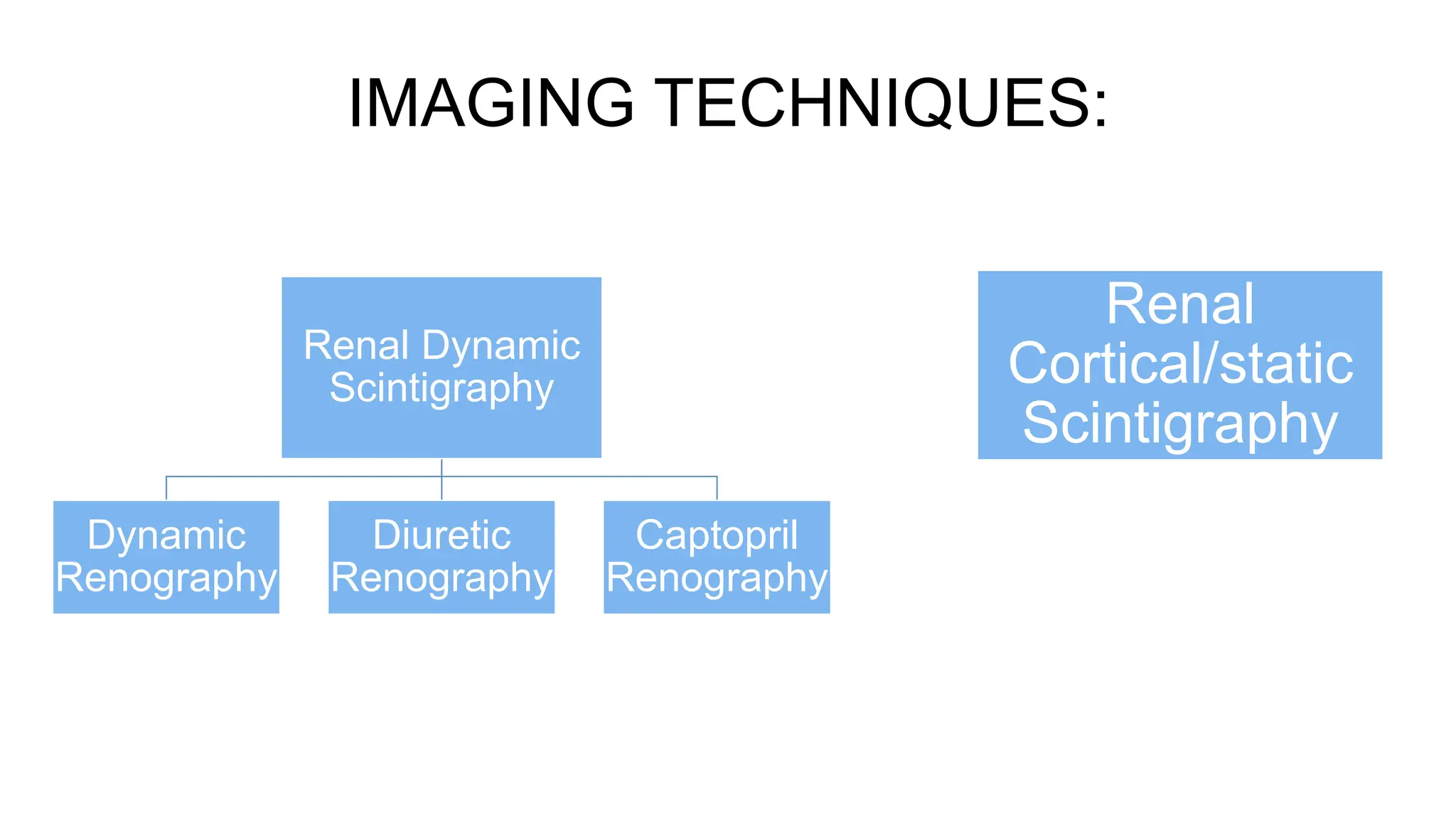
This document summarizes renal scintigraphy, which uses radionuclides and gamma camera imaging to evaluate kidney function. It describes the gamma camera components, patient positioning, common radiotracers like 99mTc-DTPA and 99mTc-DMSA, and imaging techniques including dynamic and static renography. Dynamic renography with 99mTc-MAG3 is useful to evaluate obstruction, function post-drainage, and reflux. Diuretic renography can distinguish dilation from obstruction. Captopril renography evaluates for renal artery stenosis. Static renal scintigraphy with 99mTc-DMSA assesses scarring and function.