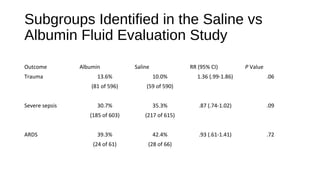
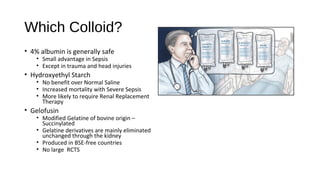
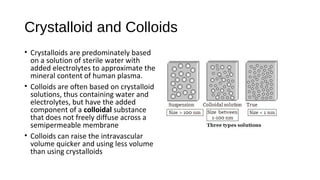
This document discusses intravenous (IV) fluid choice from an intensive care perspective. It begins by introducing IV fluids as a cornerstone treatment in emergency and intensive care medicine and discusses the debate around the relative safety of different IV fluid formulations. It summarizes the findings of several large randomized controlled trials that compared colloids to crystalloids and found increased risks of harm with some colloids. The document analyzes the safety of different IV fluid options like albumin, hydroxyethyl starches, and crystalloids based on evidence from major trials. It concludes that normal saline is generally the default fluid but that more physiological crystalloids may be preferable in some situations like burns or metabolic acidosis.



![Safety of Colloids
• It has been assumed over the past 60 years that both colloids and crystalloids are safe
and effective means of intravenous fluid resuscitation
• The safety of colloids was first questioned by a rudimentary meta-analysis performed by
Velanovich in 1989. (1)
• Subsequently in the BMJ in 1998 a systematic review questioned the safety of colloids in
general[2] and a Cochrane Review in 1998, questioned specifically the safety of albumin.
[3]
• This can only be resolved by a large randomised control trial
1. Velanovich V. Crystalloid versus colloid fluid resuscitation: a meta-analysis of mortality. Surgery.
1989;105:65-71
2. Schierhout G, Roberts I. Fluid resuscitation with colloid or crystalloid solutions in critically ill
patients: a systematic review of randomized trials. BMJ. 1998;316:961-964.
3. Cochrane Injuries Group Albumin Reviewers. Human albumin administration in critically ill
patients: systematic review of randomised controlled trials. BMJ. 1998;317:235-240](https://image.slidesharecdn.com/ivfluidchoice-anicuperspective-140416221233-phpapp02/85/IV-Fluid-Choice-An-ICU-Perspective-6-320.jpg)