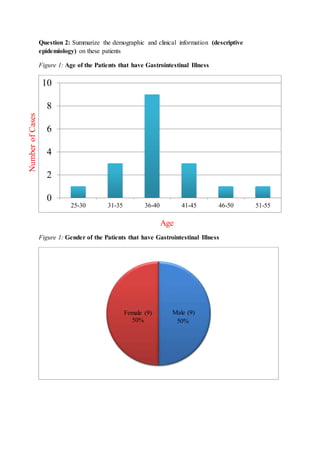
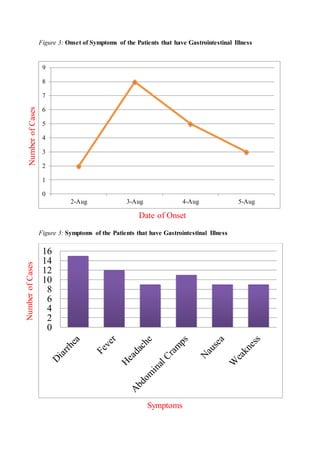
The document describes the initial steps that would be undertaken to investigate a foodborne disease outbreak:
1. Detect the outbreak through public health surveillance methods like reports of illnesses.
2. Define cases using a case definition and find related illnesses by interviewing sick individuals.
3. Generate hypotheses about the outbreak source using epidemiological data, traceback investigations, and food/environmental testing.