This document provides an overview of mechanical ventilation including:
- Indications for mechanical ventilation including respiratory and cardiac failure.
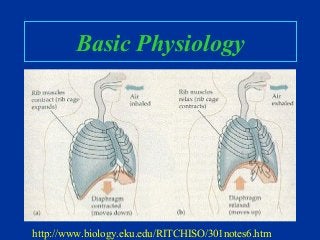
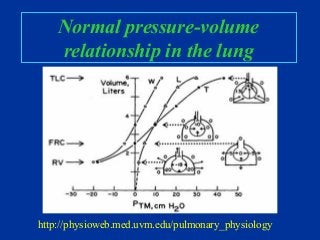
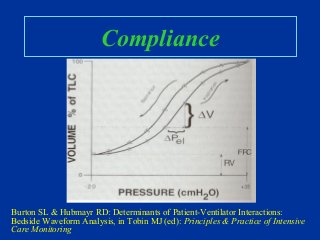
- Basic anatomy and physiology of ventilation including the roles of airways, alveoli, and pressures.
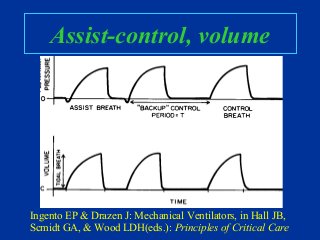
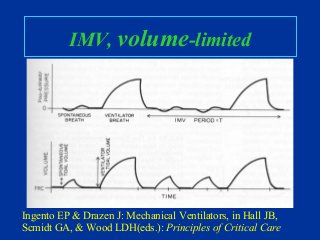
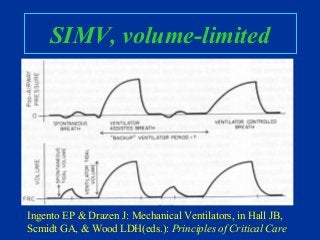
- Common modes of ventilation like assist-control, IMV, SIMV and their characteristics.
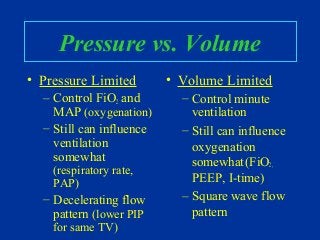
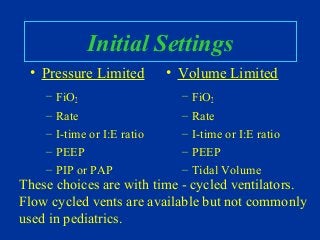
- Factors to consider when selecting initial settings like rate, pressures, and tidal volumes.
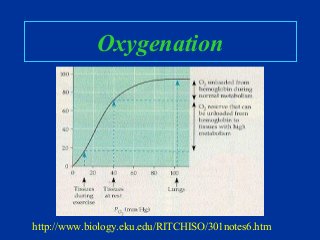
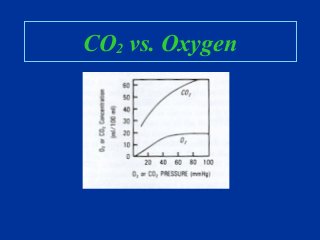
- How to adjust settings to impact oxygenation and ventilation.
- Potential problems that can arise with mechanical ventilation.