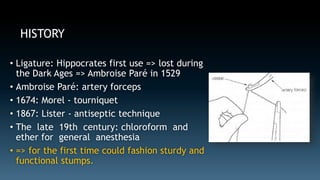
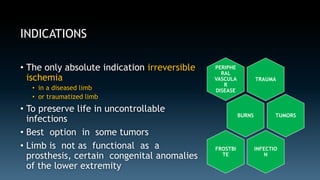
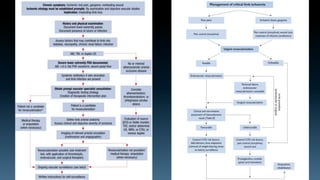
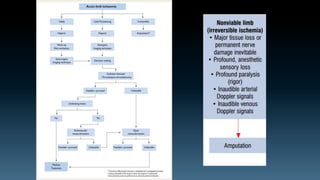
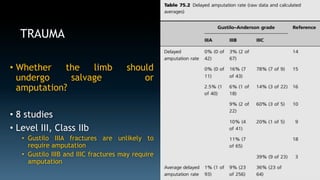
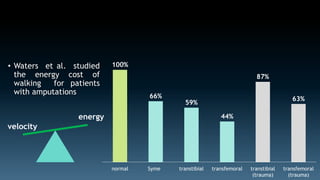
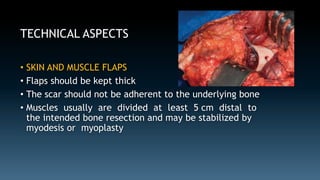
The document discusses the history and principles of amputations. It covers indications for amputations including peripheral vascular disease, trauma, infections and tumors. Key points include determining the appropriate amputation level by balancing function versus complications, and employing techniques like rigid dressings and early prosthesis to aid healing and rehabilitation. The goal of amputation is to remove non-viable tissue while preserving maximum function through prosthetics.