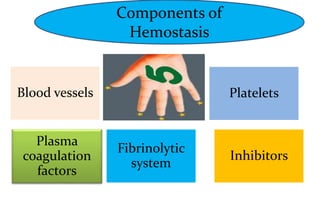
This document discusses hemostasis, which is the biological process that controls bleeding at the site of injured blood vessels. It summarizes the key components and steps of hemostasis, including:
1. Vasoconstriction of injured blood vessels to reduce blood flow and platelet plug formation via adhesion and aggregation of platelets at the injury site.
2. Activation of the coagulation cascade through intrinsic and extrinsic pathways leading to thrombin generation and fibrin clot formation to strengthen the platelet plug.
3. Fibrinolysis by the plasminogen system which acts to dissolve clots when healing is complete to restore blood flow.