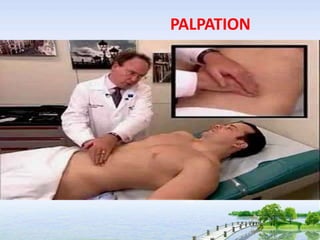
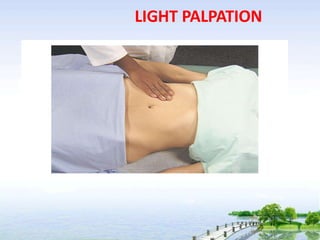
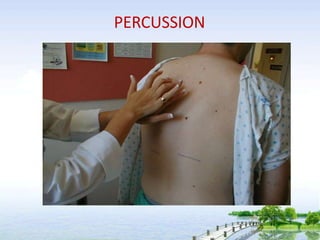
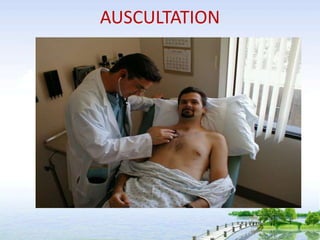
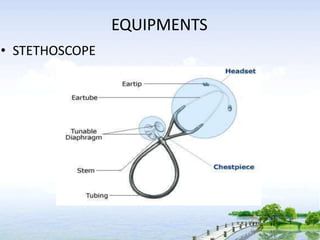
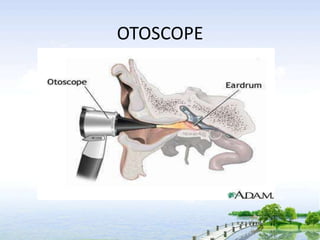
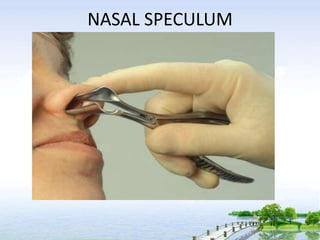
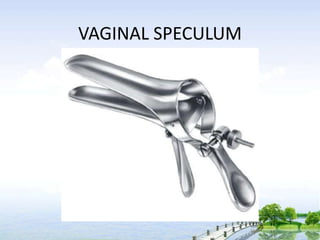
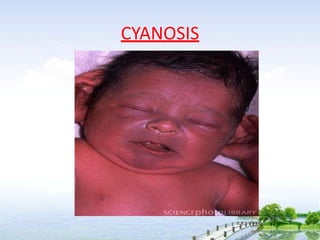
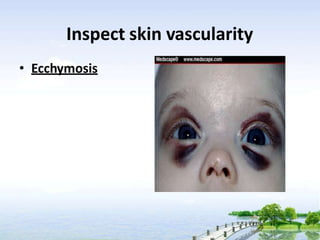
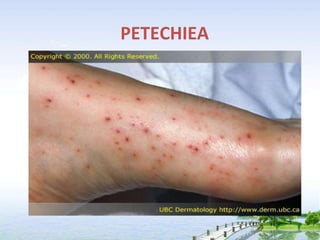
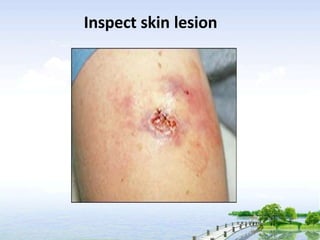
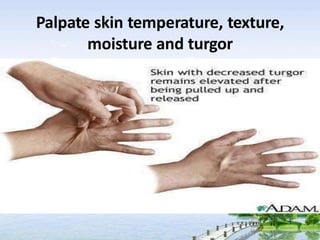
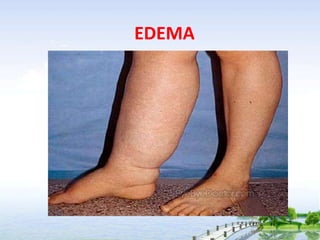
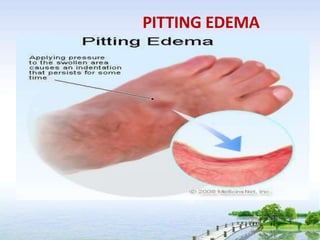
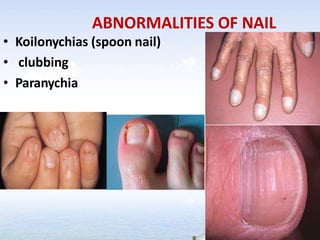
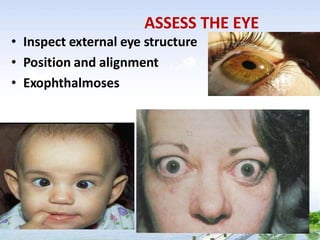
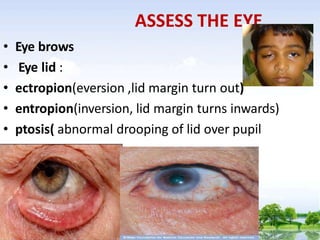
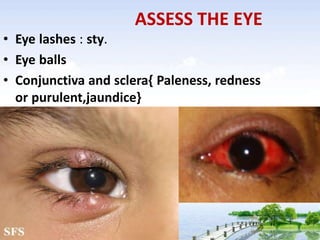
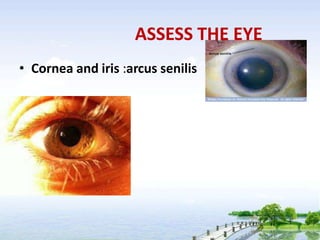
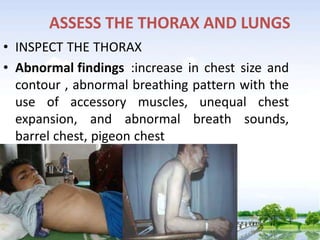
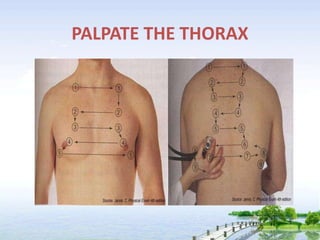
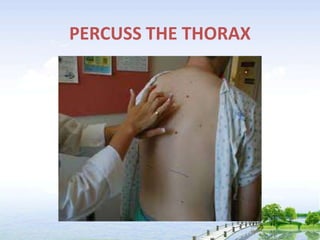
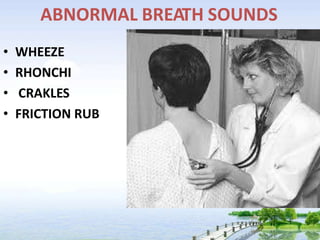
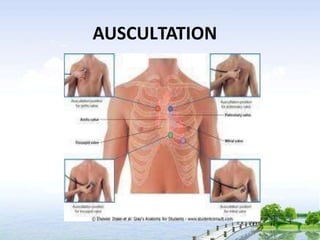
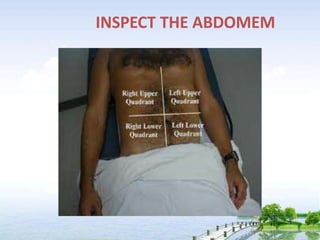
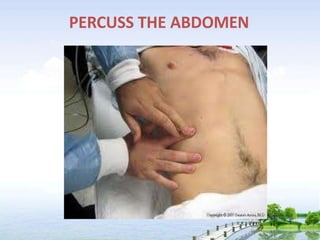
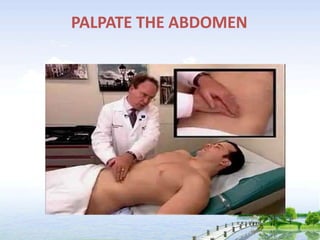
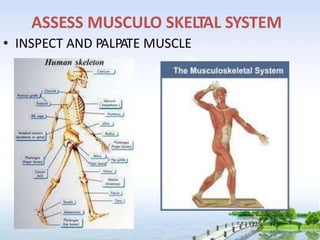
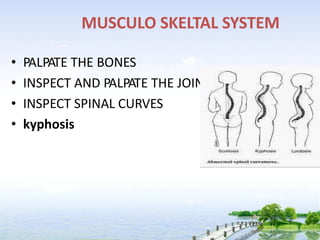
The document outlines the comprehensive procedures and techniques involved in conducting a physical examination, including inspection, palpation, percussion, auscultation, and various assessments of the body's systems. It details the necessary equipment, patient preparation, and the systematic evaluation of different body parts, emphasizing factors such as vital signs, skin conditions, and neurological assessment. Additionally, it provides guidelines for aftercare and documentation following the examination.