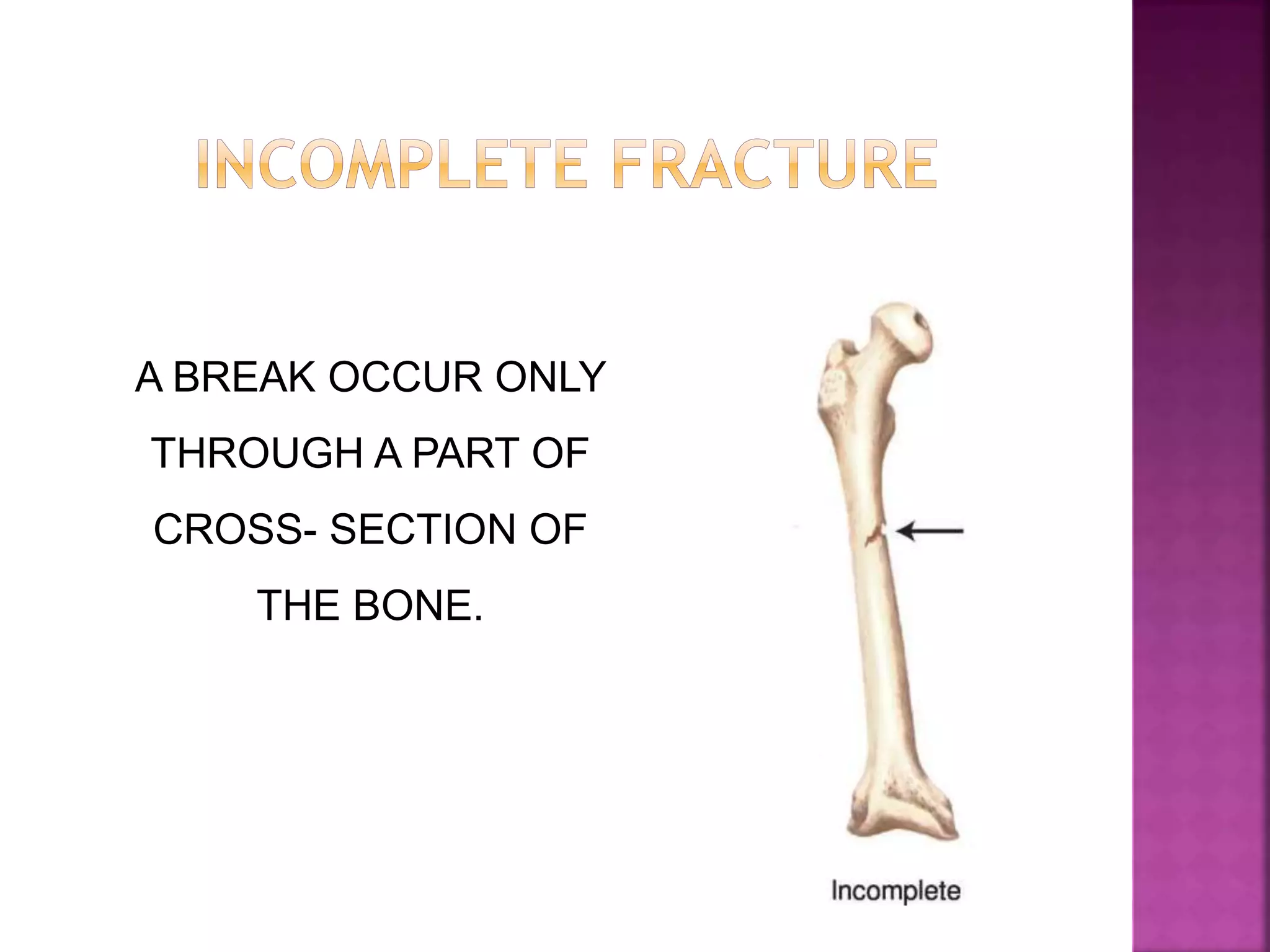
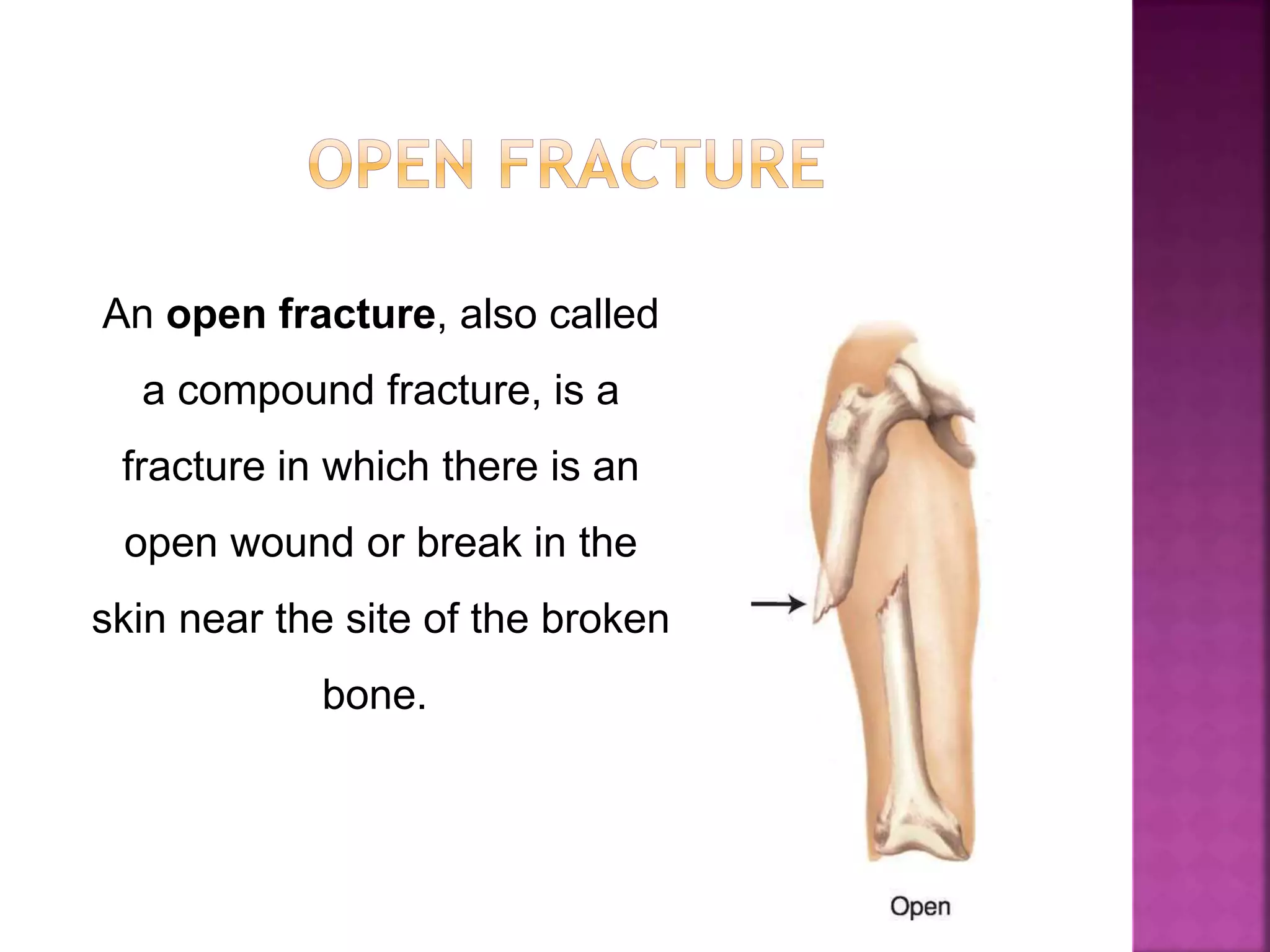
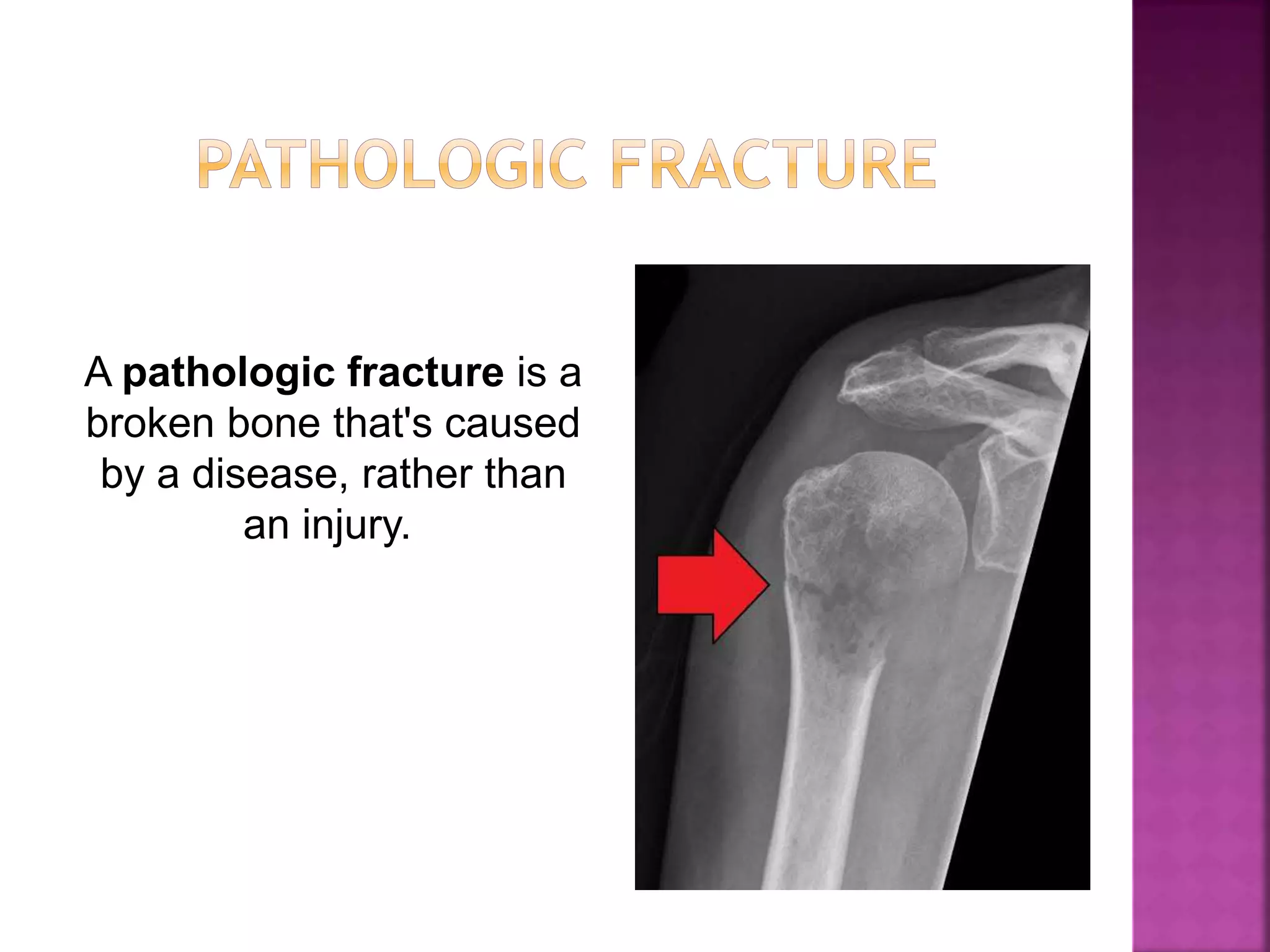
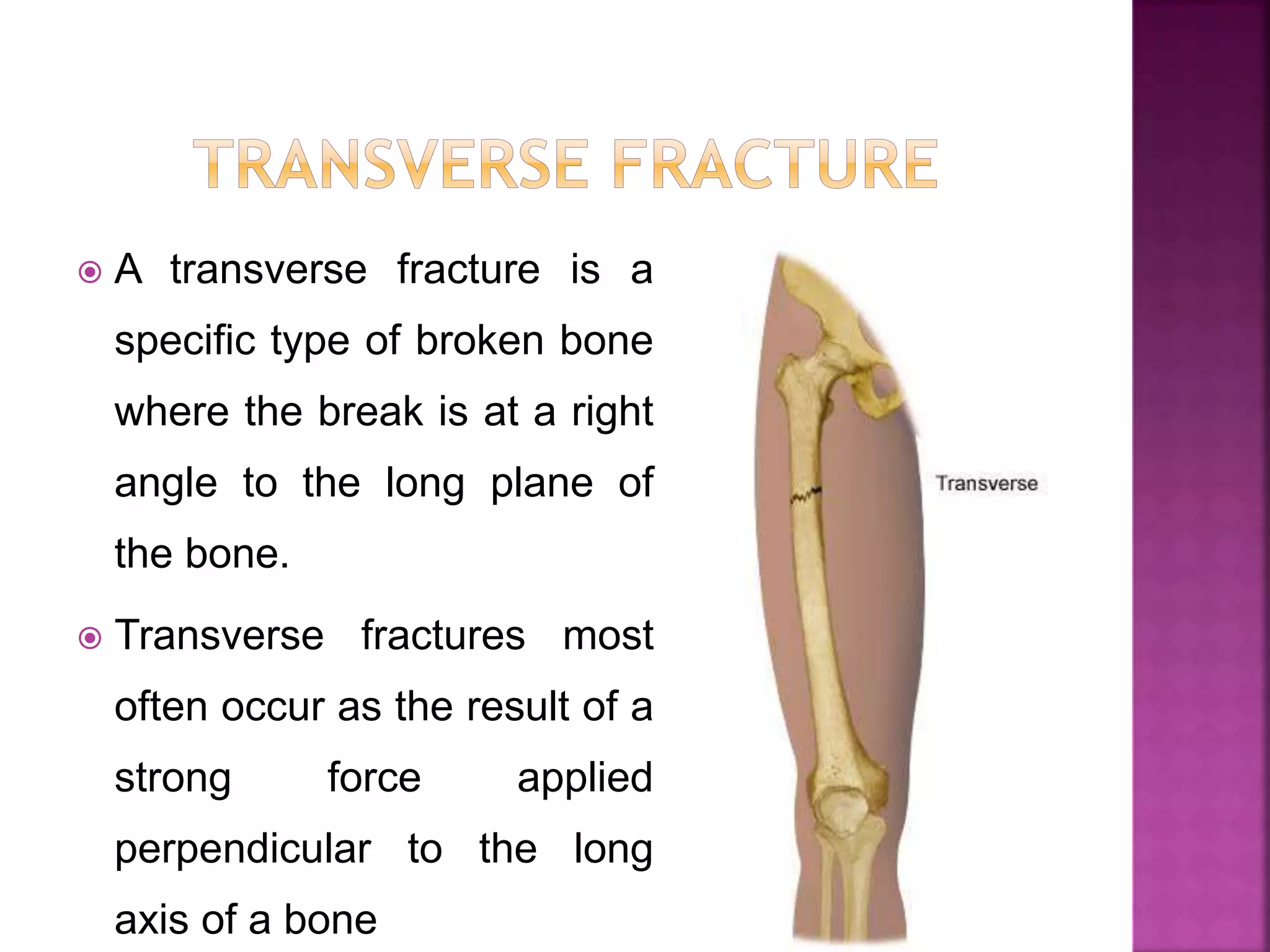
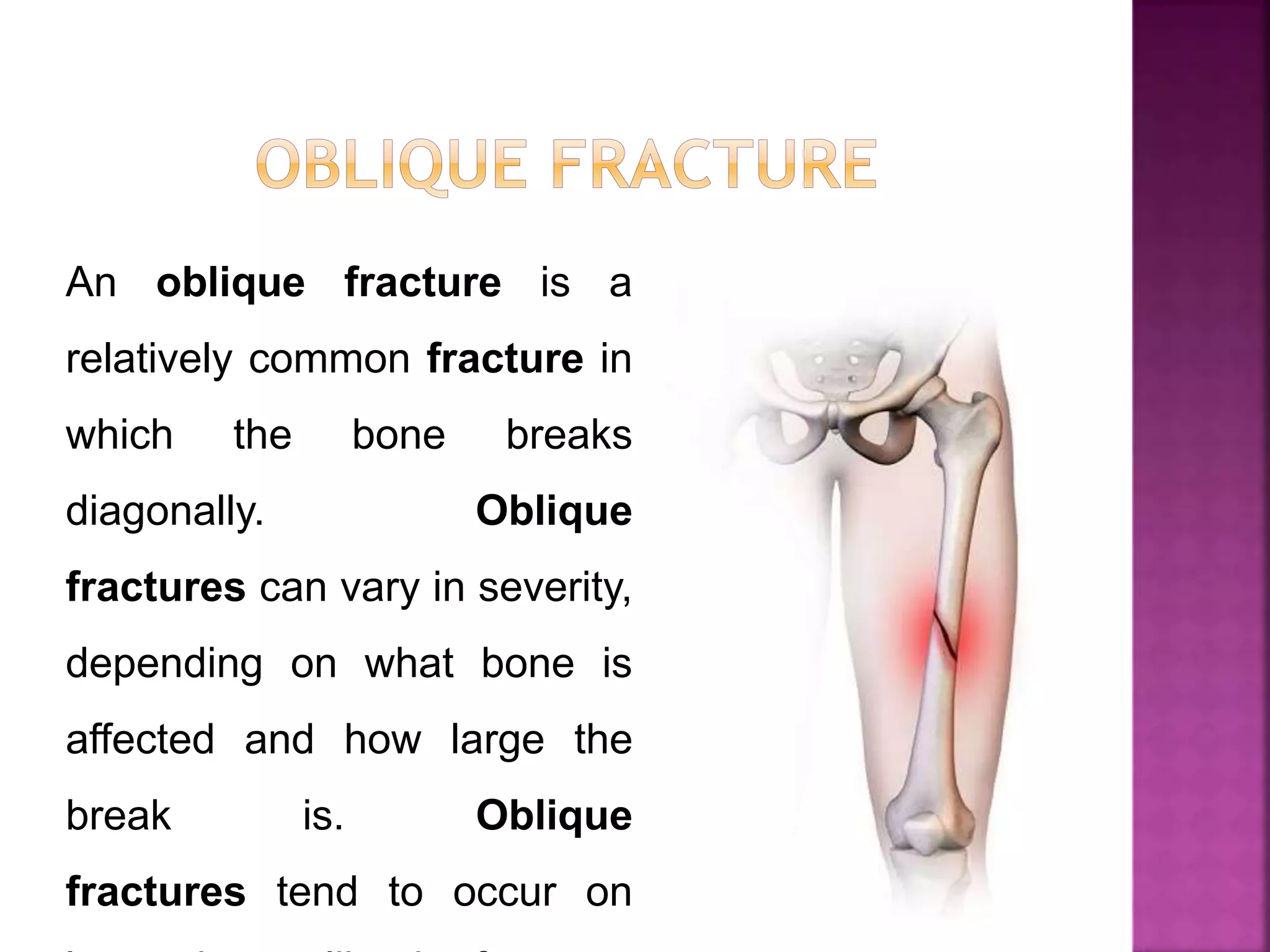
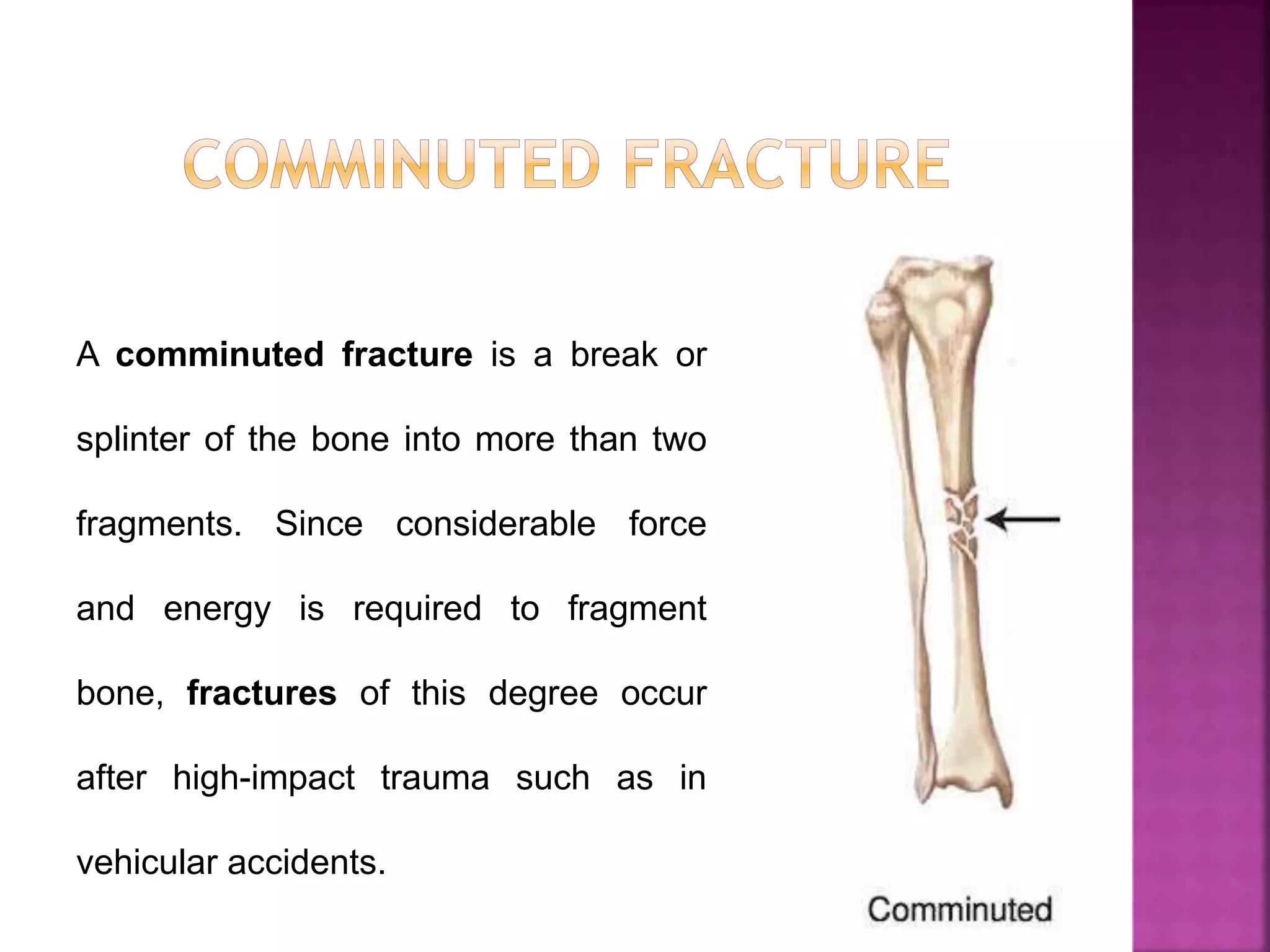
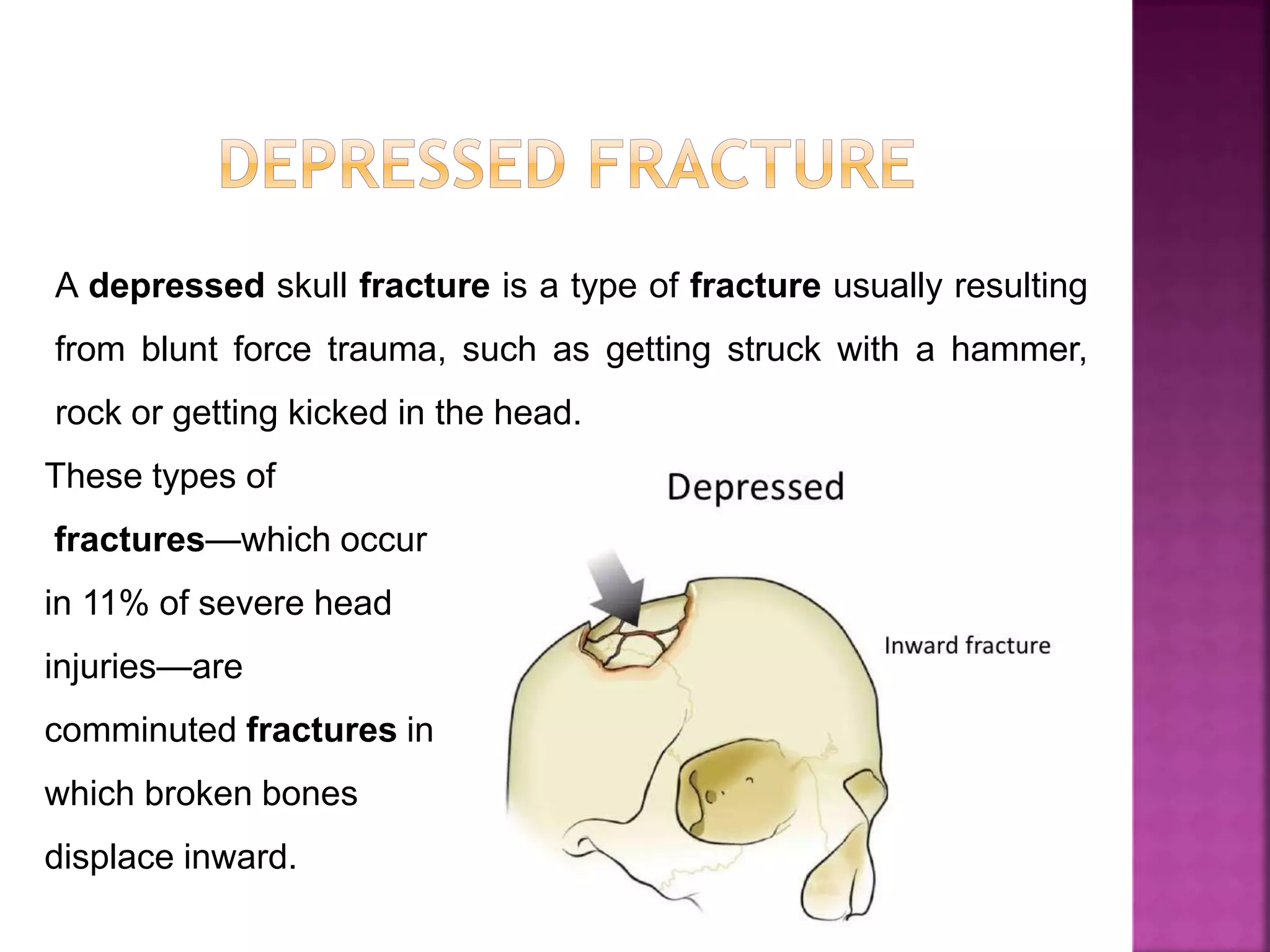
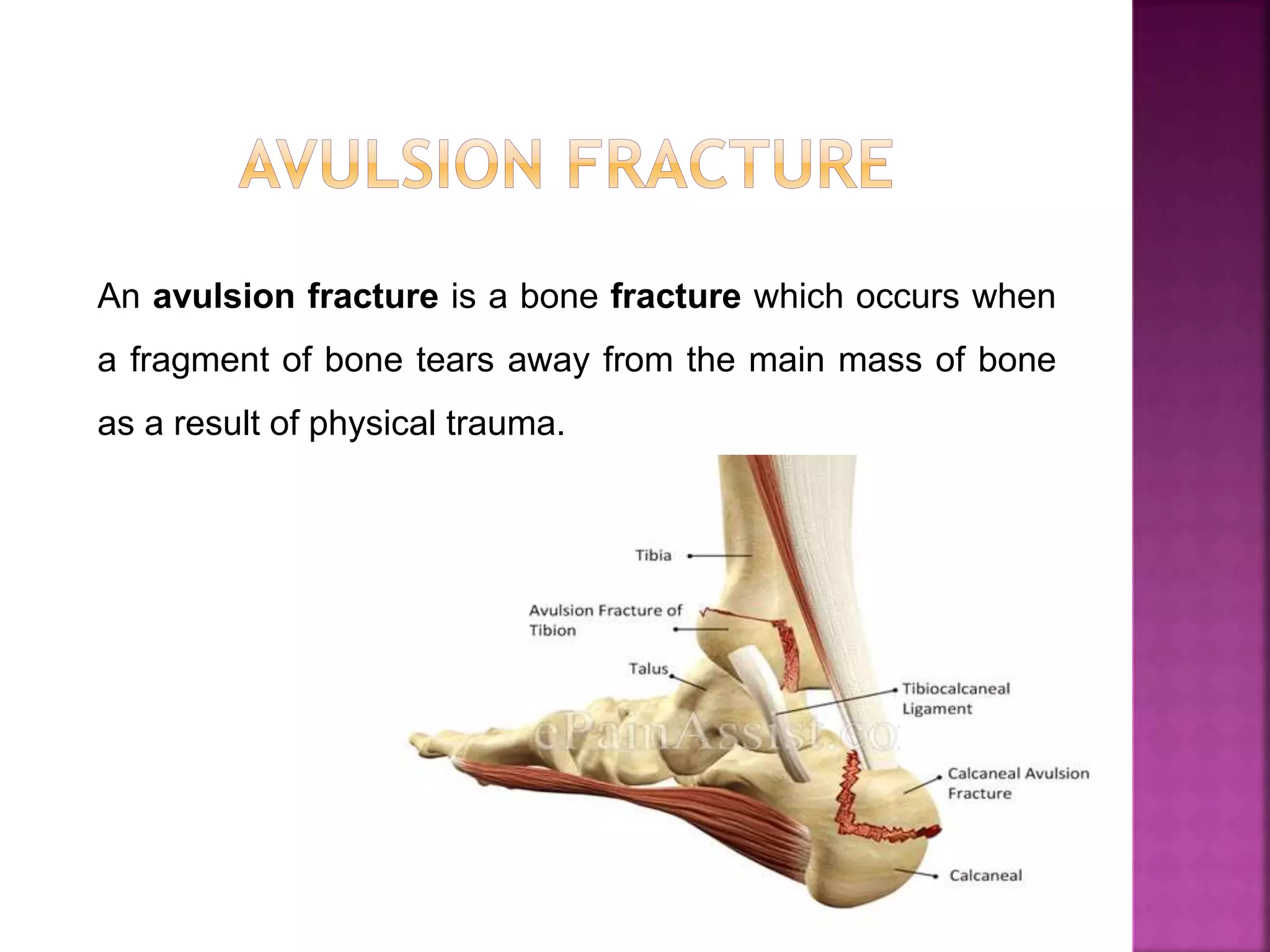
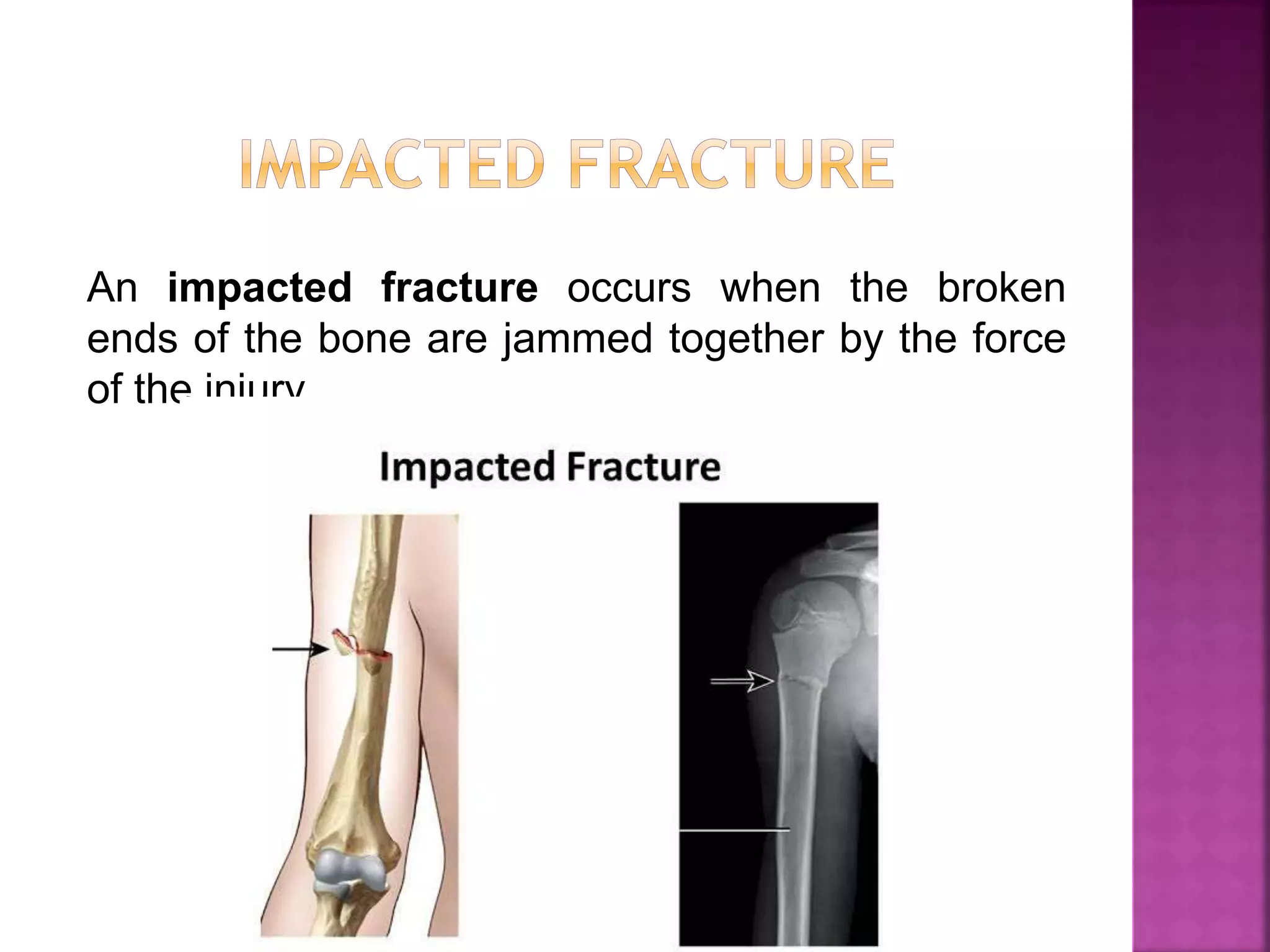
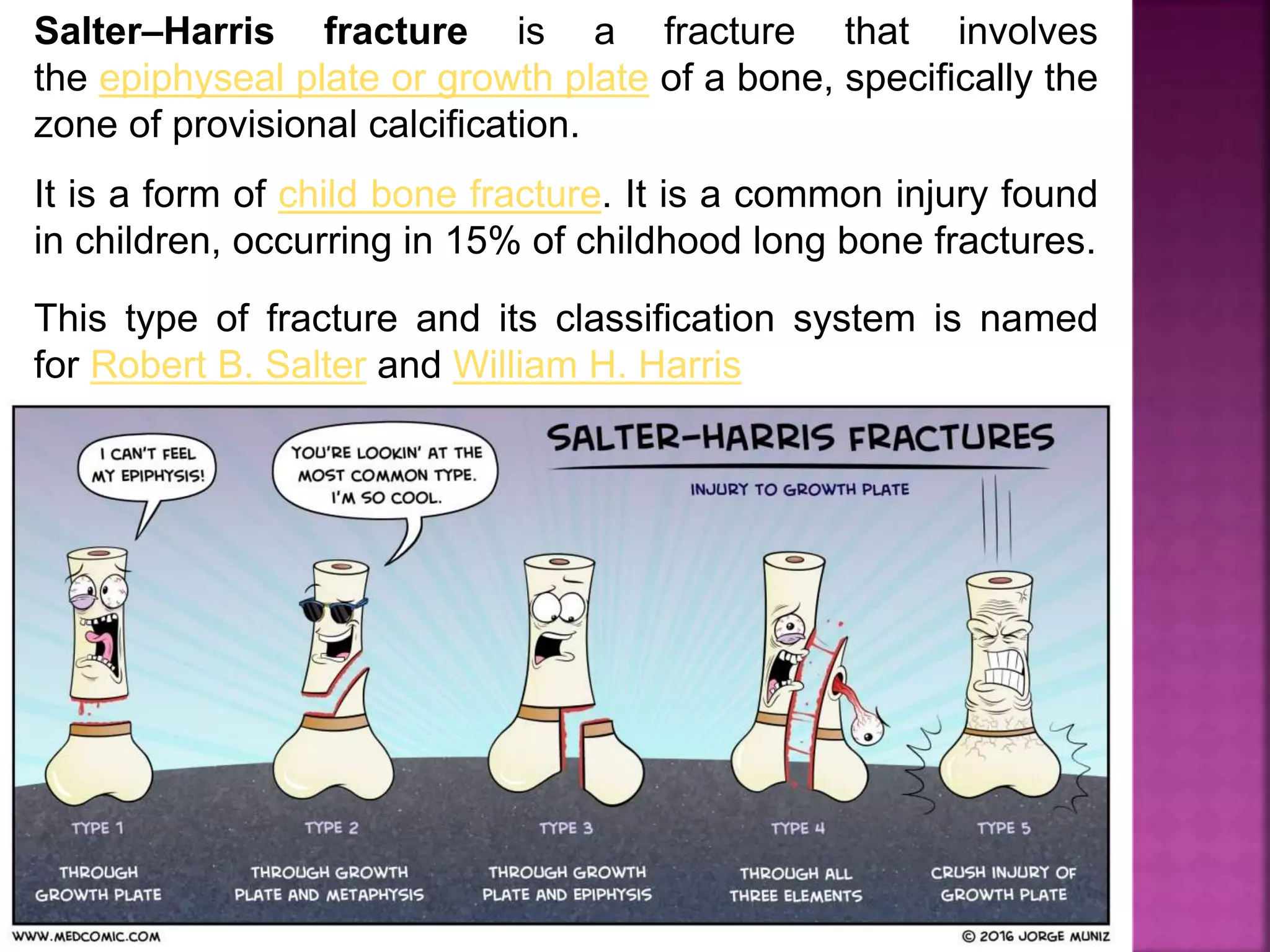
The document provides an overview of bone fractures, defining them as broken bones that can vary from minor cracks to complete breaks. It categorizes fractures into several types, including complete, incomplete, open, closed, pathological, and specific fractures such as greenstick, transverse, oblique, and comminuted. Additionally, it touches on the causes, mechanisms, and initial management steps for treating fractures.