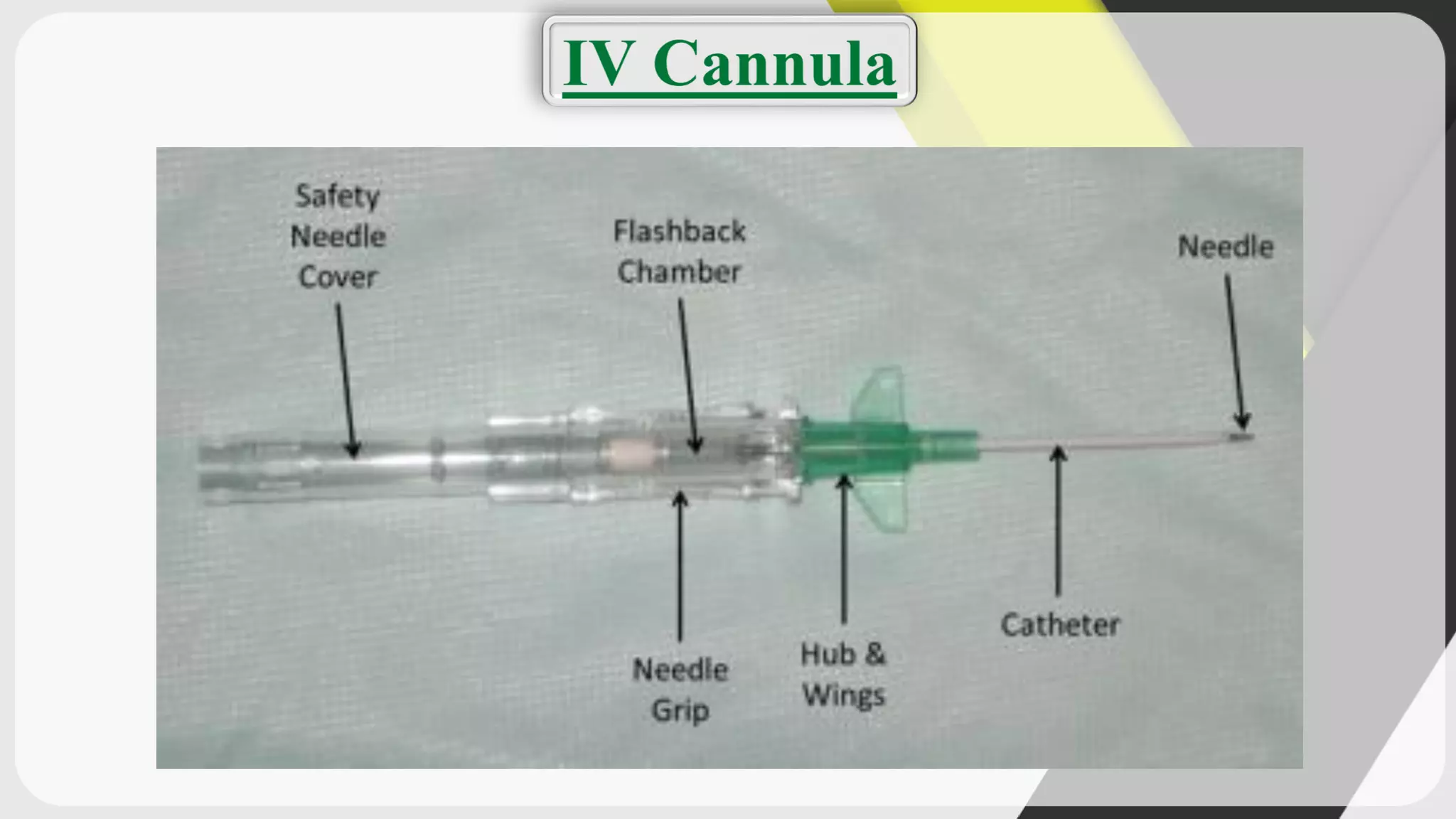
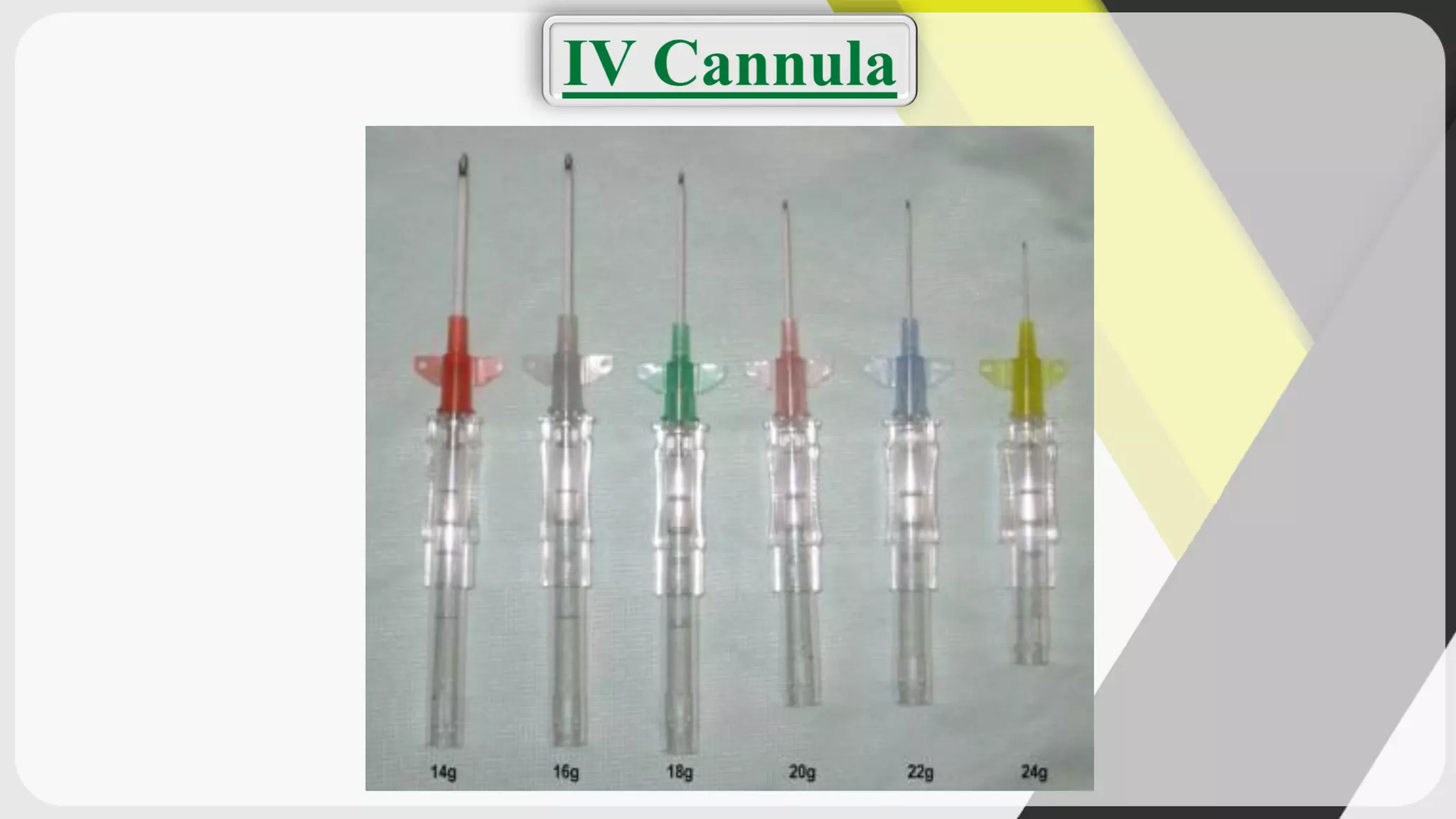
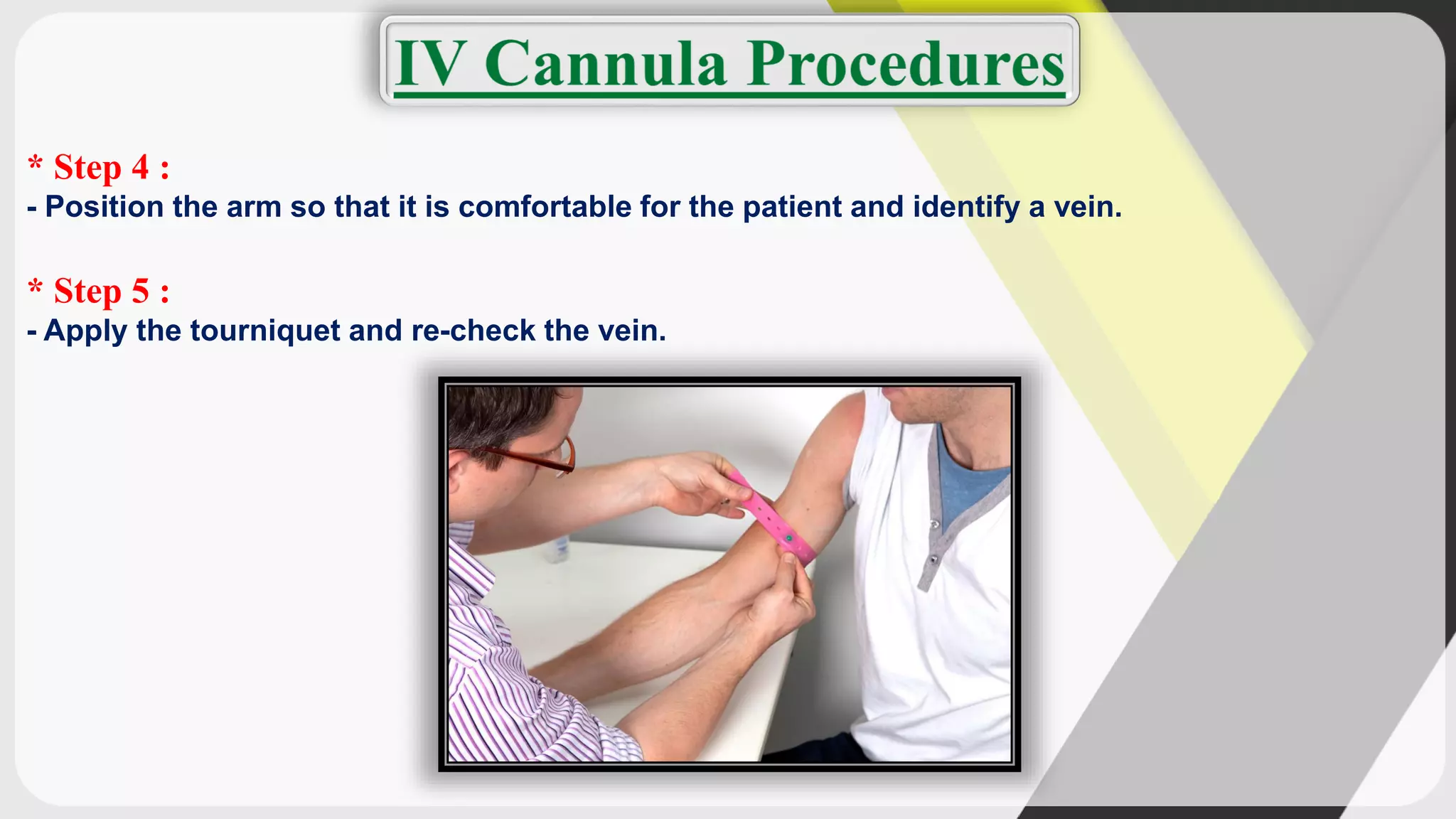
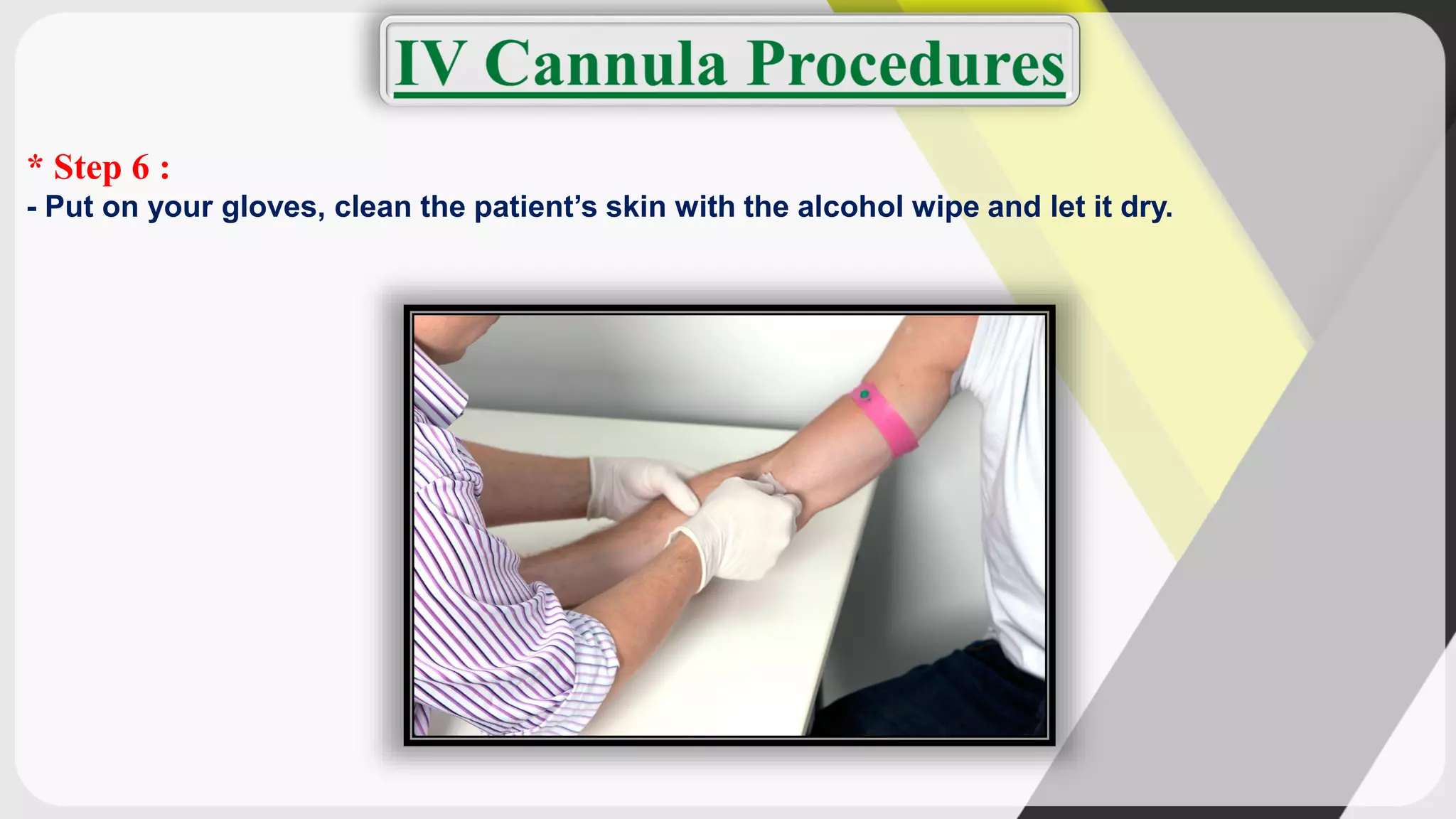
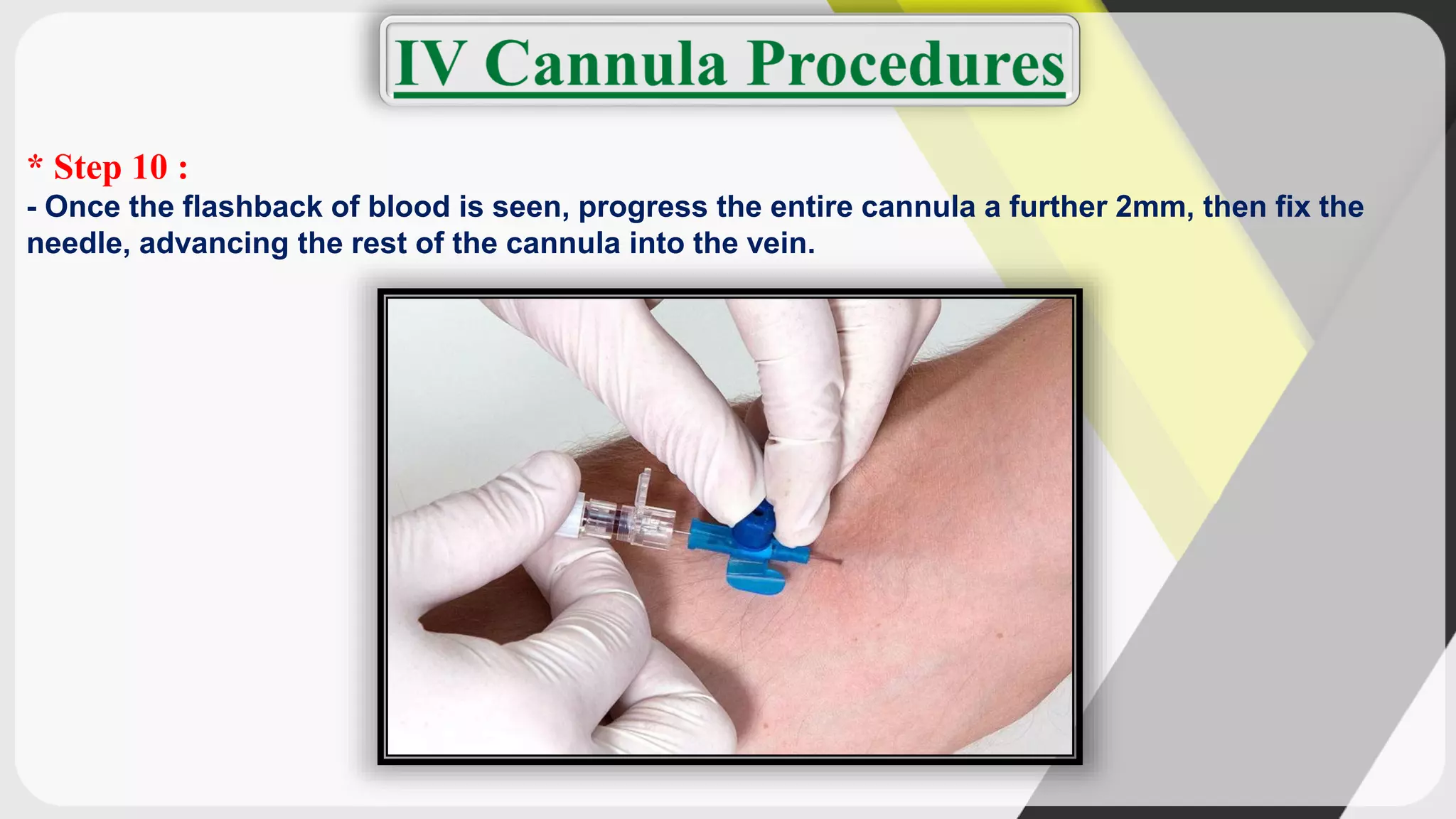
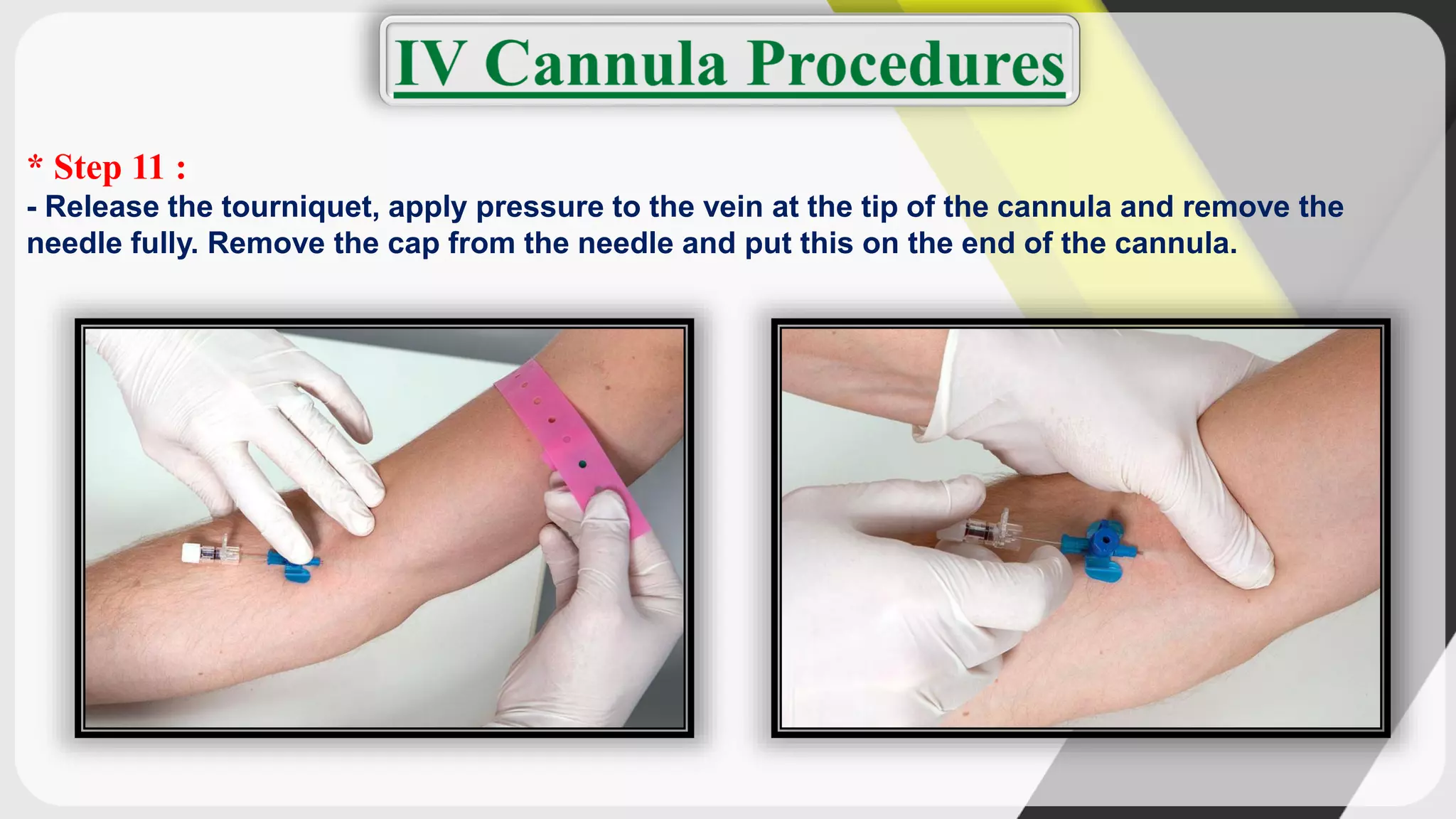
Triage is the process of prioritizing patients' treatment based on the severity of their condition. There are four categories ranging from red/immediate for life-threatening conditions to black/expectant for those who are dead. The ABCDE method is used to assess airway, breathing, circulation, disability, and exposure during triage. Intravenous cannulation involves inserting a tube into a patient's vein for infusions. The procedure has 15 steps including preparing equipment, identifying a vein, inserting the cannula, securing it, and checking for proper placement.