The document provides information about euthanasia, including:
- Euthanasia involves intentionally ending a life to relieve suffering, and can be active (e.g. lethal injection) or passive (e.g. withdrawing life support).
- It outlines different types like voluntary (patient consent), involuntary (without patient consent), and assisted suicide (patient self-administers lethal drugs with help).
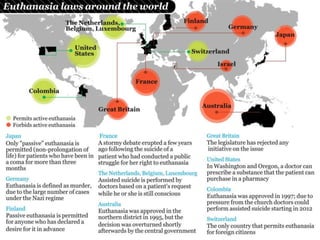
- Laws about euthanasia vary globally, with some countries and US states legally allowing it under specific conditions like terminal illness and consent. Most religions disapprove due to beliefs that only God can end a life.
- Two cases discussed are Gloria Taylor, who fought for the right to