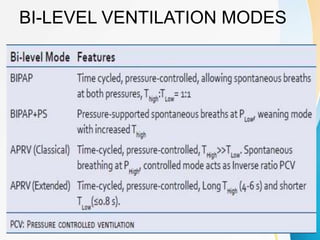
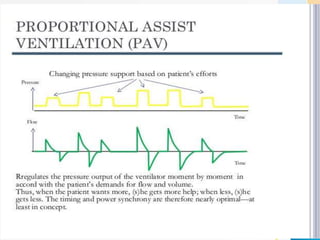
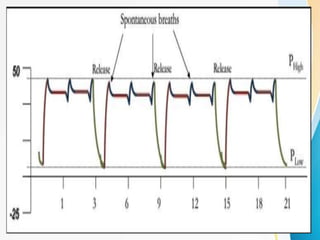
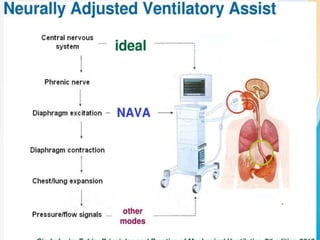
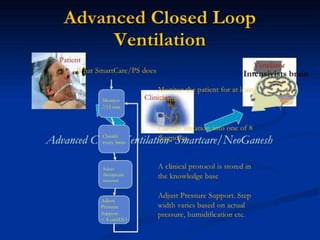
The document discusses several newer modes of mechanical ventilation that aim to improve patient-ventilator synchrony and reduce ventilator-induced lung injury compared to traditional open-loop modes. These include modes that provide dual control within or between breaths, target a minimum tidal volume, proportionally assist patient effort, and use the diaphragm's electrical activity to synchronize ventilation. The document also describes a "smart" closed-loop mode that aims to mimic clinical weaning protocols.