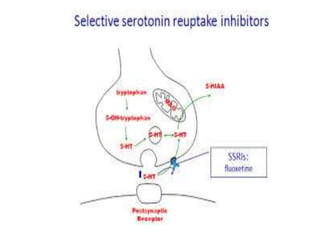
Serotonin is a monoamine neurotransmitter that is synthesized from tryptophan. It acts through multiple receptor subtypes. Serotonin is found primarily in the gastrointestinal tract, platelets, and central nervous system. It plays important roles in mood, cognition, sleep, and other physiological processes. Dysregulation of the serotonin system is implicated in depression, anxiety, migraine, nausea/vomiting, and other conditions treated with drugs that enhance serotonin signaling or block certain receptor subtypes.