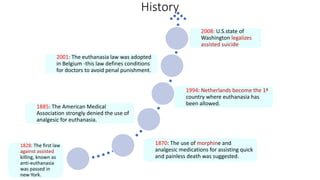
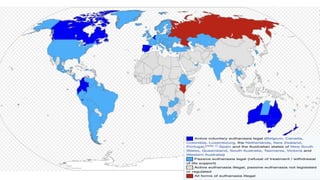
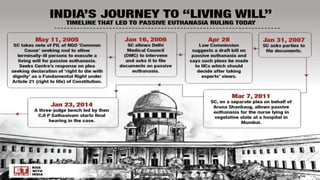
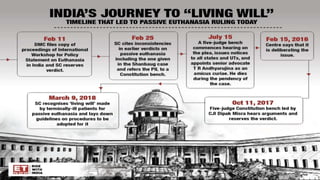
The document provides an extensive overview of euthanasia, including its definitions, historical context, types, and legal status across various jurisdictions, with a focus on Indian law. It outlines debates surrounding euthanasia's morality, religious perspectives, and the legal framework regarding the right to die and advance directives in India as of 2023. Additionally, it discusses the conditions under which euthanasia and assisted suicide are permissible and the processes involved in decision-making for patients unable to consent.