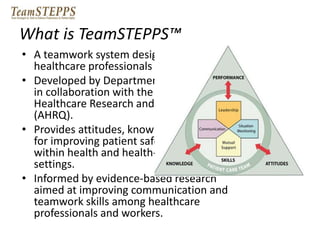
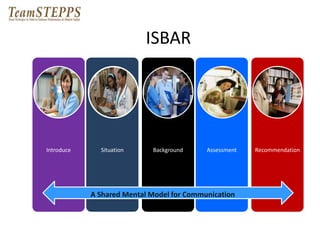
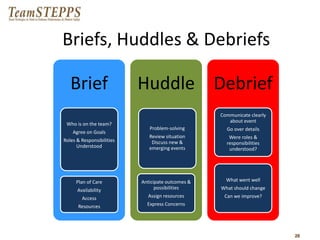
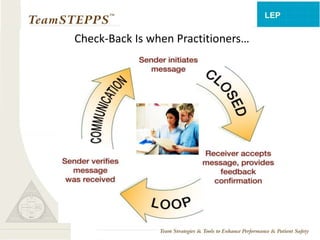
This document provides information on interprofessional education (IPE), including definitions, core competencies, rationale, implementation strategies, and tools. It defines IPE as occurring when two or more professions learn about, from and with each other to improve collaboration and quality of care. The document outlines the core IPE competencies of roles/responsibilities, values/ethics, communication, and teamwork. It emphasizes that change is difficult but can be achieved through forming inclusive coalitions, attaining clear goals, and building on small successes. A variety of teaching methods are presented, including case conferences, shadowing, and interprofessional research.

![Introduction to IPE
Here are my ideas about introduction to
IPE/IPCP and Collaborative Practice – SCK
[This slide will be deleted]](https://image.slidesharecdn.com/ipenutsandboltssck-140901103314-phpapp02/85/Interprofessional-Education-and-Practice-Nuts-and-Bolts-for-Teaching-IPE-2-320.jpg)

















![Facilitation Goals
• Orient learners to goals of the session
• Prompt learners to discuss their observations
• Encourage a non-judgmental environment
• Make interprofessional learning explicit (e. g. let’s
get the [discipline] view of client’s needs)
• Inquire about what is missing and where might
we find it?
• Capture teachable moments
• Prompt self-reflection
• Encourage closure and final case/topic
determinations](https://image.slidesharecdn.com/ipenutsandboltssck-140901103314-phpapp02/85/Interprofessional-Education-and-Practice-Nuts-and-Bolts-for-Teaching-IPE-20-320.jpg)