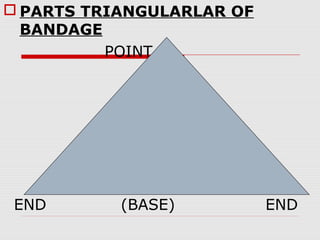
Bandaging involves covering wounds or injuries to provide support, immobilization, and protection. Common bandage materials include cotton, gauze, and elastic bandages. Proper bandaging techniques such as starting from below and applying even pressure are important to avoid complications. Common types of bandages include triangular bandages, roller bandages, and special bandages like T-bandages. Slings and splints are also used to immobilize injured limbs and provide support.